What is Arthrogryposis?
Page Contents
It is a rare form of non-progressive congenital neuro-musculo-skeletal disorder that affects the bones and joints of an individual. An individual affected by this condition suffers from multiple joint contractures, fibrosis and muscle weakness.
The term “Arthrogryposis” has its origins in Greek, and denotes ‘curved or hooked joints.’ The disease is also called arthrogryposis multiplex congenita or AMC.
Arthrogryposis Epidemiology
The occurrence of AMC is rather rare. Only 1 out of 3000 people gets affected by this disorder. Amyoplasia is the most common form of this disease and is observed in nearly 43% of all reported cases. A small section of the population is affected by problems of the respiratory muscles.
Arthrogryposis Types
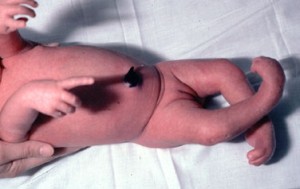
Several known subgroups of AMC exist, with varying causes, signs and symptoms. In some cases, only a few joints are affected and the individual may have nearly complete range of motion. Amyoplasia, the most common variety of AMC, affects a person’s wrists, hands, shoulders, elbows, hips, knees and feet. In most severe cases, almost every joint of the body is involved, including one’s jaw and back. The contractures are also often accompanied by weakness of muscles, which further hinders smooth movement. AMC is usually symmetrical, involving all 4 extremities with some variations.
Picture 1 – Arthrogryposis
The various types of AMC are mentioned below:
- Arthrogryposis multiplex caused by muscular dystrophy
- Arthrogryposis epileptic seizures and migrational brain disorder
- Arthrogryposis ectodermal dysplasia and other anomalies also referred to as Trichooculodermovertebral syndrome, Cote Adamopoulos Pantelakis syndrome, Alves syndrome and TODV syndrome
- Arthrogryposis-like disorder, also called Kuskokwim disease
- Arthrogryposis IUGR thoracic dystrophy, also referred to as Van Bervliet syndrome
- Arthrogryposis multiplex congenita CNS calcification
- Arthrogryposis-like hand anomaly and sensorineural deafness
- Gordon Syndrome, also referred to as Distal Arthrogryposis, Type 2A
- Arthrogryposis multiplex congenita distal or AMCD also known as Arthrogryposis multiplex congenita, distal, x-linked or AMCX1 and Arthrogryposis spinal muscular atrophy
- Arthrogryposis multiplex congenita, distal type 2B, also called Freeman-Sheldon syndrome variant
- Arthrogryposis multiplex congenita neurogenic type or AMCN; this type of Arthrogryposis Multiplex Congenita has been associated with AMCN gene on the locus 5q35 and is known by various synonyms such as Arthrogryposis multiplex congenita pulmonary hypoplasia
- Illum syndrome, also known as Arthrogryposis multiplex congenita whistling face
- Arthrogryposis multiplex congenita, distal type 1 or AMCD1
- Oculomelic amyoplasia, also known as Arthrogryposis ophthalmoplegia retinopathy
- Arthrogryposis renal dysfunction cholestasis syndrome, which is also referred to as ARC Syndrome
Arthrogryposis Causes
Although the exact causes for the development of AMC are unknown, a number of mechanisms or responsible factors have been suggested. These include:
- Fetal hyperthermia
- Fetal vascular compromise
- Prenatal virus
- Reduced amniotic fluid
- Septum of uterus
- Developmental abnormalities of muscle and connective tissues
The causes of this condition can be subdivided into:
Extrinsic Factors
Insufficient space within the uterus can hinder normal movement of the fetus. A mother may also have an abnormally shaped uterus or the uterus may lack sufficient amounts of amniotic fluid.
Intrinsic Factors
These include:
Neurological defects
AMC may occur when the spinal cord and central nervous system are malformed. In such cases, numerous types of other conditions generally accompany AMC.
Connective Tissues
Abnormal development of bones, tendons, joints or the joint linings may lead to AMC. For instance, the tendons may not stay attached to the appropriate place in the joints. When a joint remains immobile for a long period of time, additional connective tissue starts developing around it, thereby fastening it and making joint movement difficult.
According to research, anything which prevents the normal movement of joints during the prenatal stage can lead to joint contractures. A lack of proper joint movement means that the tendons that connect to the joint are not getting stretched as they should be. The short tendons make it difficult to move the joints normally.
The major cause of AMC is akinesia or decreased fetal movements caused by fetal or maternal abnormalities. It is also associated with myopathic and neurogenic disorders. Neuropathic AMC is supposed to involve deterioration in anterior horn cell, which leads to fibrosis and muscle weakness.
In the majority of cases, AMC does not occur due to genetic reasons. It occurs only once within a family. A genetic factor can be identified in almost 30% of all cases. In such instances, the possibility of recurrence of the symptoms varies with the form of genetic disorder. A rare autosomal recessive type of this disease is also known to exist.
Other causes of Arthrogryposis include conditions that impair the nervous system, such as:
- Spina bifida
- Brain defects
- Spinal muscular atrophy
- Neuro-muscular ailments like myotonic dystropy, myasthenia gravis and multiple sclerosis
- Maternal infections at the time of pregnancy, like German measles
- Maternal exposure to certain substances which are injurious to fetus, such as alcohol, drugs or phenytoin
Arthrogryposis Signs and Symptoms
There are various common symptoms associated with the AMC group of disorders, such as:
- Clubfoot
- Flexion knee
- Skin impairment
- Cardiac disorders
- Facial deformities
- Ankle deformities
- Displaced hip joint
- Ulnar and volar wrist
- Respiratory disorders
- Spinal cord anomalies
- Genital tract abnormalities
- Internal rotation of the shoulder
- Extension and pronation of the elbow
- Muscle weakness or absence of muscles
- Externally rotated, flexed or abducted hip
- Joint immobility or restricted joint mobility
- Hand deformities, such as thumb-in-palm and fingers in a fixed flexion
Cognition and speech of the patients affected by AMC remains normal.
Arthrogryposis Diagnosis
As yet, no prenatal diagnostic mechanisms can be used to test this condition. The diagnosis of AMC is conducted shortly after birth mainly to rule out other factors. The diagnostic methods include procedures like:
- Checking of medical history
- Physical examination
- Blood tests
- X-rays
- Muscle biopsies
- Imaging studies, like Ultrasonography and CT Scans
Arthrogryposis Treatment
Although AMC is irreversible, proper treatment can greatly improve the quality of life of affected individuals. As each person has different needs and responds differently to treatments, a combination of different therapeutic measures is usually advisable. Physical therapy can include strengthening, stretching and mobility training which can greatly improve range of motion and flexion to increase mobility. Patients can also be given occupational therapy which will include splinting of the affected joints, casting and training in fine motor skills and ADL. Addressing the emotional and psychosocial implications of living life with a disability can help the person to adjust better to his or her health problems. Since mobility impairments vary in their nature, orthopedic correction should be tailored according to individual requirements. Orthopedic surgery, which can include external Ilizarov fixator or osteotomy, may be employed to mend severely affected limbs and joints as well as symptoms like:
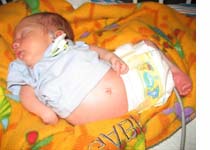
Picture 2 – Arthrogryposis Image
- Clubfoot
- Hernia repair
- Correction of unilateral hip dislocation
In these cases, surgery can significantly improve the quality of life. In most cases of AMC, however, the contractures tend to return even after operation. Tendon Release surgery can stretch the tendons and helps patients to walk on toes.
Arthrogryposis Complications
AMC may lead to the following complications:
- Scoliosis
- Abdominal hernias
- Growth retardation
- Respiratory problems
- Pulmonary hypoplasia
- Midfacial hemangioma
- Jaw and facial variations
Arthrogryposis Prognosis
AMC patients are usually aided by regular therapy and as well as in some cases with surgical intervention. The severity of the reduction of mobility of a patient does in fact influence the prognosis of the disorder. AMC is not progressive. Patients of this disease normally have healthy speech and cognition. Hence, they can live independent, productive and rewarding lives. In some cases, however, their lifespan may be altered by issues with central nervous system or heart defects. However, proper medical treatment allows a patient to live a long and healthy life in most cases.
References:
http://www.childrenshospital.org/az/Site594/mainpageS594P3.html
http://rarediseases.about.com/cs/arthrogryposis/a/121403.htm
http://www.arthrogryposis.net/
http://emedicine.medscape.com/article/941917-overview