Plantar fibromatosis is a condition that affects quite a sizeable population across the globe and is seen as cosmetically discomforting. Know what is Plantar fibromatosis and more about this condition including its causes, symptoms, diagnosis, treatment and prevention.
Plantar fibromatosis Definition
Page Contents
- 1 Plantar fibromatosis Definition
- 2 Plantar fibromatosis Synonyms
- 3 Plantar fibromatosis Incidence
- 4 Plantar fibromatosis Symptoms
- 5 Plantar fibromatosis Causes
- 6 Plantar fibromatosis Diagnosis
- 7 Plantar fibromatosis Differential Diagnosis
- 8 Plantar fibromatosis Treatment
- 9 Plantar fibromatosis Prognosis
- 10 Plantar fibromatosis Complications
- 11 Plantar fibromatosis Prevention
- 12 Plantar fibromatosis Pictures
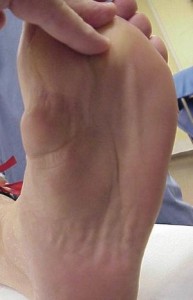
Picture 1 – Plantar fibromatosis
It is a condition characterized by formation of hard nodules or bumps beneath the skin surface on the lower region of the foot. The lesions are composed of excess fibrous tissue or collagen in the feet.
Plantar fibromatosis Synonyms
This syndrome is known by various other names like:
- Ledderhose’s Disease
- Morbus Ledderhose
- Plantar aponeurosis
Plantar fibromatosis Incidence
The condition can affect individuals of any age group. However, it is mostly detected in approximately 25% of the population segment that comprises of middle aged and senior citizens. The disorder is found to be ten times more frequent in men than women.
Plantar fibromatosis Symptoms
As aforementioned, the disorder gives rise to firm lumps under the skin of lower foot area, particularly the arch. These are hard to touch. People with these nodules may or may not experience any painful symptoms. Pain, if experienced, is largely caused due to pressure exerted on the lump by a shoe. Shoes that push against the arch press the bump and give rise to pain. Patients may also experience pain during standing or walking barefoot.
In the initial stages, the lump appears to be small in shape yet noticeable. It appears firm to the touch. Over time, the bump may grow in size. In some patients, there may be a development of multiple painful fibromas. Symptoms usually vary depending on the type of the lesion that a patient suffers from.
Plantar fibromatosis Causes
The actual cause for the development of Plantar fibromatosis is still unclear. But medical researchers have indicated some potential causes of the disease. These include,
Underlying disorders
Patients suffering from certain diseases, such as Diabetes mellitus, Epilepsy, Palmar fibromatosis, Peyronie’s disease, Liver disease and Thyroid problems, are found to suffer more from this condition.
Foot trauma
Individuals who suffer from recent foot injuries (trauma) or those who overuse their feet for long duration are also at risk from this syndrome.
Alcohol abuse
People who consume alcohol for a long period of time are also found to be susceptible to this disorder. Alcoholism is supposed to be a causative as well as aggravating agent for several foot problems.
Smoking
Long-time smokers are also seen to be at higher risk of getting this discomforting disease than non-smokers.
Genetics
Individuals with a family history of this disorder are often found to suffer from this disorder. Hence, genetic factors are supposed to be responsible for the rise of this syndrome.
Medications
Medications such as beta blockers, which are used for controlling high blood pressure, have been associated with fibrotic tissue disorders. Supplements like Chondroitin/Glucosamine and anti-seizure medications such as Phenytoin can also cause this disease. For patients of foot disorders, it is essential to consult doctors before taking any new supplements or medications.
Vitamin C
Consumption of high amounts of supplemental vitamin C can promote the manufacture of excessive collagen in the body. This can be directly responsible for Plantar fibromatosis development.
Ancestry
The development of this condition is also believed to depend on the ancestry of sufferers. People of North-European origin and Caucasian males over 70 years of age are found to be at a higher risk of getting this condition than individuals who belong to other ethnic groups.
Plantar fascia injury
According to some experts, the syndrome may also be associated to prior trauma (injuries) of the plantar fascia. Fibromas often occur after an injured fascia repairs itself after an episode of trauma. However, this cause is only speculated by podiatrists and there is no conclusive evidence to prove it as yet.
Plantar fibromatosis Diagnosis
The diagnosis of this condition is usually carried out with the aid of imaging tests like
- X-rays
- Ultrasound scans
- MRI (Magnetic Resonance Imaging) scans
In some cases, the lesions arising from the disease are misdiagnosed for other conditions like post-traumatic neuroma. This can be avoided by a biopsy of the lesion. Samples of the nodules are taken and examined in laboratories under a microscope. This lessens the chance of misdiagnosis.
In many cases, MRI tests are preferred by podiatrists over X-rays. This is due to the fact that X-rays are mainly helpful in detecting bone abnormalities and fail to identify soft tissue structures successfully. MRI scans can show the severity of the syndrome, which often involves the Aponeurosis (the flat, fibrous connective tissue layer that joins muscle to bone). Doctors also ask patients about
- Their lifestyle
- Any medications that they may be using
- Any other medical condition that they may be having
- The symptoms that they are experiencing
- Their medical history of their family
Plantar fibromatosis Differential Diagnosis
The differential diagnosis of this condition involves differentiating it from other similar disorders, such as
- Post-traumatic neuroma
- Calcifying aponeurotic fibroma
- Epithelioid sarcoma
- Extra-abdominal desmoid fibromatosis
- Fibrosarcoma
- Inclusion body fibromatosis
- Synovial sarcoma
Plantar fibromatosis Treatment
Treatment for this disorder depends on the stage of the condition and whether there are any painful symptoms. Minimal treatment is required during the initial stages, or when the lesions are small in size. Small-sized bumps can be successfully cured with non-invasive treatment.
Non-Invasive Treatment
Non-invasive treatment for the disorder involves use of:
Foot orthotics
Initial stages of the condition can be cured by preventing direct pressure over the fibromas. This can be done by using padding or operable foot orthotics like heel lifts, soft arch supports or night splints. Decreasing pressure over the fibromas can help reduce them.
Topical medications
Topical medications, such as Verapamil, are considered to be effective in decreasing the mass. Verapamil is a calcium channel blocker that is primarily used to treat problems like high blood pressure, irregular heartbeat and angina. Directly applying this drug over the mass for two times every day for several months can help cure the lesions.
Invasive Treatment
If non-invasive cure fails to improve the situation, invasive treatment can be seen as essential. Such treatment is also necessary in case of more advanced stages of the disease that involve bigger bumps on the feet. Two invasive treatment options, that are used to cure Plantar Fibromatosis, include:
Cortisone injections
Cortisone injections can be quite helpful in curing the bumps. However, they can sometimes lead to the enlargement and dispersion of the growths. If the lumps cause pain and fail to improve with non-invasive treatments, it can be removed by an operative procedure.
Surgery
Surgical intervention for this syndrome differs on the basis of the size of the growth and medical history of the patient apart from a few other factors. Operation is performed in a hospital or a surgery center under the effects of general or local anesthesia and takes about 30–45 minutes to be completed. Patients must refrain from lifting heavy loads for at least three weeks after operation.
However, the abnormal lumps might recur even after a surgical removal. There is also a possibility that patients might suffer from hammertoe and flat feet problems after operation.
Plantar fibromatosis Prognosis
Unlike Plantar fasciitis, which being a self-limiting disorder goes away in about 3-4 months, Plantar fibromatosis rarely resolves without some sort of treatment. Fortunately, proper treatment helps resolve unusual lesions in most cases.
Plantar fibromatosis Complications
The condition does not always give rise to serious complications. For many patients, the presence of these lesions does not give rise to any problem. The bumps may remain same in size for a long time or may grow rapidly within a short duration. These are not cancerous growths and hence, do not spread to other areas of the body. As aforesaid however, patients with these nodules may experience painful symptoms at times.
Plantar fibromatosis Prevention
The cause of their development being unknown, Plantar fibromatosis nodules are difficult to prevent. However, seeking medical attention in the early stages can prevent further worsening of the condition. A few lifestyle modifications may help you avoid this problem. These include:
- Stretching exercises, especially for your plantar fascia (see Plantar Fasciitis Exercises)
- Drinking lots of fluids every day
- Following a healthy diet
- Wearing shoes that stabilize as well as support and protect your feet
- Maintaining a healthy weight
- Warming up before workouts followed by cooling down sessions afterward
- Gradually beginning new exercise routines
- Resting your feet as often as you can
You should also examine your feet from time to time to notice any changes that might not be apparent to the eyes.
Plantar fibromatosis Pictures
Check out the pictures of Plantar fibromatosis to know more about the condition.
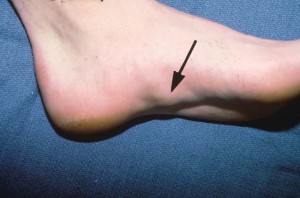
Picture 2 – Plantar fibromatosis Image
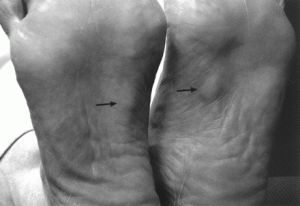
Picture 3 – Plantar fibromatosis Photo
If you find any hard lumps arising on your feet, it is best to call up your healthcare provider and make an appointment. Even if Plantar fibromatosis is not a discomforting syndrome, it may be an altogether different condition that you are suffering from. Early diagnosis and cure will help you make a quicker recovery and avoid any complicated condition.
References:
http://www.footanklehealth.com/ligaments/plantar-fibromatosis.html
http://emedicine.medscape.com/article/1061903-overview
http://www.bunionbusters.com/footcare/plantar_fibromatosis.asp
http://www.podiatrytoday.com/article/7488
