What is T-cell Lymphoma?
Page Contents
- 1 What is T-cell Lymphoma?
- 2 T-cell Lymphoma Incidence
- 3 T-cell Lymphoma Classification
- 4 T-cell Lymphoma Symptoms
- 5 T-cell Lymphoma Causes
- 6 T-cell Lymphoma Risk Factors
- 7 T-cell Lymphoma Diagnosis
- 8 T-cell Lymphoma Differential Diagnosis
- 9 T-cell Lymphoma Treatment
- 10 T-cell Lymphoma Prognosis
- 11 T-cell Lymphoma Survival Rate
- 12 T-cell Lymphoma Complications
- 13 T-cell Lymphoma Prevention
- 14 T-cell Lymphoma in Dogs
- 15 T-cell Lymphoma Pictures
T cell Lymphoma (TCL) is one of the four kinds of lymphoma that affect T-cells, the small lymphocytes that develop in the thymus. These can be related with Human T-cell leukemia virus-1 or Epstein Barr virus.
T-cell Lymphoma Incidence
The condition accounts for 8% of all cases of cancer involving same classes of blood cells. 2% of these cases are cutaneous T cell lymphomas and 2% are precursor T lymphoblastic.
T-cell Lymphoma Classification
The condition can be differentiated into a number of subtypes on the basis of their size, shape and other characteristics of the tumor cells. The classification of these tumors is complicated in nature as the majority of the tumors are different from other neoplasms.
TCL can generally be classified into the following categories:
Peripheral T cell Lymphoma
It is a very rare type of T cell Lymphoma that arises in mature T-cells. The condition is more common in grown-ups than in children. This is an aggressive, high-grade form of cancer.
Cutaneous T cell Lymphoma (CTCL)
It is a rare, low-grade form of Non-Hodgkin’s Lymphoma. This type of cancer has a slow progression and primarily affects the white blood cells known as T-cells in the skin.
Angioimmunoblastic T cell lymphoma (AILT)
Also referred to as Immunoblastic lymphadenopathy, it is a type of aggressive cancer that develops in the T-cells. It accounts for 1% of all cases of Non-Hodgkin’s Lymphomas (NHL) and is mostly found to affect the elderly population.
Hepatosplenic lymphoma (HSTCL)
It affects the T lymphocytes in the lymphatic system and is more specifically referred to as Hepatosplenic T cell lymphoma. It is not necessarily common for sufferers to have enlarged or inflamed lymph nodes, unlike many other types of Lymphomas.
Adult T cell Lymphoma (ATLL or ATL)
It is also referred to as adult T cell leukemia or HTLV-1 and is regarded as a Peripheral T cell lymphoma (PTCL). The condition is very rare in the U.S although it is reported to be more common in Japan and other regions of Asia.
This form of TCL is aggressive in nature and is further categorized into the following four subtypes:
- Acute ATL
- Lymphocytic ATL
- Chronic ATL
- Smouldering ATL
The first two subtypes are quite aggressive in nature and the last two are slow-growing. The Human Lymphotropic Virus-1 (HTVL-1) is responsible for this disorder.
The HTVL-1 virus is present in certain ethnic populations such as Caribbean, South America and Japan. However, only 2-5% of all infected individuals develop the disorder.
T-cell Lymphoma Symptoms
The signs and symptoms of this condition can vary on the basis of the location and stage of malignancy in the body. It can often be difficult to distinguish these symptoms from those of common ailments like flu or cold.
Some of the common signs of this disorder involve:
- Fever
- Headaches
- Unexplained weight loss
- Skin rash or itchy skin (Pruritus)
- Coughing or shortness of breath
- Difficulty moving parts of the body
- Night sweats that often soak the sheets
- Persistent fatigue, lethargy, feeling of tiredness
- Pain in the chest, abdomen or bones for no apparent cause
- Inflammation in the lymph nodes in the neck, underarms, groin, or abdomen
Due to the similarity of the symptoms with those of common disorders, it is essential for patients to get in touch with expert medical professionals who can carry out an accurate diagnosis.
T-cell Lymphoma Causes
It is not known what exactly results in the development of the majority of cases of TCL. However, it is possible that genetic alterations occurring at the time of antigen processing and presentation leads to an aggressively dividing cell population that may cause TCL.
T-cell Lymphoma Risk Factors
There are no known risk factors for this condition as TCL is found to arise mainly as a result of genetic changes. However, Adult TCL is found to arise more in people of the Asian regions. Due to this reason, being of Asian origin is supposed to increase the susceptibility of a person to Adult TCL.
T-cell Lymphoma Diagnosis
Lymphomas can develop from the lymph nodes that are located all over the body and are named according to the tissue where they originate. Due to this reason, a T cell lymphoma can be definitely diagnosed by an evaluation of cell types that are present in biopsy samples of tissue. This diagnostic process is contrary to another form of lymphoma, like a B-cell lymphoma.
The detection of TCL is usually based on the type of the condition that one suffers from:
Diagnosis of Peripheral TCL
A biopsy can be used for detecting PTCL in humans. Physicians can also look for physical signs associated with the development of the condition.
Diagnosis of Cutaneous TCL
It is diagnosed with the aid of biopsy which involves removal of a small part of the affected tissue for laboratory analysis. In the majority of cases of CTCL, the process is comparatively simple and can be performed with local anesthetics.
Diagnosis of Angioimmunoblastic TCL
This type of TCL can be detected with the help of a lymph node biopsy as well as other follow-up exams such as PET scans, x-rays, bone marrow biopsies and CT scans for staging of the disorder. Concrete information about staging is not available due to the rarity of the condition.
Diagnosis of Adult TCL
Biopsies are generally useful for the detection of this form of TCL.
Diagnosis of Hepatosplenic Lymphoma (HSTCL)
A bone marrow biopsy of the condition is likely to yield positive outcomes, as the involvement of bone marrow is common. Meanwhile, blood tests may reveal low blood counts or certain evidence of Cytopenia.
T-cell Lymphoma Differential Diagnosis
The differential diagnosis of TCL involves distinguishing the signs of the condition from those of similar disorders, such as:
- Allergic Contact Dermatitis
- Autoimmune lymphoproliferative syndrome (ALPS)
- Angiofollicular lymphoid hyperplasia (Castleman disease)
- Granulomatous disease
- Irritant Contact Dermatitis
- Lichen Planus
- Parapsoriasis
- Pediatric Atopic Dermatitis
- Pemphigus Foliaceus
- Plaque Psoriasis
- Pustular Psoriasis
- Tinea Corporis
- Paracortical (T zone) lymphoid hyperplasaia
- Kikuchi-Fujimoto disease, proliferative phase
- Paracortical (T zone) lymphoid hyperplasia
- Sézary syndrome (SS)
- T large granular lymphocytic leukemia
- T-cell prolymphocytic leukaemia (T-PLL)
T-cell Lymphoma Treatment
The treatment of TCL depends on the type of the disorder that a person suffers from.
Peripheral T cell Lymphoma Treatment
The treatment options for PTCL include steroids, chemotherapy, bone marrow transplant and radiotherapy. However, there is no gold-standard cure for recurring PTCL.
Cutaneous T cell Lymphoma Treatment
There are numerous treatment options for the disorder. The choice of treatment generally depends on the stage of the condition. The curative options that are usually opted for include:
- Photopheresis
- UVB Therapy
- PUVA treatment
- Topical treatment options
- Radiation
- Chemotherapy
- Bexarotene capsules
Angioimmunoblastic T cell lymphoma Treatment
The treatment for the disease generally begins with steroids that can help cure rashes and inflammation. The CHOP regimen of chemotherapy is generally administered after steroid treatment. Bone marrow transplants are generally tried in cases of recurrence of Adult TCL.
Adult T cell Lymphoma Treatment
An allogenic transplant may offer some amount of hope to approximately 40% of sufferers. IFN-alpha therapy or Zidovudine has been a little effectual in patients likely to show poor outcome. However, the treatment for this form of the disease has yet to be proven on a broader scale.
Hepatosplenic lymphoma Treatment
Combination chemotherapy tends to be the preferred curative option for people detected with this condition. In this process, one of the drugs to be administered is most likely to belong to the anthracycline class like Doxorubicin. However, medical treatment is not considered to be widely successful and recurrences are highly common, as is the case with many other forms of TCL.
HSTCL is a refractory and aggressive disorder. Due to this reason, it is difficult to treat. The median period of survival for patients from the time of diagnosis is said to be approximately 3 years.
T-cell Lymphoma Prognosis
The outcome of the condition depends on a variety of factors, such as the age of patients and the stage of the disorder. Those under the age of 60 and having a good performance status, stage 1 or 2 cancer and limited or non-existent lymph node involvement have a better prognosis. Those over 60 years of age, suffering from stage 3 or 4 cancer, poor PS, high LH levels and involvement of multiple lymph nodes show a poor outcome.
T-cell Lymphoma Survival Rate
Around 75% people in the lowest risk-group and only 30% of individuals in the highest risk-group have a 5 year survival rate.
T-cell Lymphoma Complications
The complications commonly associated with this condition include:
- Anemia or other blood abnormalities
- Enlargement of liver or spleen
- Malignancy
Death may also occur in older patients and in case of involvement of more than one lymph node. The survival rate is low in such people. Prompt treatment can ensure somewhat lower risk of life-threatening complications although that is often not true in case of aged patients.
T-cell Lymphoma Prevention
There is no known way to prevent this disease. However, its rapid progression and associated complications can be prevented by consulting a qualified medical professional on an earlier basis and undergoing diagnosis and treatment as early as possible.
T-cell Lymphoma in Dogs
TCL, along with B-cell Lymphoma, is one of the two types of lymphoma cancers that may affect dogs. TCL in dogs is referred to as Canine lymphosarcoma and generally arises in the bone marrow or the lymphatic system. Eventually, it spreads to the other regions of the body if left untreated. Suffering dogs may experience symptoms like inflamed lymph node, weight loss, fever, vomiting and weakness. Microscopic analysis of biopsy sample is usually the definitive diagnostic procedure for TCL in dogs. Intravenous chemotherapy is the most effective curative option for Canine lymphosarcoma.
T-cell Lymphoma Pictures
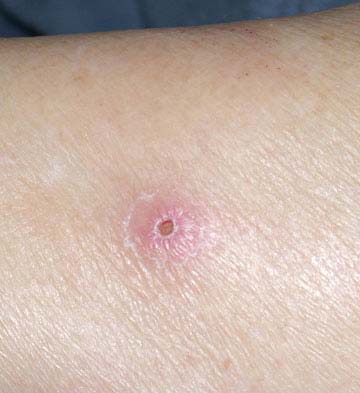
The following images will help you get an idea about the physical appearance of those suffering from TCL.
Picture 1 – T-cell Lymphoma
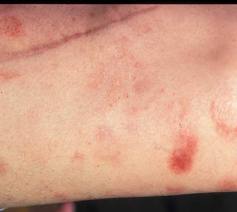
Picture 2 – T-cell Lymphoma Image
If you suspect yourself or a family member to be suffering from any form of TCL, do not delay treatment. Get in touch with a doctor as soon as possible and get tested. Faster detection and treatment has been found to reduce the risk of progression and improve the outcome for sufferers.
References:
http://www.cancercenter.com/non-hodgkin-lymphoma/t-cell-lymphoma.cfm
http://www.lymphomainfo.net/nhl/t-cell.html
http://en.wikipedia.org/wiki/T-cell_lymphoma
http://www.wisegeek.com/what-is-t-cell-lymphoma.htm