Wolf-Hirschhorn Syndrome is a dreadful condition associated with frequent stillbirths and perinatal deaths. Find out all about the disease, including its causes, symptoms, diagnosis and treatment.
Wolf–Hirschhorn Syndrome Definition
Page Contents
- 1 Wolf–Hirschhorn Syndrome Definition
- 2 Wolf–Hirschhorn Syndrome Synonyms
- 3 Wolf–Hirschhorn Syndrome Incidence
- 4 Wolf–Hirschhorn Syndrome Symptoms
- 5 Wolf–Hirschhorn Syndrome Causes
- 6 Wolf–Hirschhorn Syndrome Diagnosis
- 7 Wolf–Hirschhorn Syndrome Differential Diagnosis
- 8 Wolf–Hirschhorn Syndrome Treatment
- 9 Wolf–Hirschhorn Syndrome Prognosis
It is a chromosomal disorder that causes severe malformations in most parts of the body.
Wolf–Hirschhorn Syndrome Synonyms
The condition is also known by other names like:
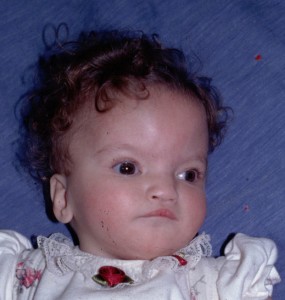
Picture 1 – Wolf-Hirschhorn Syndrome
- Chromosome deletion Dillan 4p syndrome
- Pitt-Rogers-Danks syndrome
- Pitt syndrome
The condition is generally abbreviated as WHS.
Wolf–Hirschhorn Syndrome Incidence
The prevalence of this rare syndrome is estimated to be approximately 1 in 50,000 births.
Wolf–Hirschhorn Syndrome Symptoms
During pregnancy, the affected fetus may show decreased movements and growth retardation. There is also a progressive degeneration of placenta, which impairs nutrient uptake, waste elimination, and gas exchange via the blood supply of mothers. The clinical features that are normally visible after the birth of the infants include:
- Scalp defect
- Broad-beaked nose
- Wide-spaced eyes
- Crossed eyes
- Drooping eyelids
- Cleft lip/palate
- Small chin
- Downturned mouth
- Undersized jaw
- Short vertical groove in the median portion of the upper lip
- Small and/or asymmetrical head
- Low-set ears with a small dimple or skin tag right in the front
- Hearing loss
- Congenital cardiac abnormalities
- Difficulty eating and swallowing
- Urinary opening on the underside of the penis
- Undescended testicles
- Seizures
- Growth deficiency
- Mental retardation
- Difficulty with speech
- Severe to profound developmental problems
- Hydrocephalus, an abnormal accumulation of cerebrospinal fluid in the brain
- Complete or partial absence of corpus callosum
- Lack of muscle coordination
- Abnormal gait
- Scoliosis
- Shortening of muscles of the hands, wrists, and feet
- Low muscle tone
- Delayed development of secondary sexual characteristics
- Congenital malformation in the lens, iris, or retina of the eye
- Underdevelopment/incomplete development of the kidneys and genital tract
- Abnormal opening in the diaphragm
- Immunodeficiency
Wolf–Hirschhorn Syndrome Causes
Nearly 90% of the cases of WHS occur due to a partial deletion of the short (p) arm of the chromosome 4, typically in the region of WHSC1 and WHSC2. This type of chromosomal abnormality is called pure de novo deletion in which a new mutation takes place without any inheritance. In the remaining 10% of cases, one of the parents has a balanced chromosome rearrangement involving the chromosome 4p (short arm of chromosome 4), which is derived by the child. In genetics, this 4p- anomaly is called balanced chromosome translocation in which an even exchange of chromosome material with no missing or extra genetic information, takes place. Parents who are carriers of a balanced translocation have an increased risk of having a child with unbalanced chromosome arrangement. The maternal transmission of the defective chromosome is two times greater than the paternal heritability. In 80% of de novo cases, affected individuals paternally acquire the anomalous chromosome. The amount of genetic material deleted from the chromosome determines the severity of the disorder and its phenotype, which are the observable physical characteristics of an individual.
Wolf–Hirschhorn Syndrome Diagnosis
WHS can be diagnosed at the prenatal stage with the help of the following tests:
Ultrasound scan
The abnormalities in the fetus, including the intrauterine growth deficiency, are sonographically detectable. The ultrasound findings may provide some information to the physicians regarding WHS.
Fetal Karyotyping
This is one type of chromosome analysis mandatorily conducted after a fetal ultrasound. The procedure requires a standard arrangement of the whole set of chromosomes that can be obtained by utilizing the following techniques:
Amniocentesis
The fluid present inside the amniotic sac in the uterine cavity is a potential medium for evaluating the karyotype of the fetus. Here, the fluid is removed by placing a long needle through the abdominal wall of the mother into the amniotic sac. The needle is guided into the sac using ultrasound imaging performed either prior to or during the procedure. Once the needle enters the sac, a syringe is used to withdraw the amniotic fluid. The collected sample is now sent for genetic evaluation. The deletion of the 4p- chromosome can be determined from the test.
Chorionic villus sampling
This is typically conducted between eighth and tenth weeks of pregnancy. Chorionic villi are the tiny finger-like projections on the edge of the placenta. A small sample of the placental tissues can be collected through the vagina or abdomen. In the former method, a thin, plastic tube along with a speculum is inserted up the vagina and into the cervix. The sampling of the chorionic villi is done on reaching the placenta. To collect the villi via abdomen, a long needle is directly infused into the placenta. The cells are then cultured and karyotypically analyzed for chromosomal defects.
Umbilical blood sampling
Blood can be withdrawn from the fetal umbilical cord by inserting a needle through the abdominal and uterine wall of the mother. Examination of the fetal blood is one of the most crucial means of rapid chromosome analysis.
Individuals born with WHS can be diagnosed on the basis of the distinctive craniofacial characteristics. The maldevelopment of the internal structures can be assessed with tests like:
Blood test
Patients with a compromised immune system show a diminished level of immunoglobins, a class of antibodies produced by the B cells, in their blood. Such patients also have a low count of T cells, a type of white blood cells called lymphocytes.
Electroencephalography (EEG)
Epileptic seizures are marked by abnormally high electrical activity of the brain. Electrodes or sensors are placed on the patient’s scalp in order to record the electrical signals of the brain. The EEG pattern obtained after the procedure is evaluated by a neurologist for any abnormality.
Echocardiography
The possible congenital conditions of the heart such as atrial or ventricular septal defect can be identified using this technique. High-frequency waves provide detailed images of the internal structures of the organ. The pumping ability of the heart is also studied to determine its current status.
Imaging techniques
A series of MRI and CT scans can fairly demonstrate the underlying problems of the brain.
Wolf–Hirschhorn Syndrome Differential Diagnosis
The clinical findings of WHS can also be consistent with other genetic syndromes that must be distinguished from the disorder. Some of these include:
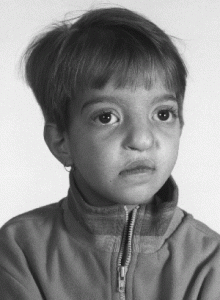
Picture 2 – Wolf-Hirschhorn Syndrome Image
- Cri-du-chat Syndrome
- Patau Syndrome
- Smith-Lemli-Opitz Syndrome
- Trisomy 18
Wolf–Hirschhorn Syndrome Treatment
Presently, there is no single treatment available for this complex disorder. However, management of the various symptoms can lessen the severity of WHS. Administration of valproic acid and benzodiazepines can control seizures. Multidisciplinary team approach is imperative for managing the physical and behavioral conditions. Occupational and physical therapy aid in maintaining muscle strength and movement of the joints. Speech and communication specialists help affected children in improving their cognitive aspects of communication as well as the language. Physicians must accomplish standard procedures for treating the associated ocular disorders, congenital cardiac defects and skeletal abnormalities. Patients who have difficulty in swallowing and eating are provided with a gastrostomy feeding tube, a medical device inserted through a small incision in the abdomen into the stomach for long-term nutrition.
Wolf–Hirschhorn Syndrome Prognosis
In very few cases, affected patients survive beyond infancy. However, sufferers are prone to a number of developmental and growth disorders. The mortality rate is high in the first two years of life due to the existence of severe conditions such as heart defects and hydrocephalus.
People who known themselves to be carriers of Wolf–Hirschhorn syndrome must undergo genetic testing and counseling prior to starting a family as this would prevent the disorder from getting transmitted to the child. Prenatal screening is advisable to families that have one parent as a carrier of the syndrome.
References:
http://en.wikipedia.org/wiki/Wolf%E2%80%93Hirschhorn_syndrome
http://emedicine.medscape.com/article/950480-overview
http://ghr.nlm.nih.gov/condition/wolf-hirschhorn-syndrome
http://wolfhirschhorn.org/about-wolf-hirschhorn-syndrome/