Vasculitis is a rare cardiovascular disease that gives rise to a number of problems, some of them even life-threatening ones, in individuals suffering from it. Read and know all about the disorder, including its possible causes, symptoms, diagnosis and treatment options.
Vasculitis Definition
Page Contents
It refers to a swelling of the blood vessels, occurring due to an attack on the vessels by the immune system of the body. However, the disease often arises as a result of unknown causes.
The condition is also known as Angiitis or Arteritis.
Vasculitis ICD9 Code
The ICD9 Code for this disorder is 447.6.
Vasculitis Incidence
This is a rare disease. Approximately 3,000 individuals in the U.K suffer from any of its forms on an annual basis.
Vasculitis Symptoms
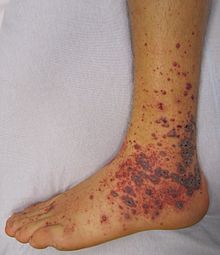
The condition may give rise to a variety of symptoms, as any organ might be affected. If the skin is affected, patients may develop rashes. In case nerves suffer from a lack of blood supply, affected individuals may suffer from an abnormal sensation which may be followed by muscular weakness or loss of sensation.
Picture 1 – Vasculitis
If Vasculitis affects the brain, a stroke may ensue. If it impacts the heart, individuals affected by the disorder may suffer a heart attack. Swelling in the kidney may cause abnormalities that can result in progressive kidney failure. Such abnormalities can be noticed in urine tests.
In some cases, the symptoms might be general in nature and include:
- Fever
- Loss of weight
- Loss of appetite
- Loss of energy
Patients should contact a physician in case of such abnormal symptoms.
Vasculitis Causes
The condition arises when the immune system mistakes the blood vessel cells as foreign objects such as invading microbes, like virus or bacteria. Hence, it acts against the vessels as a natural response. It is not known why this occurs. Many of the types of the disorder occur due to unknown factors and are referred to as Primary Vasculitis. The cases of the disease that have some underlying factor are referred to as Secondary Vasculitis. The underlying causes for the secondary types have been identified. These include:
Certain types of cancers
Cancerous conditions that affect the blood vessels, including Lymphoma and Leukemia, can result in Vasculitis.
Infection
The disorder may also arise in response to an infection. The majority of cases of cryoglobulinemia arise as a result of Hepatitis C viral infection. Certain cases of Polyarteritis nodosa occur in response to Hepatitis C virus infection.
Allergic reaction
Some individuals are found to develop this disorder due to an allergic reaction to some medication.
Some immune system disorders
The condition may also occur as a result of some disorders of the immune system, such as Lupus, Rheumatoid Arthritis or Scleroderma.
The blood vessels affected by this disorder may suffer an inflammation, which can lead to a thickening of the layers of the walls of the blood vessels. This results in a narrowing of the blood vessels and lowers the amount of blood, and consequently the oxygen and important nutrients, reaching the body tissues.
In certain patients, an affected blood vessel may develop a blood clot which can lead to an obstruction in the supply of blood. In some cases, rather than being narrowed, a blood vessel may weaken and develop a bulge (or aneurysm) which is a potentially fatal disorder.
Vasculitis Diagnosis
The diagnosis for this disease usually begins with doctors asking patients about their symptoms, followed by a complete physical examination and analyzing their past medical history. Further diagnostic tests for the disorder include:
Urine tests
Testing urine samples of sufferers may help physicians detect abnormalities, such as higher amounts of protein and red blood cells, which frequently indicate a medical problem. The outcome tends to be poorer if the disease results in kidney problems.
Blood tests
When used to detect Vasculitis, blood tests involve special exams like C-reactive protein tests and Erythrocyte Sedimentation Rate (ESR) to look for signs of swelling. A complete blood count (CBC) can help determine whether or not a patient has enough blood cells. Antineutrophil cytoplasmic antibodies test, an exam for detecting certain antibodies, indicate whether or not the immune system of the sufferer is fighting healthy cells.
Imaging tests
Noninvasive imaging procedures help physicians to find out whether or not larger arteries, like the aorta and its branches have been affected. Such tests include ultrasound, x-ray, Magnetic Resonance Imaging (MRI) and Computerized Tomography (CT) scans.
Biopsy
This is a surgical process involving removal of a small sample of an organ or blood vessel that has been affected. The affected parts may include the nerve, lung, skin and kidneys. Biopsy helps a physician to examine tissues for signs of Vasculitis.
Angiogram
In this test, a flexible catheter (that appears as a thin straw) is introduced into vein or large artery. Then, a contrast medium or special dye is injected into the catheter. X-ray images are obtained as the dye fills these veins or arteries. The outlines of the blood vessels can be viewed on the resulting images of X-rays.
Vasculitis Differential Diagnosis
The differential diagnosis for the disease includes ensuring the absence of a variety of conditions that may mimic the symptoms of cutaneous Vasculitis. These include:
- Trauma
- Insect bites
- Pigmented lesions
- Pityriasis lichenoides
- Purpura eg due to low platelet count
- Disseminated intravascular coagulopathy
Before arriving at a conclusion, physicians should consider the above conditions and ensure their absence. Not doing this can lead to a misdiagnosis and erroneous treatment on the part of a doctor, jeopardizing the health of sufferers.
Vasculitis Treatment
The treatment for this disorder is specific in nature and depends on the following factors:
- The type of Vasculitis that an individual is found to suffer from
- The severity of the condition
- The general health of sufferers
Certain forms of this disorder, such as Henoch-Schonlein purpura, are found to be self-limiting and resolve on their own. Others, however, need medications to improve.
The medicines used to cure Vasculitis involve:
Steroids
These are useful for addressing the problem of inflammation associated with this disease. Many forms of Vasculitis need to be cured with doses of corticosteroid drugs like Methylprednisolone (Medrol) or Prednisone for control of swelling.
The side effects of steroid treatment can be acute in nature, particularly in cases where the medications are taken for a prolonged duration. The problems may include:
- Diabetes
- Weight gain
- Thinning of bones (Osteoporosis)
Due to this reason, physicians tend to administer patients with the lowest possible doses of steroids to manage the disorder.
Immune system medicines
Acute cases of Vasculitis or those that show poor response to corticosteroids may need to be treated with Cytotoxic medicines that destroy immune cells which lead to swelling. Cytotoxic drugs include cyclophosphamide (Cytoxan) and azathioprine (Azasan, Imuran).
Rituximab (Rituxan) is another medicine that helps slacken the response of the immune system. The drug, along with corticosteroids, has been approved for curing Microscopic polyangiitis and Granulomatosis with Polyangiitis (Wegener’s). Medical researchers have also got some amount of success in using drugs that change the response of the immune system to cure some forms of vasculitis. Medicines that have been used and are still in the testing phase include adalimumab (Humira), anakinra (Kineret), infliximab (Remicade) and mycophenolate (Cellcept).
Patients may seek medical help from the following healthcare providers who specialize in treating Vasculitis:
- Skin doctors (dermatologists)
- Brain and nervous system doctors (neurologists)
- Muscle and Joint doctors (rheumatologists)
- Kidney doctors (nephrologists)
- Heart doctors (cardiologists)
- Eye doctors (ophthalmologists)
- Doctors for infectious diseases
- Lung doctors (pulmonologists)
Before visiting any of the above mentioned medical professionals, sufferers should make a list of:
- All the symptoms that they have been experiencing
- All the medications that they have been using of late, including one or more supplements
- Any recent changes in their life, such as a major stressful event
As appointments are brief, it is better to be well-prepared beforehand to make the most of time and also to avoid missing out any key information.
Vasculitis Management and Support
The management and supportive measures associated to this disease include:
Choosing a healthy diet
Following a healthy diet can help patients prevent possible side effects of medications, such as high blood pressure, diabetes and thinning of bones. Follow a diet that is rich in whole grains, lean meats, fishes, low-fat dairy products and fresh fruits and vegetables. If you are undergoing a corticosteroid therapy, ask your physician to suggest you a good calcium or Vitamin D supplement.
Regular exercise
Performing aerobic exercises on a regular basis, and even walking, can help prevent side effects of corticosteroids like diabetes, high blood pressure and bone loss. It can also be beneficial for vital organs of the body, such as the heart and the lungs. Moreover, many patients find that performing workouts on a regular basis improves their mood and also improves their overall sense of well-being.
Patients who are not used to workouts should begin gradually and then build up over a period of several weeks or months. Your physician can help you plan a workout regimen that is ideal for you.
Vasculitis Complications
The complications for Vasculitis depend on the type of the condition that one suffers from. Generally, the complications include:
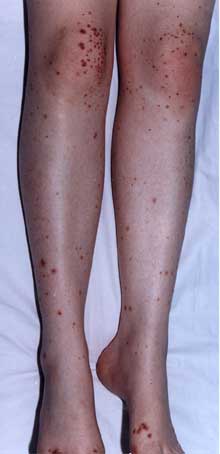
Picture 2 – Vasculitis Image
Repeated episodes of Vasculitis
Vasculitis may recur even in cases where the treatment for the disorder is initially successful. In such cases, additional curative measures may be needed. In other cases, the disease may never go away completely and need ongoing treatment.
Organ damage
Certain forms of Vasculitis can be acute in nature and cause damage to major organs.
Some of the common complications involve the following problems:
- Arterial or venous thrombosis
- Central nervous system infarction
- Digital gangrene
- Pulmonary haemorrhage
- Renal insufficiency
- Subglottic stenosis
Vasculitis Prognosis
The outcome of the disorder depends on the degree of end-organ involvement of patients. When the condition is detected and cured on an early basis, the outcome is generally good.
If you suspect yourself to be showing the symptoms of Vasculitis, seek treatment on an immediate basis. Early cure can help you recover faster from the condition while keeping it neglected can do just the opposite and even give rise to life-threatening consequences. Naturally, it is imperative that you consult your family physician and get yourself diagnosed.
References:
http://www.mayoclinic.com/health/vasculitis/DS00513
http://www.nlm.nih.gov/medlineplus/vasculitis.html
http://www.patient.co.uk/doctor/Vasculitis.htm
http://www.medicinenet.com/vasculitis/article.htm