Acrodermatitis enteropathica (AE) is a rare condition, typically arising in both breast-fed and bottle-fed infants. Get detailed information about this disease, including its symptoms, causes, diagnosis, and treatment.
Acrodermatitis enteropathica Definition
Page Contents
- 1 Acrodermatitis enteropathica Definition
- 2 Acrodermatitis enteropathica Symptoms
- 3 Acrodermatitis enteropathica Causes
- 4 Acrodermatitis enteropathica Diagnosis
- 5 Acrodermatitis enteropathica Differential Diagnosis
- 6 Acrodermatitis enteropathica Treatment
- 7 Acrodermatitis enteropathica Prognosis
- 8 Acrodermatitis enteropathica Complications
It is an inherited childhood disorder caused due to malabsorption of zinc.
The condition is also known by other names like:
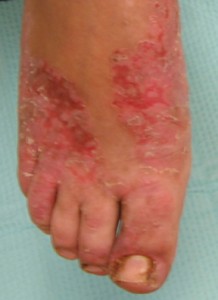
Picture 1 – Acrodermatitis enteropathica
- Congenital zinc deficiency
- Danbolt-Cross syndrome
- Brandt syndrome
Acrodermatitis enteropathica Symptoms
In the first few months of life, infants affected by AE stop drinking breast milk. They become irritable and often inconsolable. The other clinical features manifested in the later stages of the disorder include:
- Failure to thrive
- Inflammation of the skin on the cheeks, elbows, knees, hands, feet and scalp
- Dry scaly plaques on the skin, evolving into eroded, pustular or pus-filled lesions
- Balding of the scalp, eyebrows and lashes
- Delayed wound healing
- Swelling and redness of tissues surrounding the mouth and anus with formation of blistering, oozing, and crusting eruptions
- Red glossy tongue
- Mouth ulcers
- An inflammatory lesion at the corner of mouth
- Recurrent bacterial and fungal infections of the skin lesions
- Diarrhea or other gastrointestinal disturbances
- Infection along the edge of a fingernail or toenail
- Nail dystrophy
- Abnormal sensitivity to light
Acrodermatitis enteropathica Causes
AE arises due to an inborn error of metabolism, in which patients display autosomal recessive traits. Zinc is an essential trace nutrient required for proper function of several enzymes and has a crucial role in nucleic acid metabolism. Normal and prenatal development cannot take place without this mineral. In addition to this, it even impacts the immune system and the process of wound healing. Multiple systems in the body suffer when the level of zinc is too low. The genetic disorder has been ascribed to a mutation of the SLC39A4 gene on chromosome 8 q24.3. The SLC39A4 gene primarily encodes a transmembrane protein that forms a part of the zinc/iron-regulated transporter–like protein family required for uptake of zinc into the blood. The protein is typically expressed in the enterocytes lining the mucosa of duodenum and jejunum of the small intestine. Individuals who receive two copies of the mutated gene, one from each parent are likely to be affected with the condition. In the absence of the transmembrane protein, affected infants develop a reduced ability to absorb dietary zinc during weaning. Non-existence of a binding ligand required to transport zinc may cause additional problems in the absorption of the biologically significant element. Such a ligand has been identified in normal pancreatic secretions, as well as in human milk.
Genetic researchers have also observed that the condition begins to develop in full-term breastfed infants. Premature babies normally have high physiological demand for zinc. Lack of zinc in maternal serum, or a defect in the secretion of zinc from the mammary gland could be closely associated with the deficiency disorder. High concentration of phytate found in cereals and soy milk may also inhibit zinc absorption. Infants who have the habit of eating earthy substances such as sand or mud may have impaired zinc metabolism. The condition has also been reported in infants with undiagnosed food allergy and liver disorders.
Acrodermatitis enteropathica Diagnosis
There is usually a sharp demarcation between the affected area and normal skin. The appearance of various dermatologic features may sufficiently confirm the diagnosis of the disorder. However, signs of secondary infection may sometimes obscure the important clinical presentations due to which physicians perform additional tests and exams. Some of these are:
Blood test
Low serum/plasma zinc level, reflects impaired metabolism of the mineral. The important component can also be tested in red blood cells, white blood cells and platelets. However, the evaluation of cellular zinc level is technically more difficult, despite the fact that fluctuation of this trace element is greater in the serum. Low concentration of zinc in hair is verified only in rare cases. The hepatic function status can be determined by screening the blood for the presence of antibodies produced against the viral agents invading the liver. Certain liver enzymes are spilled into the blood stream when the liver is infected or injured. In such cases, therefore, a simple blood test is advisable.
Urine test
Reduced amount of zinc in a sample of urine imply low absorption of the mineral.
Skin biopsy
The most common reason for conducting a skin biopsy is to look for characteristic features like pustules, blisters and presence of flakes. The histopathological findings are necessary for the appropriate diagnosis of the condition.
Acrodermatitis enteropathica Differential Diagnosis
Acquired zinc deficiency shares common symptoms with the autosomal recessive disorder. The underlying causes are however, different for this childhood disorder. These include factors such as inadequate dietary zinc, glucagonoma and heavy metal exposure. It is necessary for the health professionals to rule out the possibility of the acquired condition. A variety of dermatological conditions also exhibit the same set of clinical and histologic manifestations of congenital zinc deficiency. Some of these include:
- Atopic Dermatitis
- Cutaneous Candidiasis
- Mucosal Candidiasis,
- Epidermolysis Bullosa
- Seborrheic Dermatitis
Acrodermatitis enteropathica Treatment
Like most genetic disorders, this congenital condition has no permanent cure. Although gene therapy has shown optimistic results in clinical trials, its use in the treatment of the metabolic disorder remains uncertain. Lifelong oral zinc supplementation in the range of greater than 1–2 mg/kg of bodyweight per day can reverse the symptoms of the condition. It is normally administered in the form of zinc gluconate or sulfate as pure zinc may lead to allergic reactions in infants. Positive clinical response is normally observed by physicians within 5-10 days. Significant increase in the plasma zinc levels considerably improves the health of the patients. It is mandatory to monitor the zinc levels every 3-6 months. If the condition exacerbates, the oral dose of zinc should be subsequently increased. The scaly patches on the skin can be removed with the help of warm compresses, followed by topical application of petrolatum or petroleum jelly. The skin ointment has shown to enhance the formation of new cells when used in adjunct with zinc replacement. A diet rich in zinc applies only to young children. The level of zinc in the body can be raised by the consumption of:
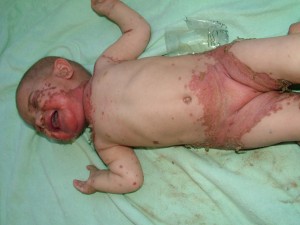
Picture 2 – Acrodermatitis enteropathica Image
- Oysters
- Beef
- Pork
- Chicken
- Turkey
- Red meat
- Baked beans
- Chickpeas
- Almonds
- Cashews
- Peanuts
Secondary dermatological infections can be readily treated with antibiotic therapy. Health care providers must be careful while treating patients with zinc supplementation as high doses result in side-effects such as dizziness and anemia. Treatment of the underlying hepatic disorders can reverse the condition and promote the levels of zinc.
Acrodermatitis enteropathica Prognosis
Patients who undergo replacement therapy receive substantial benefits and show consistent improvement. Outpatient follow-up care is equally essential for such individuals.
Acrodermatitis enteropathica Complications
Delayed treatment can increase the fatality of the disorder. The emphasis on constant supplementation of zinc is high, owing to the number of mortality cases in the past. An impaired liver along with serious zinc deficiency can be even more fatal to the patients.
Controlling zinc deficiency is the key for managing Acrodermatitis enteropathica. If your baby is showing signs of abdominal discomfort and skin irritation, it’s important to seek the assistance of a pediatrician as soon as possible. By closely working with an experienced healthcare provider, the health of a suffering infant can be made as normal as possible.
References:
http://en.wikipedia.org/wiki/Acrodermatitis_enteropathica
http://emedicine.medscape.com/article/912075-treatment#a1129
http://dermatology-s10.cdlib.org/133/case_reports/acrodermatitis/maverakis.html
http://bestpractice.bmj.com/best-practice/monograph/1195/diagnosis/step-by-step.html