Bronchiectasis Definition
Page Contents
- 1 Bronchiectasis Definition
- 2 Bronchiectasis ICD9 Code
- 3 Bronchiectasis Incidence
- 4 Bronchiectasis Symptoms
- 5 Bronchiectasis Causes
- 6 Bronchiectasis Risk Factors
- 7 Bronchiectasis Diagnosis
- 8 Bronchiectasis Differential Diagnosis
- 9 Bronchiectasis Treatment
- 10 Bronchiectasis Prognosis
- 11 Bronchiectasis Complications
- 12 Bronchiectasis Prevention
Bronchiectasis refers to an abnormal widening of one or more air passages causing them to become scarred and flabby.
The disorder is also referred to by other names, like:
- Acquired bronchiectasis
- Congenital bronchiectasis
The condition can arise at any age.
Bronchiectasis ICD9 Code
The ICD9 Codes for this disorder are 494 and 748.61.
Bronchiectasis Incidence
Global data about the exact incidence of this disease is not known. The condition is relatively uncommon in the U.S, with a prevalence of around 100,000 cases – based on data available from the 1980s.
Bronchiectasis Symptoms
The symptoms of this disease arise gradually. They may develop months or years after the event that gives rise to Bronchiectasis. The signs and symptoms may include the following:
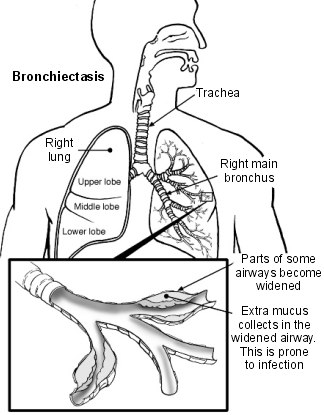
Picture 1 – Bronchiectasis
- Fatigue
- Breath odor
- Bluish skin color
- Coughing up blood
- Paleness
- Wheezing
- Weight loss
- Clubbing of fingers
- Cough that gets worse when lying on one side
- Shortness of breath that gets worse with exercise
- Chronic cough with large amounts of foul-smelling sputum
Over a period of time, sufferers may experience symptoms of a more severe nature. They may feel extremely tired and may cough up bloody mucus or even blood. Children affected by this disease may not be able to lose weight or develop at a normal pace.
Bronchiectasis Causes
The condition usually arises as a result of damage to the walls of the air passages. This damage can occur due to infectious conditions of the lung, such as:
- Fungal infections
- Tuberculosis
- Acute pneumonia
- Measles or whooping cough (rare disorders in the U.S as a result of vaccination)
The disease can also originate due to conditions that damage the air passages and elevate the risk of lung infections, including:
- Conditions that can cause the obstruction of airways, such as inhalation of small objects or development of a growth or benign tumor.
- Malformation of the lungs in the fetal stage (known as Congenital Bronchiectasis).
- Chronic pulmonary aspiration, Allergic bronchopulmonary aspergillosis, cystic fibrosis and immunodeficiency disorders that can increase the risk of lung infections.
Bronchiectasis Risk Factors
The risk factors for this condition include:
Being female
Females are supposed to be more susceptible to this condition. Two-thirds of all sufferers of this disorder are found to be women. However, the disease is more common in boys than in girls in children population.
Certain disorders
Some conditions that increase the risk of lung infections and damage the lungs can make sufferers susceptible to Bronchiectasis. Such diseases include:
- Immunodeficiency disorders like common variable immunodeficiency and rarely HIV and AIDS
- Cystic fibrosis, which is the cause of 50% of all cases of Bronchiectasis in the U.S
- Conditions that affect functioning of the cilia, such as Primary Ciliary Dyskinesia
- Allergic bronchopulmonary aspergillosis, which is an allergic response to a type of fungus known as Aspergillus. This response results in an inflammation of the air passages.
Bronchiectasis Diagnosis
Doctors may suspect the condition if patients suffer from a daily cough that is characterized by large amounts of sputum. To determine the presence of this disease, doctors may recommend tests in order to rule out other causes of the symptoms, determine the extent of damage to the airways and detect any underlying causes that need treatment.
The diagnostic tests for this disease include the following:
Chest x-ray
It is a painless exam that creates pictures of chest structures, such as the lungs or the heart. It can also reveal abnormal regions of the lung and irregular, thickened walls of the airways.
Chest CT scan
It is the most common diagnostic test for this disease and is painless for sufferers. This imaging exam produces accurate images of the airways as well as other structures in the chest. It can also determine the location and extent of lung damage and renders more detailed images than a standard x-ray of the chest.
Bronchoscopy
This is carried out if the condition fails to respond to standard treatment options. Physicians use this technique to view the inside of the air passages. In this test, a flexible tube fitted with a light at one end (bronchoscope) is inserted into the airways through the mouth or the nose.
Bronchoscope renders a video image of the airways. Before conducting the test, medications are administered to patients to induce numbness into their upper air passages to help them relax during the technique. The process can show a possible obstruction in the airways and also reveal any source of bleeding in the airways.
Other tests
Doctors may also recommend certain other exams, such as:
- Lung function tests
- Sputum culture
- Sweat tests
- Blood tests
- Serum immunoglobulin electrophoresis
- Genetic testing, including sweat test for cystic fibrosis
- PPD skin test, in order to detect a prior tuberculosis infection
- Aspergillosis precipitin test (to check for signs of the aspergillosis fungus)
Initially, however, doctors may listen to the lungs of patients with a stethoscope to hear abnormal lung sounds.
Bronchiectasis Differential Diagnosis
The differential diagnosis of this disease includes telling its symptoms apart from those of other conditions that produce similar symptoms. These include:
- Primary Ciliary Dyskinesia
- Cystic fibrosis
- Respiratory failure
Physicians should make sure that patients are not suffering from any of these conditions and actually exhibiting the signs of Bronchiectasis.
Bronchiectasis Treatment
The condition is often cured with the aid of hydration, medications and chest physical therapy (CPT).
Medicines
These include:
Antibiotics
This class of drugs is the main treatment option for recurring lung infections caused by Bronchiectasis. Oral antibiotics are often used to cure such infections. Physicians may prescribe intravenous (IV) antibiotics to cure infections that are hard to treat. Such drugs are administered through an IV line inserted into the arm.
For persisting cases, doctors may help arrange for a care provider at home to administer antibiotic medicines.
Bronchodilators
This helps relax the muscles around the air passages and open the airways, making breathing easier. The majority of Bronchodilators are medicines to be inhaled. In this technique, patients have to use a nebulizer or an inhaler to breathe in a fine mist of medicine. Inhaled Bronchodilators work rapidly as the medication goes straightly to the lungs. Physicians may recommend sufferers to use a bronchodilator just prior to CPT.
Mucus-thinners or expectorants
These are used to help patients cough up mucus. Expectorants can help loosen the mucus present in the lungs. These are often used along with decongestants to provide patients with additional relief. Mucus thinners like Acetylcysteine help loosen the mucus and make it easier for sufferers to cough up.
Hydration
Drinking lots of fluids, particularly water, can help prevent mucus in the airways from becoming thick and sticky in nature. Proper hydration can help make mucus moist and slippery in form, making it easier for sufferers to cough up.
Chest Physical Therapy (CPT)
Also referred to as Percussion or Chest Clapping or Physiotherapy, this process includes using hands or a specialized device to pound the chest and back again and again. This technique can help loosen the mucus from the lungs so that sufferers can cough it up.
While CPT is being carried out, patients can sit or lie on their stomach with their head in a tilted down posture. Gravity and force can help drain the mucus from the lungs.
Bronchiectasis Prognosis
The outcome of this disorder is based on the particular underlying cause of the disorder. In the majority of affected individuals, the symptoms do not worsen. The condition takes a turn for the worse in certain cases and patients may suffer from respiratory problems. In a small number of sufferers, the disease gradually becomes worse as more and more air passages are affected. In rare cases, a life-threatening bleeding from a damaged air passage may also occur.
With proper and timely treatment, however, the majority of sufferers can lead normal lives without suffering from a major disability.
Bronchiectasis Complications
Acute cases of this disease may result in serious health disorders, like:
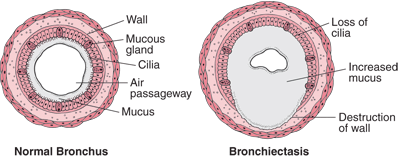
Picture 2 – Bronchiectasis Image
Atelectasis
In this condition, one or more regions of the lungs fail to inflate properly or even collapse. Due to this reason, sufferers may experience shortness of breath. The breathing rate and heart rate may increase, and there can also be blue discoloration of the lips and skin.
Respiratory Failure
In this condition, there is a deficiency of oxygen passing into the blood from the lungs. The disease can also develop if the lungs cannot properly remove carbon dioxide (CO2) from the bloodstream. The condition can result in problems like rapid breathing, shortness of breath and air hunger (sensation of lacking enough air for respiration). In acute cases, the symptoms may involve sleepiness, confusion and a bluish discoloration of the fingernails, lips and skin.
Heart failure
If Bronchiectasis is severe enough to affect all parts of the air passages, it may result in cardiac failure – a condition in which the heart is unable to pump enough blood to satisfy the needs of the body. This may be characterized by problems like fatigue, shortness of breath and inflammation of the abdomen, legs, feet, ankles and neck veins.
Other possible complications include:
- Coughing up blood
- Cor pulmonale
- Recurrent pneumonia
- Low oxygen levels (in severe cases)
Bronchiectasis Prevention
It is necessary to prevent lung damage, and lung infections that may arise as a consequence, in order to prevent Bronchiectasis. Childhood vaccines for whooping cough and measles can prevent infections associated to such disorders. These vaccines also decrease complications from these infections, like Bronchiectasis.
Proper medical treatment of lung infections in children may also help prevent lung damage (that can cause this disorder) and preserve lung function.
Avoiding smoke, gases, toxic fumes and other harmful materials can also help protect the lungs. Children as well as adults should be stopped from inhaling small materials that might enter and obstruct the small air passages. In case of accidental inhalation of such materials, medical attention should be sought on a prompt basis.
In case you or any of your family members is suffering from difficulties like respiratory shortness, chest pain or change in phlegm color, you should contact a professional medical care provider on an immediate basis. Prompt medical treatment can help achieve a faster recovery and avoid all possible complications.
References:
http://www.nhlbi.nih.gov/health/health-topics/topics/brn/treatment.html#
http://www.wisegeek.com/what-is-bronchiectasis.htm
http://en.wikipedia.org/wiki/Bronchiectasis
http://emedicine.medscape.com/article/296961-overview