Chancroid is a rare disorder that gives rise to painful, elevated ulcers over the skin surface. Read and find out all about the causes, symptoms, diagnosis and treatment of Chancroid disorder.
What is Chancroid?
Page Contents
- 1 What is Chancroid?
- 2 Location of Chancroid
- 3 Chancroid Symptoms
- 4 Chancroid in Women
- 5 Chancroid Causes
- 6 Chancroid Diagnosis
- 7 Chancroid Treatment
- 8 Chancroid Pictures
- 9 Chancroid and Haemophilus Ducreyi
- 10 Chancroid and STD
- 11 Chancroid Prognosis
- 12 Chancroid Prevention
- 13 Chancroid Statistics
- 14 Is Chancroid Curable?
This is a bacterial disorder that is transmitted by sexual contact. It is common in tropical nations but rare in other areas of the world.
Location of Chancroid
Each of these ulcers arises in particular spots. The most common spots where these ulcers arise are glans (tip of the penis), shaft of the penis, Coronal Sulcus or the groove posterior to the tip of the penis, scrotum and Urethral Meatus or aperture (opening) of the penis.
In women, these ulcers commonly arise on the Labia Majora or outer lips of the vagina. In some cases, an ulcer in one labium of vagina may give rise to a corresponding ulcer in another labium. These are known as “Kissing ulcers”.
Chancroid Symptoms
This infectious disorder is marked by bubo formation, painful ulcers and painful chronic enlargement of the lymph nodes in the groin (Inguinal Lymphadenopathy).
An individual usually develops a small lump in the groin within a day or even a week or two after getting Chancroid. This becomes an ulcer within a day after its origin. The ulcer is soft, painful and its diameter varies from 1/8 inch to 2 inches. It has clearly defined edges though some are also seen with ragged borders.
The base of these ulcers is covered with a grey or grayish-yellow substance. They bleed easily if scraped or injured.
Approximately half of all infected men suffer from only one ulcer. Women are seen to have 4 ulcers or more.
Chancroid in Women
These ulcers are frequently seen to be asymptomatic in women. These may arise within the body and can go unnoticed. Women may not become aware of these lesions due to absence of symptoms. A medical study isolated the Haemophilus ducreyi bacteria from the urogenital tract of women who are healthy. This indicated that women may be the carriers of the bacterium which suggests why there is a low incidence of the condition in women.
In women, these lesions can be found on regions like
- Clitoris
- Fourchette
- Labia Majora
- Labia Minora
In women, the condition involves direct extension of the anus. It appears on the anus as a cleft encircled by hypertrophic growths. These may be mistaken for hemorrhoids or warts.
A person may be regarded as infectious due to the presence of these lesions. The disease has not been reported in kids born to women who have active Chancroid at the time of childbirth.
Chancroid Causes
This disorder mainly results from an infection caused by a kind of bacteria that is known as Haemophilus ducreyi (abbreviated as H. Ducreyi). It is a gram-negative bacterium that is generally situated in the spaces outside cells.
As aforesaid, this disease is generally spread by sexual contact. The bacteria may invade the sexual organs during physical intimacy, particularly at points where there is a pre-existing trauma, such a small scratch or cut. If the person is sexually active and has an improper sexual hygiene, he or she can be at greater risk of transmitting this disease.
Chancroid Diagnosis
These ulcers are generally diagnosed by physical observation and checking for inflammation of lymph nodes. An experienced doctor can generally make a prompt identification of this disease simply by looking at the sores or inflamed lymph nodes in the groin.
Chancroid Treatment
This condition is generally treated with the aid of antibiotics such as
- Ceftriaxone
- Erythromycin
- Ciprofloxacin
- Azithromycin
Antibiotic medications are typically prescribed to destroy the bacteria. Large lymph node inflammation requires draining, either with local surgeries or needle operation. In case of inflammation of the inguinal lymph nodes, a doctor will generally make a perforation on the surface of the ulcer skin with a needle or by cutting out the top surface. These are important for removing the infected fluid if the lymph nodes are still under the surface of the skin.
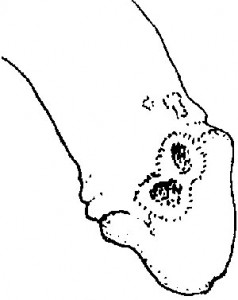
Chancroid Pictures
Here are some images of Chancroid that will provide you with an idea of how these ulcers look like. You may find these photos of Chancroid quite useful for reference.
Picture 1 – Chancroid
Source – magazine.ayurvediccure.com
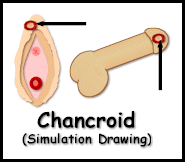
Picture 2 – Chancroid Image
Source – mjbovo.com
Chancroid and Haemophilus Ducreyi
As aforesaid, the Haemophilus Ducreyi is the causative factor of this disorder. This bacterium is the major cause of this condition in Southeast Asia and Africa. It is also becoming a cause of concern in the United States.
Chancroid and STD
Individuals having chancroid lesions should be diagnosed to detect the presence of any other sexually transmitted diseases (STD) like genital herpes infection, HIV infection and Syphilis. Patients with HIV (human immunodeficiency virus) must be particularly careful not to get this disorder as they have a weakened immunity that prevents complete healing of the sores. The transmission of this disorder can be avoided by using condoms during sexual intimacy. This infection is not generally life-threatening.
Chancroid Prognosis
These ulcers can get better without any external cure. However, some individuals may suffer from pain and drainage from their ulcers for several months. Antibiotic drugs usually clear up the ulcers rapidly with very little formation of scars.
Chancroid Prevention
This disorder can be prevented by avoiding all forms of sexual activity. However, a person may reduce the risk of contracting this condition by proper use of condoms. A person needs to keep wearing the condom from the beginning to the end of sexual activity.
Chancroid Statistics
In recent years, the practice of safer sexual habits has reduced the incidence of this disorder. In the United States alone, there are only about 143 individuals suffering from this condition on an annual basis.
Is Chancroid Curable?
This is a curable bacterial STD infection. Though extremely contagious, it can be cured with antibiotic medications. A follow-up examination should be carried out 3-7 days after beginning of treatment. On successful treatment, lesions usually show an improvement within this period.
If you suspect yourself to be suffering from symptoms of this disease, immediately get in touch with your healthcare provider. Early diagnosis and treatment will help you evade further complications and make a faster recovery.
References:
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001659/
http://www.wrongdiagnosis.com/c/chancroid/
http://www.space-age.com/std/chancroid02.html
http://www.idph.state.il.us/public/hb/hbchancroid.htm

Yes th information was beneficial to me thanks
Very beneficial to me