Creutzfeldt-jakob disease (CJD) is a rare, fatal disorder that affects one in every million individuals in the U.S alone and is found to afflict 250-300 new people in the nation. Read and know all about this disease, including its causes, symptoms, diagnosis and treatment options.
Creutzfeldt-jakob disease Definition
Page Contents
- 1 Creutzfeldt-jakob disease Definition
- 2 Creutzfeldt-jakob disease Synonyms
- 3 Creutzfeldt-jakob disease Incidence
- 4 Creutzfeldt-jakob disease Types
- 5 Creutzfeldt-jakob disease Symptoms
- 6 Creutzfeldt-jakob disease Causes
- 7 Creutzfeldt-jakob disease Transmission
- 8 Creutzfeldt-jakob disease Diagnosis
- 9 Creutzfeldt-jakob disease Treatment
- 10 Creutzfeldt-jakob disease Risk Factors
- 11 Creutzfeldt-jakob disease Complications
- 12 Creutzfeldt-jakob disease Prognosis
- 13 Creutzfeldt-jakob disease Prevention
It is a degenerative disorder of the nervous system that is characterized by a severe form of brain damage which leads to a rapid decline in movement and mental capabilities.
Creutzfeldt-jakob disease Synonyms
CJD is known by various other names, such as:
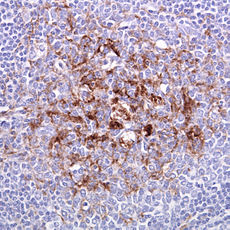
Picture 1 – Creutzfeldt-jakob disease
- Subacute Spongiform Encephalopathy
- Jakob’s Disease
- Jacob-Creutzfeldt disease
- vCJD
- Transmissible spongiform encephalopathy
Creutzfeldt-jakob disease Incidence
Fortunately, CJD is an extremely rare disorder and affects only about 250 to 300 individuals in the U.S. each year. The condition has been estimated to arise in only out of every 1 million people every year. It is most common in older adults. The condition usually appears first between 20 and 70 years of age. Its symptoms generally manifest in the late 50s. In rare cases, however, the condition can also be prominent in young adults and individuals over 80 years of age.
According to a 2004, it was assessed that the total number of cases would not surpass 2,000. The variant type of the disease, vCJD, is considered to be its least common form.
Creutzfeldt-jakob disease Types
The condition has been classified into two types:
Classic CJD
This has been further grouped into two separate forms:
Sporadic CJD
It accounts for 85% cases of the disease.
Familial CJD
This subtype is also known as Inherited CJD and is rare in form. It accounts for only 5-10% of all cases of the disease.
Variant CJD
It is a particular form of the disorder that is associated to Bovine Spongiform Encephalitis or BSE (the medical term for Mad Cow Disease) unlike Classic CJD. The condition is more common in younger people. It makes up for less than 1% of all cases of CJD. Less than 200 people around the world are found to suffer from this disorder. When Mad Cow Disease crosses species and afflicts humans, it is known as Variant Creutzfeldt-Jakob Disease. However, this only makes up a comparatively small number of cases.
There is also another form of CJD, known as Acquired Creutzfeldt-Jakob Disease.
Creutzfeldt-jakob disease Symptoms
The disease is characterized by abrupt development of neuromuscular and neurological symptoms that worsen rapidly. The primary ones of these symptoms include:
- Mental confusion
- Changes in gait (walking)
- A feeling of disorientation
- Dementia, occurring over a period of few weeks or months
- Blurred vision, in some cases
- Hallucinations
- Myoclonic jerks or seizures
- Lack of coordination (manifested by falling and stumbling)
- Muscle stiffness
- Muscle twitching
- Nervous, jumpy sensation
- Sleepiness
- Speech impairment
- Changes in personality
Although the signs of CJD are quite similar to those of other types of dementia (like Alzheimer’s disease), the two are rarely mistaken for one another. This is because the symptoms tend to worsen much faster in CJD. In both forms of CJD, the symptoms worsen quickly and lead to disability and death (unlike Dementia).
Creutzfeldt-jakob disease Causes
CJD as well as its variants are a part of a broad group of animal and human disorders known as “Transmissible spongiform encephalopathies” (TSEs). The name obviously refers to the spongy holes that develop in affected brain tissues and are visible under a microscope.
Abnormal versions of prions, a form of protein, are supposed to be the actual reason for the occurrence of CJD and other TSEs. These proteins are usually harmless. But they are found to become infectious, when deformed, and destroy normal biological activities.
The causes of CJD actually differ according to the type that one is found to suffer from. Know about the causative agents for various forms of the disease.
Causes of Sporadic CJD
This form seems to arise without any apparent reason. The condition usually manifests at around 65 years of age. Sporadic forms of CJD are believed to occur randomly due to a mutation (alteration) in the Prions (a type of protein) of the body.
Causes of Familial/Inherited CJD
It arises when an individual inherits an abnormal prion (a type of protein) from a parent. The defective gene leads to the formation of harmful prions.
Causes of Variant CJD
In humans, vCJD is believed to occur due to the same infection that gives rise to the disorder in cows.
Causes of Acquired CJD
It arises due to a contact with infectious tissues of the brain and the nervous system.
Creutzfeldt-jakob disease Transmission
The disorder, unlike conditions arising due to bacterial infection, is not transmitted from person to person through touching, sneezing, coughing or sexual contact. Due to this reason, there is low risk of transmission of this disease. The disease may develop due to:
Spontaneous occurrence
In the majority of patients with classic cases of CJD, there is no apparent cause for the development of the disease. CJD that arises without any specific reason is termed sporadic CJD or spontaneous CJD. Most CJD patients suffer from such spontaneous types of the disorder.
Genetic mutation
Around 5-10% of CJD sufferers in the US are found to have a family history of the condition or confirmed to be carriers of a mutated gene associated with the disorder. This type of the disease is known as Familial CJD.
Contamination
A small number of patients are found to develop the disorder on exposure to an infected human tissue during a skin or cornea transplant or a similar medical procedure. In cases where contaminated instruments are used for brain surgery, a few patients are seen to suffer from CJD. This also occurs due to the fact standard sterilization methods fail to destroy abnormal prions. Such cases of CJD, which are associated to medical processes, are known as Iatrogenic CJD.
Variant CJD is also believed to arise due to contamination. It is mainly associated to the consumption of beef that is infected with Mad Cow Disease.
Creutzfeldt-jakob disease Diagnosis
Physicians assess the personal and medical history of suspected CJD patients and also put them through a neurological exam and a few diagnostic tests to diagnose the disorder accurately. However, only an autopsy (brain tissue examination after death) and a brain biopsy help confirm the presence of the condition.
A neurological exam has the potential to disclose characteristic symptoms of the disease, such as coordination problems, spasms, muscle twitching, and abnormal reflexes. Ocular examination may also be assistive in diagnosis as CJD patients may also suffer from changes in visual-spatial perception and blind spots.
Some other tests, commonly used by physicians along with the aforementioned exams, are also assistive in the detection of CJD:
Electroencephalogram (EEG)
The test involves placing electrodes on the scalp and measuring the electrical activity of the brain. In individuals affected with CJD and vCJD, a characteristically abnormal pattern is exhibited in the results.
Magnetic resonance imaging (MRI)
This imaging procedure creates cross-sectional images of the head and body of patients by making use of a magnetic field and radio waves. MRI scans render high-resolution images of the white and gray matters of the brain. This makes the technique particularly assistive in diagnosing brain disorders.
Spinal fluid tests
The brain and spinal cord are surrounded and protected by the cerebral spinal fluid. Spinal tap, a popular lumbar puncture exam, is often used by doctors to analyze this fluid. Physicians use a needle to take out a small quantity of this fluid for analysis. CJD or vCJD can be said to be present if a specific protein, known as Prion, is detected in this fluid.
Tonsil biopsy
The method involves examining a tissue sample of the tonsil to detect the presence of vCJD. Although the test may help detect vCJD, it is seen as less reliable for the diagnosis of other forms of CJD.
Creutzfeldt-jakob disease Treatment
Unfortunately, there is no effective treatment for CJD or any of its variants as yet. CJD has a sudden and unstoppable onset once its symptoms begin to manifest. A variety of medications, including antiviral agents, antibiotics and steroids have been used with little or no success. Interleukins and other drugs may help retard the progression of the disease. Due to this reason, doctors aim at addressing the symptoms instead of the condition itself. The objective of symptomatic treatment is to provide as much comfort to sufferers as possible. The physical discomforts, such as pain, may be managed with analgesics. Antispasmodics can be effective in controlling muscular problems, like spasms. People suffering from this disease may require assistance in controlling dangerous or unacceptable behavior or actions arising due to CJD. A few drugs may also be needed to keep aggressive behavior in check.
Patients may require constant care in the early stage of the disease itself. Sufferers should be provided with a safe environment and all their requirements should be met in home. If that is not possible, they should be kept in a care facility. Family members should consider counseling to know about the changes required for home care.
Creutzfeldt-jakob disease Risk Factors
The risk factors of CJD cannot be identified as most of its cases occur due to unknown causes. However, a few factors have been supposed to make people more susceptible to different forms of CJD.
Age
Sporadic CJD affects older individuals, with the average age of onset being 60 years. Familial CJD develops slightly earlier. Young people are more susceptible to vCJD, the symptoms of which usually manifest in the late 20s.
Genetics
A genetic mutation is found to be responsible for the occurrence of Familial CJD. The condition is autosomal dominant in nature. This means an individual can develop the disease by inheriting a single copy of the mutated gene from either parent. A child has 50 percent chance of inheriting the disorder from a parent who is a carrier of the mutated gene.
Exposure to contaminated tissue
In patients of Variant and Iatrogenic CJD, genetic analysis suggests that inheritance of identical copies of certain prion variants may make a person susceptible to CJD on exposure to contaminated tissue. Individuals having dura mater grafts or received human growth hormone drawn from pituitary glands may be prone to Iatrogenic CJD.
It is difficult to assess the risk of contracting vCJD from the consumption of contaminated beef. Generally, the risk is found to be very low in countries where public health measures are effectively implemented.
Creutzfeldt-jakob disease Complications
The possible complications arising as a consequence of this disorder include:
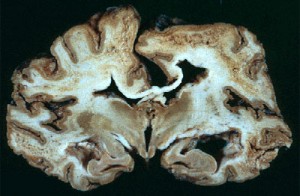
Picture 2 – Creutzfeldt-jakob disease Image
- Infection
- Reduced interactive ability
- Lowered functional ability
- Loss of capability for self-care
In worst cases, there may also be death of sufferers.
Creutzfeldt-jakob disease Prognosis
The condition generally exhibits a poor prognosis in its sufferers. A CJD patient is usually found to lose the ability to take care for himself/herself within 6 months or even less after the beginning of appearance of its symptoms. The condition becomes life-threatening within a short period, generally before 8 months have passed since the onset of symptoms. A few patients have been, however, found to survive for a maximum period of 1 or 2 years. Death usually occurs due to respiratory failure, cardiac failure or infection.
Creutzfeldt-jakob disease Prevention
The prevention of CJD is difficult. However, medical instruments can be used to remove the proteins (prions) from the body that act as causative agents of the disorder. People having a history of the disorder should not donate a tissue or cornea, as this might spread the condition. These days, there are strict guidelines in most countries for managing infected cows and prevent transmission of CJD from cattle to humans.
Although Creutzfeldt-jakob disease is not a medical emergency, it is sensible to seek early medical attention to help physicians control its symptoms more easily and prevent the disease from getting more complicated. If addressed and treated in time, the symptoms can be checked in time and there can be an improvement of the lifespan of patients.
References:
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001792/
http://www.mayoclinic.com/health/creutzfeldt-jakob-disease/DS00531
http://www.webmd.com/brain/creutzfeldt-jakob-disease
http://www.medicinenet.com/creutzfeldt-jakob_disease/article.htm