Esophageal Atresia (EA) is a rare congenial disorder found in newborns. Read on to know all about the causes, symptoms, diagnosis and treatment of this acute condition.
Esophageal Atresia Definition
Page Contents
- 1 Esophageal Atresia Definition
- 2 Esophageal Atresia ICD9 Code
- 3 Esophageal Atresia Incidence
- 4 Esophageal Atresia and Tracheoesophageal Fistula
- 5 Esophageal Atresia Classification
- 6 Congenital Esophageal Atresia
- 7 Esophageal Atresia Causes
- 8 Esophageal Atresia Symptoms
- 9 Esophageal Atresia Diagnosis
- 10 Esophageal Atresia Treatment
- 11 Esophageal Atresia Prognosis
- 12 Esophageal Atresia Complications
The term “Atresia” means ‘lack of any normal gap’. Esophageal Atresia is an uncommon medical condition wherein a part of esophagus (the long tube that joins the mouth to the stomach) is not present in the body of an infant. This disorder occurs along with tracheoesophageal fistula, a condition where the esophagus is connected to the trachea (the tube which joins the nasal region to the lungs).
This condition is also known as “Oesophageal Atresia”.
Esophageal Atresia ICD9 Code
The ICD9 code for this syndrome is 750.3.
Esophageal Atresia Incidence
It occurs in 1 out of 4000 births. It generally occurs with Tracheoesophageal Fistula in the body of a sufferer. However, a new born baby may have fistula with no atresia or vice-versa. Although a rare disease by nature, EA is considered to be the 25th most common birth disorder in the world.
Esophageal Atresia and Tracheoesophageal Fistula
EA, along with Tracheoesophageal Fistula (Fistula is an irregular channel between two internal organs of the body), is a common disease occurring among newborns in the US. Family doctors and physicians should provide necessary treatment for affected babies who face severe feeding difficulties and respiratory problems during the first few days of their life. Generally, one out of every 3000 to 4000 newborns are found to suffer from these two conditions.
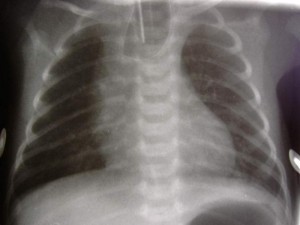
Picture 1 – Esophageal Atresia
EA occurs when a part of the upper esophagus is segmented while Tracheoesophageal Fistula develops when the trachea (the windpipe that carries air to the lungs) gets connected with the esophagus. Both of the conditions require surgical repair, which should be initiated immediately after birth. Surgery is done when an affected child is asleep and injected with anesthesia.
However, there are few risks involved with a surgical treatment. The risks include:
- Excessive bleeding during operation
- Possibility of infection
- Low body temperature
- Shrinkage of lungs
Esophageal Atresia Classification
This condition can be further classified into various forms, namely:
- Pure, Long Gap or Isolated EA
- EA with proximal Tracheoesophageal Fistula
- EA with distal Tracheoesophageal Fistula
- EA with both distal and proximal Tracheoesophageal Fistula’s
- Only TEF with no EA, but with presence of an unsighted small pouch and Hageal Atresia
- Esophageal Stenosis
Congenital Esophageal Atresia
It is a condition acquired during fetal development. It is characterized by the inability of the esophagus to evolve as a normal passage between the mouth and the stomach. It eventually closes in a blind pouch.
Esophageal Atresia Causes
The actual cause of this congenital syndrome is unknown. An infant born with this condition appears normal in the initial stage. Later on, saliva and mucus passing through the stomach fill the blind pouch. These emissions in the nasal and mouth area lead to drooling and cause feeding problems in the baby.
Esophageal Atresia Symptoms
A number of symptoms indicate the presence of EA in the body of a patient. These comprise of:
- Drooling
- Feeding problems
- Bluish discoloration of skin during attempts to feed
- Gagging, coughing and choking during attempts to feed
Esophageal Atresia Diagnosis
EA is generally diagnosed immediately after birth. A sound diagnosis helps physicians provide patients with an effective treatment. Following are the different types of diagnosis and tests done on patients to find the existence of EA syndrome:
Ultrasound
It should be done on a pregnant woman before birth of her child, to determine the exact amount of amniotic fluid present in the body. Excess amniotic fluid indicates the presence of EA in a patient.
X-Ray
It is usually performed on the esophagus to detect any air-filled pouch in the intestine and stomach of an affected patient.
Feeding Tube
This disorder can be easily detected by a feeding tube. In an infant with EA, any attempt to pass a feeding tube into the stomach via nose or mouth is met with obstruction.
Esophageal Atresia Treatment
The exact treatment of this disorder depends on its severity. Infants affected with this syndrome generally fail to survive unless a surgical rejoining of the esophagus is performed. Surgery is considered to be the best option for reconnecting the two extreme ends of the esophagus of a suffering infant. The best time for an operative treatment is between 2 and 6 months after birth. However, prematurity, aspiration, pneumonia and other birth disorders can postpone a surgical cure.
Esophageal Atresia Prognosis
The outcome of this ailment depends on the associated complications and abnormalities. With proper treatment, the survival rate can be as high as 90%. Proper growth occurs after a good treatment. Late mortality generally occurs due to respiratory problems while early mortality is caused by cardiac abnormalities.
Esophageal Atresia Complications
An infant with EA may swallow fluids such as saliva inside the lungs, which can result in choking, aspiration pneumonia and even death in few cases. In a few cases, prematurity can further complicate the situation. Some other possible complications include:
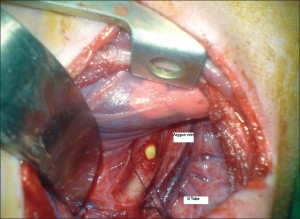
Picture 2 – Esophageal Atresia Image
- Scarring (arising due to surgery), which causes contraction of the esophagus
- Repetitive uplifting of food from the stomach after surgery
- Kidney, heart and stomach problems
If any newborn in your family exhibits constant feeding problems and vomits repetitively after food intake, call your health care provider without delay. With right medication and care, this congenital disorder can be cured in time – ensuring faster recovery for sufferers.
References:
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001957/
http://en.wikipedia.org/wiki/Esophageal_atresia
http://www.patient.co.uk/doctor/Oesophageal-Atresia.htm
http://medical-dictionary.thefreedictionary.com/esophageal+atresia