What is Idiopathic Thrombocytopenic Purpura?
Page Contents
- 1 What is Idiopathic Thrombocytopenic Purpura?
- 2 Idiopathic Thrombocytopenic Purpura Epidemiology
- 3 Idiopathic Thrombocytopenic Purpura Classification
- 4 Idiopathic Thrombocytopenic Purpura Causes
- 5 Idiopathic Thrombocytopenic Purpura Symptoms
- 6 Idiopathic Thrombocytopenic Purpura Diagnosis
- 7 Idiopathic Thrombocytopenic Purpura Differential Diagnosis
- 8 Idiopathic Thrombocytopenic Purpura Treatment
- 9 Idiopathic Thrombocytopenic Purpura Treatment Complications
- 10 Idiopathic Thrombocytopenic Purpura Prognosis
- 11 Idiopathic Thrombocytopenic Purpura Prevention
- 12 Idiopathic Thrombocytopenic Purpura Pictures
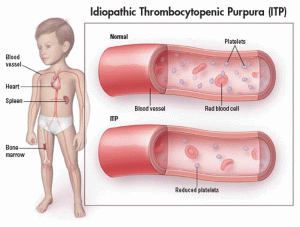
Idiopathic thrombocytopenic purpura (ITP) is a condition characterized by the presence of unusually low platelet count or thrombocytopenia of an idiopathic or unknown cause. As most cases of ITP seem to be associated to the manufacturing of the antibodies against the platelets, the condition is also known as immune thrombocytopenia or immune thrombocytopenic purpura. ITP can be frequently asymptomatic and only discovered incidentally; however a severely low platelet count might lead to increased chance of purpura and bleeding. Some of the other names for this condition include:
- Morbus haemorrhagicus maculosus
- Splenic thrombocytopenic purpura
- Purpura haemorrhagica
- Thrombocytolytic purpura
Idiopathic Thrombocytopenic Purpura Epidemiology
ITP affects both boys and girls equally, although the gap widens as they tend to become more mature. The ratio of male to female adult patients is around 1:1.2 to 1:7. The average age in which this condition is first detected falls roughly between 56 and 60.
Idiopathic Thrombocytopenic Purpura Classification
ITP can be of two types:
Acute ITP
This form of the disorder develops suddenly and generally follows some viral condition in a child. Acute form of ITP may not require any treatment, if there is low bleeding and the number of platelets does not decrease significantly. The condition generally shows spontaneous improvement and rarely shows any signs of relapse in children.
Chronic ITP
This type of ITP develops over a long time, is much more long lasting and is generally found in adults. The condition may not require treatment if the platelet count does not pose a major risk of bleeding. Participating in various contact sports or handling manual work should be done with care.
Idiopathic Thrombocytopenic Purpura Causes
ITP occurs when certain specific immune system cells develop antibodies against the platelets. Platelets assist in clotting of blood by clumping together and blocking small holes in the damaged blood vessels. Antibodies get attached to the platelets and the spleen damages the platelets carrying the antibodies. The immune system generally protects the body from diseases and infections. However, it destroys the body’s platelets in ITP sufferers. The exact causes for this are not known, although some probable factors have been suggested.
The various probable factors that lead to the development of this disorder have been listed below:
- An abnormal autoantibody (such as immunoglobulin G) binds to platelet membrane leading to the spleen’s removal.
- HIV infections
- Helicobacter pylori infections
- Lymphoproliferative disorders like non-Hodgkin’s lymphoma and chronic lymphocytic leukemia
- Collagen vascular diseases, like Systemic lupus erythematosus
- Drugs like heparin, sulfonamides, quinine
- Toxins like ethanol
- Acute hepatitis
- Herpes group infections
- Relapsing dengue fever
- Hodgkin’s disease
- Tuberculosis
The disease can sometimes have a viral connection in children. In adults, ITP occurs more frequently after some viral infection that develops to a chronic stage (long-term). It can also be induced by the usage of certain drugs, at the time of pregnancy or in association with some autoimmune disorder.
The factors that may increase the risk of development of ITP include:
- Very low platelet count
- Acute viral sickness
- Aging
- Hypersplenism
- Cardiopulmonary bypass
- Antiphospholipid antibody syndrome
Idiopathic Thrombocytopenic Purpura Symptoms
Immune thrombocytopenia might not cause any symptoms (asymptomatic). However, the condition can lead to internal bleeding or bleeding within the body or external bleeding from or underneath the skin. Signs of such bleeding may include:
- Development of bruises or purplish areas over one’s skin or the mucous membranes which are known as purpura; they are caused by sub-dermal bleeding. Reasons for such bleeding are not known.
- Possible development of Hematomas under the skin. These are clusters of clotted or partly clotted blood that grow under the skin and have the look or feeling of a lump.
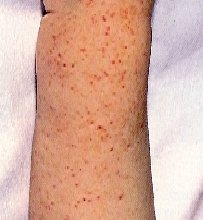
- Red spots known as petechiae are seen on the skin. They often develop in clusters and may resemble rashes. These spots are also caused by sub-dermal bleeding.
- Bleeding of the gums during a dental work or nosebleeds
- Blood found in one’s stool or urine
Any form of bleeding that is difficult to stop could indicate ITP. This also includes menstrual bleeding that is heavier than normal. Cerebral bleeding is very rare with variable symptoms.
Low platelet count does not directly lead to pain, difficulty in concentration or any other problems. However, it might be linked with tiredness or fatigue.
Idiopathic Thrombocytopenic Purpura Diagnosis
ITP is diagnosed through a procedure of exclusion. Firstly, the doctor will have to conduct a thorough physical examination and determine that no signs of any blood abnormalities are present other than a low platelet count. No physical signs are expected either except for the regular signs of bleeding. The secondary causes, which are seen in about 5 to 10% of all suspected cases of ITP, include:
- Medications
- Leukemia
- Cirrhosis
- Lupus erythematosus
- Hepatitis C
- HIV
- Antiphospholipid syndrome
- Congenital factors
- Onyalai
- Deficiency caused by von Willebrand factor
These factors should be excluded as well. In around 1% of cases, ITP co-exists along with autoimmune hemolytic anemia in a condition commonly referred to as the Evans Syndrome.
The spleen is generally not enlarged even though the platelets are destroyed by splenic macrophages. In fact, the presence of an enlarged spleen must lead a physician to explore other possible factors that might have led to the development of thrombocytopenia. ITP patients normally experience prolonged episodes of bleeding. However, the practice guidelines issued by American Society of Hematology discourages the usage of bleeding time while diagnosing idiopathic thrombocytopenic purpura. The normal bleeding time generally does not exclude platelet disorders.
Bone marrow examination can be performed on the patients who are above 60 years of age and those who show no response to treatment, or if the diagnosis is doubtful. A doctor may find signs of increased production of megakaryocytes while examining the bone marrow, which may conclusively suggest ITP. Analysis of the anti-platelet antibodies can be conducted; although that rests on the preferences of the physician.
The standard tests for the diagnosis of ITP include the following:
- Complete blood count test
- Blood clotting tests like PT and PTT
- Bone marrow biopsies
- Blood smear tests
Idiopathic Thrombocytopenic Purpura Differential Diagnosis
The differential diagnosis for the ITP includes ensuring the absence of the following health issues that might give rise to similar symptoms in sufferers:
- AIDS and other HIV infections
- Disseminated intravascular coagulation
Idiopathic Thrombocytopenic Purpura Treatment
An individual is treated for ITP if his or her blood work shows a platelet count less than 20000 per μl. Patients having a platelet count range between 20000 and 50000 per μl are normally evaluated on a per case basis, and except only in some rare instances, sufferers showing a count above 50000 per μl do not require any treatment. Hospitalization might be recommended for patients with very low platelet counts, and especially so in cases where significant mucocutaneous or internal bleeding has developed. Platelet count less than 10000 per μl is considered as a medical emergency; an affected individual might feel vulnerable to intracerebral or subarachnoid hemorrhage because of some moderate head trauma. Treatment is generally administered under recommendations of a hematologist and might be different for pediatric and adult cases of ITP.
Steroids
Usage of steroids makes up the basic form of treatment for this disorder. This group of medications helps to suppress the immune system. The mode of administration and dosage is determined by platelet count and if there is any active bleeding. Infusions of methylprednisolone or dexamethasone can be carried out in emergency cases. Milder forms may be treated with oral prednisolone or prednisone. After the platelet count has been improved, the dosage of steroids is reduced gradually and relapses if any are monitored. Nearly 60% to 90% of people experience relapses at the time of dosage reduction or cessation. A long-term usage of steroids is not recommended as it can cause various side effects.
Anti-D Immunoglobulin
Treatment of ITP can be conducted by administering Anti-D medications in case of Rh-positive patients. Anti-D or Rho(D) immune globulin is administered intravenously to these patients. It is also normally given to Rh-negative women during their pregnancy or after an Rh-positive infant is born in order to prevent the sensitization to Rh-factor in a newborn. The Anti-D medications have proven their effectiveness on some of the ITP patients. However, the procedure is costly, producing improvements only for a short term and not recommended for the patients recovering from a splenectomy procedure.
Steroid-sparing agents
Immunosuppressant medications like azathioprine and mycophenolate mofetil are growing in popularity due to their effectiveness in handling cases of ITP. In issues like chronic refractory problems where immune pathogenesis has already been established, a chemotherapeutic agent known as vincristine may be used. However, vincristine (a vinca alkaloid) produces serious side effects and hence it should be used only with caution in the treatment of idiopathic thrombocytopenic purpura. This is especially so for children as they are more vulnerable to its ill effects.
Intravenous immunoglobulin can be used in some cases as a mode of treatment for ITP. Although this method of treatment is costly and is effective only for a short period of time, it can be used for patients who are scheduled for surgery, have a critically low count of platelets as well as shown poor response to other forms of treatment to increase platelet count and minimize the bleeding risks.
Thrombopoietin receptor agonists
These are pharmaceutical agents which can be used to cure ITP. They induce production of platelets instead of trying to hinder platelet destruction. Thrombopoietin receptor agonists prevent bruising and bleeding by increasing platelet production in the bone marrow. Romiplostim, sold under the brand name of Nplate and Eltrombopag is available under the names of Promacta and Revolade. These are the examples of two well known thrombopoietin receptor agonists.
Surgery
Removal of spleen or splenectomy can be considered as a surgical option for treating idiopathic thrombocytopenic purpura. The procedure is risky in cases of ITP as it can cause severe bleeding during surgery. Splenectomy can be followed by durable remission in around 60% to 65% cases of ITP, and even less so for older patients. With the advent of various pharmaceutical remedies and steroid therapy, the usage of splenectomy as a mode of treating idiopathic thrombocytopenic purpura has been diminished to a large extent.
Transfusion of Platelets
Platelet transfusion is generally not recommended apart from emergency cases. It is also not effective enough to produce a long-term increase in platelet count. This is due to the fact that the autoimmune mechanism responsible for destroying the platelets also attacks the donor platelets.
Eradication of Helicobacter pylori
People living in areas having a high presence of the Helicobacter pylori bacterium should be targeted for treatment aimed at removal of this microbial agent, as this has shown promise in improving platelet count in many patients. In some cases, it was possible to bring back the platelet count back to normal. Tests like stool antigen testing and urea breath testing are more effective for these patients than tests based on serology. In fact, serology may show false positive results after an IVIG treatment.
There are certain other modes of treatment which are now still at an experimental stage. These include usage of the anti-infective sulfone drug called Dapsone, the chimeric monoclonal antibody known as rituximab and kinase inhibitor known as tamatinib fosdium (R788).
Idiopathic Thrombocytopenic Purpura Treatment Complications
The various treatment procedures used for curing ITP can have certain ill effects on the patients’ overall health. These treatment-related complications have been discussed below:
- Long-term usage of steroids may cause several negative side effects, such as depression, diabetes, increased appetite, weight gain, indigestion, high blood sugar, facial puffiness, indigestion, high blood pressure, chickenpox, cataracts and osteoporosis.
- Vincristine has been known to cause serious side effects and so their usage in case of pediatric patients should be limited.
- The surgical procedure of splenectomy can cause severe bleeding in a patient already affected by idiopathic thrombocytopenic purpura.
Usage of thrombopoietin receptor agonists can have various after-effects, such as:
- Headache
- Dizziness
- Vomiting
- Nausea
- Pain in joints or muscles
- An increased propensity for blood clots
Idiopathic Thrombocytopenic Purpura Prognosis
Proper treatment ensures a high chance that no remission will take place. In some rare cases, ITP can develop into a long-term condition that affects adults and relapse even after a period free of symptoms. The outcome, although generally good, is variable and depends on the intensity of the symptoms. Individuals may respond differently to the same mode of treatment.
Idiopathic Thrombocytopenic Purpura Prevention
Although ITP cannot be prevented, an individual can follow certain recommendations that might help him or her to avoid unnecessary complications. These include:
- Consulting doctor regarding medications that are considered safer. A doctor might advise to stay away from medicines like aspirin and ibuprofen that may affect the platelet count and increase chances of bleeding.
- Taking protection from bleeding or bruising.
Idiopathic Thrombocytopenic Purpura Pictures
Here are some pictures that would give you a clearer idea about the nature of this health condition.
Idiopathic thrombocytopenic purpura develops as a result of extremely low platelet count due to some unknown causes. Although it might be difficult to find out the underlying causes of the disorder, proper treatment can effectively cure an individual of this condition, blocking the risks of a possible relapse.
References:
http://www.nlm.nih.gov/
http://emedicine.medscape.com/
http://www.patient.co.uk/