Have you been lately suffering from pain and inflammation in your joints? Watch out, for the problems could be signs of an underlying condition known as Osteoarthritis (OA). Read and know all about this disease, including its varied causes, symptoms, diagnosis, treatment options and more.
Osteoarthritis Definition
Page Contents
- 1 Osteoarthritis Definition
- 2 Osteoarthritis ICD9 Code
- 3 Osteoarthritis Incidence
- 4 Osteoarthritis Symptoms
- 5 Osteoarthritis Causes
- 6 Osteoarthritis Diagnosis
- 7 Osteoarthritis Differential Diagnosis
- 8 Osteoarthritis Treatment
- 9 Osteoarthritis Home Remedies and Management
- 10 Alternative Treatment for Osteoarthritis
- 11 Osteoarthritis Risk Factors
- 12 Osteoarthritis Complications
- 13 Osteoarthritis Pictures
It is a very common disorder of the joints. It occurs due to degeneration of a joint as a result of excessive wear and tear or ageing.
The disease is also referred to by other names like:
- Osteoarthrosis
- Degenerative arthritis
- Degenerative joint disease
- Wear-and-tear arthritis
Osteoarthritis ICD9 Code
The ICD9 Code for this condition is 715.
Osteoarthritis Incidence
OA is the most common type of arthritis and the primary reason for chronic disability among the inhabitants of United States. It affects around 27 million individuals in the U.S and approximately 8 million people living in the U.K.
Osteoarthritis Symptoms
Although the condition may damage the joints in any region of the body, it most commonly affects the joints in the neck, hands, lower back, hips and knees.
The most signs and symptoms of this disease include:
Pain
Patients may suffer from painful sensations in the affected joint during or after movement.
Stiffness
The stiffness in the joint may be most prominent after waking up in the morning or following a period of inactivity.
Tenderness
Patients may experience tenderness in the joint by applying pressure on it, even with a finger.
Grating sensation
Sufferers may also experience a grating sensation while using the impacted joint.
Loss of flexibility
The movement of the joint gets restricted due to the condition. OA sufferers may not be able to move the joint through its full range of motion.
Bone spurs
Additional pieces of bone may develop around the impacted joint and feel like firm lumps to touch.
Osteoarthritis Causes
The condition develops when the cartilage that acts as a cushion for the ends of the joint bones degenerate over a period of time. The cartilage – a firm, slipper tissue – is responsible for the near-frictionless motion of the joints. In OA patients, the slick cartilage surface turns rough. The cartilage ultimately degenerates completely, leaving the bones grate over bone and wear away due to constant friction.
Osteoarthritis Diagnosis
The diagnosis for OA usually begins with a physical examination of the affected joint. Doctors look for inflammation, redness and tenderness in the joint and also determine its range of motion. This may be followed by various imaging and laboratory tests.
Imaging tests
These may involve:
MRI (Magnetic Resonance Imaging) Scan
This test makes use of a strong magnetic field and radio waves to produce detailed images of the soft tissues (including the bone cartilage) and bone. This can be useful in finding out the exact cause of pain in sufferers.
X-rays
This exam does not reveal cartilage. However, it can help determine the loss of cartilage by showing a narrowing space between the affected joint bones. This helps to confirm the development of OA. X-rays may also reveal bone spurs in the region surrounding a joint. OA is confirmed in many individuals on the strength of X-ray images even before they experience any signs of the disease.
Lab tests
These include:
Joint fluid analysis
In this test, physicians use a needle to extract fluid out of the impacted joint. This fluid sample is then tested in a laboratory to assess a possible inflammation and whether the pain is the result of other problems such as an infection or gout.
Blood tests
Examination of the blood of patients helps ensure the absence of other causes of joint pain, like Rheumatoid arthritis.
Osteoarthritis Differential Diagnosis
The differential diagnosis for OA includes excluding the possibility that the symptoms experienced by sufferers are the result of the condition itself and not some similar disorders, such as:
- Fibromyalgia
- Ankylosing Spondylitis
- Gout and Pseudogout
- Avascular Necrosis
- Patellofemoral Arthritis
- Psoriatic Arthritis
- Rheumatoid Arthritis
- Lyme Disease
- Imaging in Neuropathic Arthropathy (Charcot Joint)
In individuals suffering from knee pain, physicians should also have to take Prepatellar bursitis Patellofemoral syndrome into account.
Osteoarthritis Treatment
The symptoms of OA usually tend to worsen with time, as there is no actual cure for the condition. The treatment options for this disease usually slow down its progression, improve the functioning of joints and provide patients with relief from pain.
The treatment options for OA include:
Medicines
The drugs used to manage OA symptoms involve:
Acetaminophen
The drugs of this category, such as Tylenol, help provide sufferers with relief from pain although they are unable to decrease swelling in a joint affected by OA. Such medications have been found to be effective in OA patients with painful sensations of mild to moderate intensity. Intake of this drug in higher than the recommended doses can result in liver damage.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
These medicines alleviate painful sensations and reduce inflammation in the impacted joint. While sufferers can avail NSAIDs like naproxen (Aleve) or ibuprofen (Advil, Motrin) over-the-counter, stronger medicines of this form have to be bought by prescription. However, these medicines may give rise to various side effects like:
- Bleeding
- Stomach upset
- Liver damage
- Kidney damage
- Cardiovascular problems
- Ringing sensation in the ears
Older patients are most susceptible to these side-effects.
Narcotics
These are prescription drugs that usually comprise of substances similar to codeine that alleviate severe painful sensations in OA sufferers. Although these are extremely useful for OA patients with acute pain, there is a risk of dependence associated with these medications that are stronger in intensity. The side effects may include:
- Sleepiness
- Nausea
- Constipation
Osteoarthritis Home Remedies and Management
The home remedial measures for this disorder, that can help patients in the management of its symptoms, include:
Rest
Resting the swollen and painful joint for 1 day can lower the intensity of the symptoms. Patients should avoid all activities that put their affected joint under stress.
Regular exercise
Regular exercise can strengthen the muscles around joints, making them more stable. It is better to perform gentle exercises like biking, swimming or walking that do not tax the joints. If the joint pain is fresh, sufferers should stop immediately. Pain arising after an exercise session usually indicates that the workout has been overdone.
Losing weight
Greater body-mass puts the weight-bearing joints, such as the hips or the knees, under greater stress. Even a minor loss of body weight can greatly help in providing such joints with relief and reduce the symptoms of OA and similar disorders. It is wise to consult a physician about proper steps to lose weight. Many individuals manage to address their obesity issues with increased level of exercise coupled with dietary changes.
Heat and cold application
Application of heat and cold can provide relief from joint pain. Heat alleviates stiffness while cold relieves muscular spasms.
Application of over-the-counter creams
Some patients find temporary relief from pain with the aid of over-the-counter gels and creams. These induce numbness into the affected region by producing a sensation of warmth or coolness. Certain creams contain medicines such as aspirin-type of components that get absorbed into the affected skin area on application. Analgesic creams have the best effect on joints that are located close to the skin surface, such as in the fingers or the knees.
Use of supportive devices
Supportive devices can help OA patients carry out daily activities without putting their affected joints under stress. Walking sticks, canes or crutches may help in moving about by taking the body weight off the hip or the knee. You may consult your physician or occupational therapist about the types of supportive equipments that may help you.
Alternative Treatment for Osteoarthritis
Some OA patients may find relief from alternative curative measures such as:
Yoga
These involve gentle stretching exercises, combined with deep breathing, that reduce stress and also make the joints move gently – thereby nourishing the cartilages.
Tai Chi
Similar to yoga, this type of exercise calms the mind and makes the joints function to an optimum extent. This helps cure OA symptoms arising due to inactivity.
Acupuncture
In this curative process, minute needles are inserted into the skin over various regions of the body. This helps cure many ailments. However, the method involves certain side effects in the form of pain, bruising and infection.
Use of nutritional supplements like Chondroitin and Glucosamine
There is controversy regarding the actual effectiveness of the intake nutritional supplements like Chondroitin and Glucosamine for OA sufferers. Those allergic to shellfish should not consume Glucosamine.
Osteoarthritis Risk Factors
The risk factors for this disorder include:
Sex
The condition clearly has a sexual preference with women being more susceptible to the disorder than men. The reason for this is not known.
Increase in age
The risk of development of this disorder increases with advancing age.
Joint injuries
Trauma or injury to the joints, such as those developing due to accidents or participating in sports activities, may elevate susceptibility to the disease.
Bone malformations
Certain individuals are born with deformed joints or malformed cartilage. This can elevate the risk of occurrence of OA.
Obesity
Greater body weight puts more stress on the joints that are under constant stress, such as those that bear the weight of the body, like the knees.
Disorders
The presence of certain disorders, such as Gout, diabetes or Paget’s disease of bone, may increase the development of the disorder. Having an underactive thyroid gland may also place patients at greater risk.
Certain professions
Individuals engaged in certain types of professions that put one or more specific joints of the body under repeated stress may make those more susceptible to OA.
Inactive lifestyle
The cartilage depends on the use of the joint it is associated with for nourishment. Keeping a joint inactive leads to the malnourishment of the cartilage associated with it. This ultimately makes it susceptible to OA.
Osteoarthritis Complications
As aforesaid, OA tends to worsen with time. Patients usually feel the stiffness and joint pain becoming severer with passing time, making execution of daily tasks more and more difficult for them. Some sufferers are no longer able to work after a time period. In cases of such severe impairment due to OA, physicians may recommend joint replacement operation.
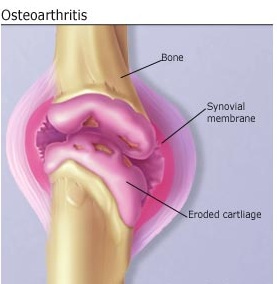
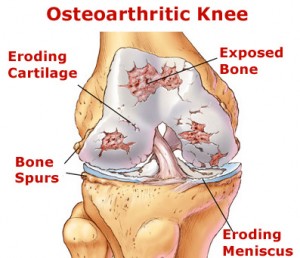
Osteoarthritis Pictures
The following images show how the joints are affected by this disorder.
Picture 1 – Osteoarthritis
Picture 2 – Osteoarthritis Image
Get in touch with a physician and get diagnosed immediately for OA if you are suffering from stiffness and inflammation in your joints that persist for over a few weeks.
References:
http://www.mayoclinic.com/health/osteoarthritis/DS00019
http://emedicine.medscape.com/article/330487-overview
http://www.nlm.nih.gov/medlineplus/osteoarthritis.html
http://www.webmd.com/osteoarthritis/default.htm
http://en.wikipedia.org/wiki/Osteoarthritis