Osteomyelitis Definition
Page Contents
- 1 Osteomyelitis Definition
- 2 Osteomyelitis ICD9 Code
- 3 Osteomyelitis Causes
- 4 Osteomyelitis Types
- 5 Osteomyelitis Risk Factors
- 6 Osteomyelitis Symptoms
- 7 Osteomyelitis Diagnosis
- 8 Osteomyelitis Treatment
- 9 Osteomyelitis in Children
- 10 Osteomyelitis Prognosis
- 11 Osteomyelitis Complications
- 12 Osteomyelitis Prevention
It is an infectious disorder of the bone, or the bone marrow, caused by germs such as bacteria.
Osteomyelitis ICD9 Code
The ICD9 Code for this disorder is 730.
Osteomyelitis Causes
The majority of cases of this disease occur as a result of infection by the staphylococcus bacteria, a particular microbe that is often found in the nose or on the skin of healthy people.
The germs can enter a bone in various ways, such as:
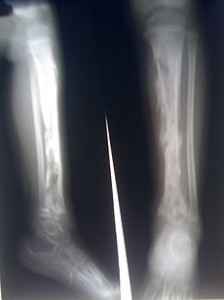
Picture 1 – Osteomyelitis
- From a nearby infected region
- Through the bloodstream
- Through direct contamination
Osteomyelitis Types
The condition is classified into various types, such as:
Vertebral Osteomyelitis
It is the most common infectious condition to affect the vertebral body inside the spine. It is a rare cause of back pain, particularly in young adults who are otherwise healthy.
Chronic Osteomyelitis
Unless treated in time, Osteomyelitis can turn chronic and cause permanent damage to the bones leading to persistent pain as well as loss of function.
Hematogenous Osteomyelitis
It is an infectious disorder resulting from bacterial seeding from the blood. Acute Hematogenous Osteomyelitis is the most common type of Osteomyelitis that develops in children. It can lead to life-long deformities of the musculoskeletal system.
Mandibular Osteomyelitis
It is a rare type of inflammatory disorder that arises in developed nations, due to the use of antibiotics and advances in medical treatment.
Salmonella Osteomyelitis
As the name indicates, it is a type of Osteomyelitis resulting from Salmonella infection. The condition is much more common in sickle-cell anemia sufferers than in the general population.
Dental Osteomyelitis
Also referred to as Osteomyelitis of the jawbone, it refers to a chronic or acute infection of the jawbone (mandible) that is generally caused by bacteria. The condition is very difficult to diagnose.
Osteomyelitis Risk Factors
The risk factors for this disorder include:
Hemodialysis
It refers to a dialysis of the blood to do away with metabolic or toxic wastes from the blood of patients. It is usually implemented in individuals with kidney failure. The process can leave the body vulnerable by providing easy access to the system for germs.
Recent trauma or injury
A deep puncture or an acute fracture of the bone makes it easy for germs and microbes to enter the bone or a tissue that is located close by. An attempt to surgically replace degenerated joints or repair fractured bones can also accidentally open the path for germs to enter the bone. Deep animal bites can also make it easy for infections to enter the system and cause long-time damages.
Disorders that weaken immunity
Poorly controlled diabetes weakens the immune system of its patients and increases the risk of Osteomyelitis. Hence, better management of diabetes is always recommended to sufferers of blood sugar disorder. Some other factors that can lead to a suppression of the immune system include organ transplant, chemotherapy and intake of corticosteroids or medications known as Tumor Necrosis Factor Inhibitors or TNF Inhibitors.
Strangely however, HIV/AIDS sufferers with severely weakened immunity are not found to be at an increased risk of having this disorder.
Poor supply of blood
Blocked or damaged blood vessels make it difficult for the body to distribute anti-infection cells necessary to prevent progression of a small infection. In such people, even a minor cut or injury can worsen and become a deep ulcer that can make bone or deep tissues vulnerable to infection. Blood circulation can be impaired due to poorly managed diabetes as well as other conditions like Sickle Cell disease and Peripheral Arterial Disease (which is often associated with smoking).
Use of illegal drugs in an injected form
Those who inject illegal drugs into their body are at greater risk of developing Osteomyelitis. This is usually due to the use of non-sterilized needles and non-sterilization of skin prior to needle perforations.
Osteomyelitis Symptoms
The condition is primarily characterized by the following signs and symptoms:
- Fever
- Pain in bone
- Localized redness, inflammation and warmth
- General ill-feeling or a sensation of not being well (malaise)
Some other associated symptoms include:
- Profuse perspiration
- Low back pain
- Chills
- Inflammation of the legs, ankles and feet
Osteomyelitis Diagnosis
The initial diagnosis for this disorder involves a physical exam, which can reveal possible inflammation, redness and tenderness of bone. This may be followed up by one or more of the following medical tests:
- Bone scan
- Bone x-ray
- Blood cultures
- Bone biopsy (which is then cultured)
- Erythrocyte sedimentation rate (ESR)
- MRI of the bone
- C-reactive protein (CRP)
- Complete blood count (CBC)
- Needle aspiration of the area around affected bones
Physicians may recommend a combination of exams to detect Osteomyelitis and assess which germ is the underlying cause of the infection. These include:
Blood tests
These exams may show a possible elevation in the white blood cell levels and also help determine other factors that may show whether the body of the patient is fighting an infection. A positive result can confirm an underlying infection. If a blood infection is responsible for Osteomyelitis, tests may show which germs are responsible. However, blood tests only give physicians a clue to the possible presence of Osteomyelitis and are non-effective in clearly confirming whether or not a person is suffering from the disorder.
Imaging tests
These involve:
X-rays
Such tests show whether or not a bone has suffered any damage or injury although the damage may not be apparent until a person has been suffering from Osteomyelitis for a number of weeks. If the condition is suspected to have developed more recently, further detailed imaging tests may be deemed as necessary.
Magnetic Resonance Imaging (MRI) Scan
These tests include the use of a strong magnetic field and radio waves. MRI scans help create highly detailed images of the bones and adjoining soft tissues.
Computerized Tomography (CT) Scan
It combines x-ray images obtained from various angles to make up cross-sectional views of the internal structures of a sufferer.
Bone biopsy
It is regarded as the gold standard for this disorder as it helps detect which specific type of germ has infected a bone. The knowledge of the type of germ responsible allows a physician to choose an antibiotic drug that is specifically effective in curing that type of infection.
An open biopsy needs surgery under anesthetic effects to access the bone. In some cases, a long needle is pushed through the skin and passed all the way into the bone. Local anesthetics are used to induce a sensation of numbness in the region where the needle is to be inserted. For guidance, x-rays or other types of imaging scans may be used.
Osteomyelitis Treatment
The aim of treatment for this disease is to cure infection and also lower damage to the bone and the adjoining tissues.
The most common treatment options for Osteomyelitis include:
Medications
A bone biopsy reveals the type of germ that results in infection. It helps physicians choose an antibiotic that is effective in curing that specific infection. The medicines are generally administered in an intravenous way for a minimum of 4-6 weeks. The side effects of these drugs may involve:
- Nausea
- Vomiting
- Diarrhea
An additional oral antibiotic course may also be necessary for treating more severe form of infections.
Surgery
The type of surgery depends on how severe the infection is. The operative procedures include:
- Draining the infected region
- Restoring flow of blood to the bone
- Removing any foreign materials
- Amputation of the limb
- Removal of the diseased tissue and bone
Hyperbaric oxygen therapy
This process may be effective in providing more oxygen to the bone and promoting healing in individuals affected by a type of Osteomyelitis that is very difficult to cure. The method helps deliver more oxygen to the area than is normally available in the surroundings. The technique involves usage of a pressure chamber that looks like a clear, large tube.
Osteomyelitis in Children
In children, the condition usually affects the long bones of the upper arm and the legs. Timely diagnosis and prompt treatment is necessary to ensure faster cure of the disorder. Lack of timely cure can complicate the disorder and lead to long-term problems in affected children, such as reduced growth and impaired functioning.
Osteomyelitis Prognosis
The outcome for even acute cases of this condition is good with proper treatment. However, prognosis is worse in cases of long-time or chronic sufferers of the disorder. The symptoms may appear and disappear for several years, even after surgery has been conducted. In some sufferers, especially those suffering from poor blood circulation or diabetes, amputation may be necessary.
The outcome for individuals with an infection of the prosthesis is based on:
- The form of infection
- The health of sufferers
- Whether or not the infected prosthesis can be removed in a safe way
Osteomyelitis Complications
The possible complications for this disease involve:
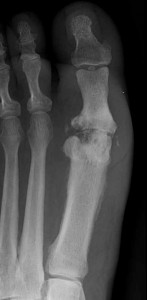
Picture 2 – Osteomyelitis Image
Septic arthritis
In some individuals with the disorder, the infection can spread to an adjacent joint from the bones.
Bone death
Also known as Osteonecrosis, it is an infection in the bone. It can obstruct the supply of blood within the bone, ultimately causing its death. This can be healed by carrying out an operation that removes small parts of dead bone. In case a large portion of the bone is found to have died, doctors may recommend amputation of the affected limb to prevent the spreading of the infection.
Skin cancer
If Osteomyelitis leads to the development of an open sore that is oozing pus, the skin of the adjoining region is at a greater risk of developing a malignant condition known as squamous cell cancer.
Reduced growth
In kids, the growth plates (softer regions of the ends of the long bones of the limbs) are the most common spots to the affected. If these plates are affected, the infected bones may have reduced growth.
Osteomyelitis Prevention
Patients informed about an elevated risk of being infected should consult with their physician about proper preventive measures to keep the infection at bay. Reduced risk of this infection can also lower the susceptibility to Osteomyelitis. Generally, suffering individuals are advised to avoid getting scraped or cut which can give germs an easy access to their body. Even if an area has been cut, patients should immediately clean the region and cover it with a clean bandage. The wounds should often be checked for any possible signs of infection. This measure even applies for unaffected individuals.
If you are suffering from worsening bone pain, along with fever, get in touch with a physician on an immediate basis. Proper and timely treatment can prevent the risks of infection and help you elevate your chances of an early recovery.
References:
http://www.mayoclinic.com/health/osteomyelitis/DS00759
http://en.wikipedia.org/wiki/Osteomyelitis
http://www.nlm.nih.gov/medlineplus/ency/article/000437.htm
http://www.nhs.uk/conditions/Osteomyelitis/Pages/Introduction.aspx