What is Parry Romberg Syndrome
Page Contents
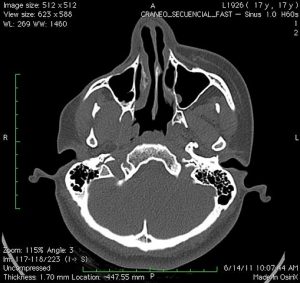
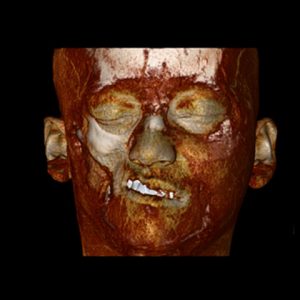
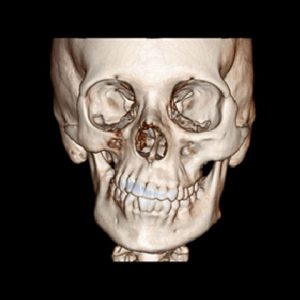
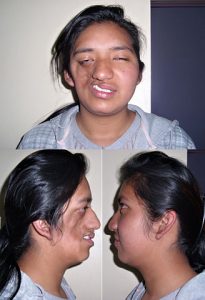
Parry Romberg syndrome (PRS), named after the English physician Caleb Parry, is a rare progressive disorder, characterized by slow atrophy or wasting away of facial soft tissues. It usually affects the left half of the face, but can occur on both sides in rare cases. Sometimes, the limbs on the same side of the body as the facial atrophy may also be affected.
Other names of the disorder include hemifacial atrophy (HFA), progressive hemifacial atrophy and progressive facial hemiatrophy.
Signs and Symptoms
The symptoms vary from person to person, ranging from mild to severe. They generally appear between ages 1 to 15, progress within the next 2 to 10 years before attaining a stable phase.
The most characteristic symptom involves leaning of the mouth, nose and other facial features towards one side, due to atrophy. Other abnormalities that occur with progression of the disease include:
Ear Abnormalities
- Unusual shrinking of the ear on the affected side
- Protrusion of the affected ear from the head
Scalp and Hair Symptoms
- Bald patches on the scalp
- Absence of hair from the middle part of eyebrows
- Unusual whitening (blanching) of hair
- Absence of eyelashes
- Whitening and falling out of facial hair
Mouth and Teeth Anomalies
- Atrophy of the upper lip or one side of tongue
- Shortening of lower jaw bone on the affected side
- Difficulty opening or closing jaws
- Twisted or raised appearance of one side of upper lip
- Abnormal or late exposure of certain teeth, presence of atrophic roots
- Inappropriate meeting of upper and lower teeth
Skin Abnormalities
- Darkening or lightening of affected skin areas indicating hyper- and hypo-pigmentation
- Development of white patches (vitiligo)
Eye Anomalies
- Sunken appearances of both eyes (enophthalmos)
- Differences in the coloration of the two eyes (heterochromia)
- Inflammation of the uvea (the iris, and middle eye portion)
Neurological Symptoms
- Migraine headaches
- Nausea and vomiting
- Sensitivity to light
Rare Symptoms
- Jerky muscle movements suggesting contralateral focal seizures
- Paresthesia or a pricking or burning sensation in the face
- Trigeminal neuralgia or severe pain in face including areas such as the mouth, nose, and cheek
- Jaw spasms
Causes
The exact cause of this disorder is not known, and among the varied theories, one points out that the disorder may result from an autoimmune reaction, produced by inflammation in the nerves supplying skin and fat. This theory is also supported by the fact that antinuclear antibodies have been found in the serum of some affected people. Actually, certain proteins called antibodies are produced by the immune system to destroy any harmful foreign materials and protect the body. When the antibodies start attacking healthy tissues by mistake, they are called autoantibodies, and the process in turn generates an autoimmune reaction, leading to conditions like the PRS.
Other theories proposed as the possible causes of PRS are inflammations of the sympathetic nervous system, brain and meninges, and defects in the formation of blood vessels.
Risk Factors
It is more likely to affect women than men. Other risk factors include:
- Trauma of head or face
- Viral infections
- Heredity
- Endocrine disturbances
Complications
- Keratitis
- Atrophy of the optic nerve
- Ipsilateral atrophic changes
- Contralateral atrophic changes
- Iritis
- Facial palsy
- Trigeminal neuralgia
- Epilepsy
- Psychiatric complications
Diagnosis and Tests
- Physical examination
- Brain’s MRI or magnetic resonance imaging scans
- Lumbar puncture
- CT scan
- Autoantibodies serum test
Differential Diagnosis
- Linear scleroderma
- Idiopathic facial palsy
- Rasmussen syndrome
- Goldenhar syndrome
- Hemifacial microsomia
- Berardinelli-Seip congenital lipodystrophy
- Partial acquired lipodystrophy
Treatment and Management
Since no treatments are available to stop the disorder from progressing, certain therapies are undertaken to manage the symptoms and associated conditions, including:
Medical Therapy
Medications that may provide relief from migraine pain and seizures include immunosuppressive drugs such as corticosteroids, azathioprine, cyclophosphamide and methotrexate.
Surgical Procedures
Micro-Vascular or Reconstructive Surgery
This surgery, done to regenerate the wasted tissues, is generally planned after one or two years of the onset of the condition when the disease has exhausted and facial growth is complete.
Microsurgical Reconstructive Surgery
In this surgery, tissues from certain body parts (such as free groin flaps or the rectus abdominis muscle) are transferred to the face to cover up the deformities.
Additional surgical options for severely affected patients are:
- Orthognathic surgery
- Cartilage grafts
- Bone distraction and grafts
Prognosis
The prognosis of the disorder varies from person to person. Mild cases do not create any aggravating or long term disabilities apart from some cosmetic deformities. Sometimes the condition subsides before affecting the whole face.
Incidence and Prevalence
It is estimated that 1 in 700,000 individuals may have PRS.
PRS ICD-9-CM Codes and ICD-10-CM Codes
The ICD-9-CM codes of PRS are 349.89, 351.8, while its ICD-10-CM code is G51.8