Are you vomiting blood or passing black, tarry stools very often? Chances are that you might be suffering from Portal hypertensive gastropathy. Read and know more about the types, causes, symptoms, diagnosis, and treatment of this disorder.
Portal hypertensive gastropathy Definition
Page Contents
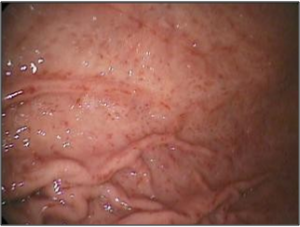
It is considered as an important cause of gastrointestinal bleeding in patients with or without cirrhosis. In this disorder, the mucosa of the stomach undergoes modification that includes friability and presence of dilated blood vessels at the surface. The gastric mucosa has a characteristic endoscopic appearance of mosaic-like pattern with or without red spots that closely resembles the skin of a snake. This disorder mainly occurs in the left portion of the stomach called as fundus. Sometimes, it may also occur in the gastric antrum. 65% of patients suffering from portal hypertension as a result of cirrhosis are affected by this disorder.
Portal hypertensive gastropathy Types
This particular condition develops through three distinct stages and can be classified on the basis of the extent of the disorder.
Picture 1 – Portal hypertensive gastropathy
Mild portal hypertensive gastropathy
It is characterized by a mosaic-like pattern without red spots.
Moderate portal hypertensive gastropathy
In this type of PHG, a typical mosaic-like pattern with intermittent red spots is observed.
Severe portal hypertensive gastropathy
In this form, a large number of red cherry-spots with the features of mild PHG are observed.
Portal hypertensive gastropathy Symptoms
Acute or chronic gastrointestinal bleeding is the primary feature of PHG. However, there are other symptoms of this disorder as well.
Esophageal varices
These are extremely enlarged sub-mucosal veins present in the lower section of the esophagus. They are most often a consequence of portal hypertension, due to cirrhosis and have a strong tendency to bleed.
Gastric varices
Development of dilated sub-mucosal veins of the stomach is an important manifestation of this disorder. Patients with bleeding gastric varices may also be prone to rectal bleeding.
Ascites
It refers to fluid retention in the abdominal cavity, and is the most common complication of PHG. It is always associated with liver disorders such as cirrhosis.
Melena
Patients frequently pass black, tarry stools as a consequence of gastrointestinal bleeding. During its passage through ileum and colon of the intestine, oxidation of the iron in hemoglobin causes the black color.
Hematemesis
Patients often vomit blood, the color of which may vary from bright red to coffee grounds.
Thrombocytopenia
It refers to a condition characterized by reduced platelet count in the bloodstream that leads to abnormal bleeding in the stomach. Platelets are cells in the blood that are responsible for clotting. Due to portal hypertension, more blood flows away from the liver and enters the spleen that traps these cells.
Leukopenia
Patients may register a low count of white blood cells that might lead to increased risk of infection.
Portal systemic encephalopathy
In this condition, there is an accumulation of toxins in the blood that affects the normal functions of the brain and nervous system. It is mainly caused due to shunting of blood away from the liver that ultimately reduces the ability of the liver to detoxify the blood.
Portal hypertensive gastropathy Causes
Pathogenesis of this disorder is not clearly defined. However, this gastric mucosal change has been associated to a few factors like:
Portal hypertension
High blood pressure in the portal vein leads to impairment in the defense mechanism of the gastric mucosa, resulting in increased flow of blood to the stomach. If it turns severe, the difference in blood pressure between the portal vein and the hepatic veins of the abdomen increases. This leads to a decrease in hepatic blood flow. This particular condition may have a negative impact on the body as the hepatic veins are responsible for draining de-oxygenated blood from the liver.
Noxious agents
Non-steroidal anti-inflammatory drugs like aspirin can cause gastric mucosal damage. Alcohol consumption directly leads to detrimental effects in the digestive tract, including gastrointestinal blood loss.
Activation of cytokines
Cytokines refer to molecular messengers such as TNF-alpha, which are responsible for regulating inflammatory response. These may induce nitric oxide and endothelin-1 to cause damage to the gastric mucosa.
Portal hypertensive gastropathy Diagnosis
The diagnosis of this particular disorder requires certain procedures and techniques that may aid in early detection.
Endoscopy
In this non-invasive technique, an endoscope is inserted into the stomach via mouth. Here, the mucosa displays mosaic-like or reticular pattern. The endoscopic appearance may often be misinterpreted as gastric antral vascular ectasia (GAVE). However, in GAVE, dilated blood vessels are found mostly in the antrum or lower portion of the stomach.
Biopsy
Generally suggested for this disorder by physicians, it is performed along with endoscopy which involves collecting small samples of gastric mucosal tissues for further examination. The damaged tissues show edema in the stomach wall that contributes to abdominal bleeding and a vast number of red blood cells in the lamina propria.
Stool test
This is generally conducted to detect presence of blood in stool, owing to abdominal bleeding. Passage of dark, tarry stools by the patients suggests some kind of gastrointestinal disorder. It is advisable to go for an endoscopic test post stool test because formation of bloody stools cannot be directly linked to PHG.
Imaging Studies
Portal hypertension is one of the main causes of PHG and can be detected in patients with the help of some imaging diagnostic methods. Duplex Doppler Ultrasonography is a low-cost, non-invasive method that provides complete information about the causes including portal vein dilation. Magnetic resonance imaging (MRI) and computed tomography (CT) are not widely used techniques but may provide some information.
Portal hypertensive gastropathy Treatment
An array of treatment options are available that may prevent further damage from this chronic gastrointestinal bleeding. These include:
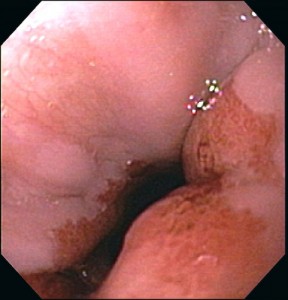
Picture 2 – Portal hypertensive gastropathy Image
Beta-blockers
These are a group of prescription drugs responsible for counteracting the stimulatory effects of beta receptors. This is generally followed by a reduction in pressure in the blood vessels of the body. In case of PHG, beta blockers may help in reducing the portal pressure of the portal vein. Propranolol and nadolol are the most commonly used non-selective beta-blockers for reducing the pressure of the portal vein in individuals suffering from esophageal varices.
Anti-fibrinolytic agents
These medications are predominantly used to treat gastrointestinal bleeding by preventing breakdown of blood clots. Deposits of fibrin, which are essential for clotting of blood, are stabilized by these reagents at various abdominal sites. Tranexamic acid is a commonly used anti-fibrinolytic agent.
Peptides
Octreotide, an octopeptide that mimics natural somatostatin, is often utilized in the treatment of PHG. Its main function is to contract the muscular walls of the portal vein that helps in reducing blood flow within the abdomen. It is extensively used for curing acute bleeding.
Argon plasma coagulation (APC)
It is an endoscopic procedure that is predominantly used to control bleeding from the dilated vessels of the abdomen. In this technique, a jet of ionized argon gas is administered through a probe, which is then passed through an endoscope. The probe is first placed near the bleeding site, and argon gas is emitted, which is in turn subjected to ionization by a high voltage discharge. High-frequency electrical current is then conducted through the jet of gas that causes coagulation of the blood on the other end of the jet.
Electrocautery
This particular procedure is used to stop bleeding from dilated vessels and eliminate them by using heat conduction from a metal probe that is heated by electricity.
Transjugular intrahepatic portosystemic shunt (TIPS)
In this procedure, under fluoroscopy guidance, an artificial channel called TIPS is established within the liver to connect the portal vein to one of the hepatic veins (veins that carry blood away from the liver back to the heart). A small, tubular metal device, known as stent, is then placed in this channel to keep the pathway open. There is a decrease in pressure over the liver which further reduces the portal venous pressure. This, in turn, lowers the pressure on the intestinal blood vessels to resist further bleeding.
Cryotherapy
In this process, pressurized carbon dioxide is directed through an endoscope that generates extreme cold to destroy the damaged tissues of the abdomen.
Portal hypertensive gastropathy can be cured with appropriate medical treatment, provided the diagnosis is done before it reaches a critical state.
References:
http://en.wikipedia.org/wiki/Portal_hypertensive_gastropathy#Clinical_findings
http://www.gastrosource.com/Patient-Cases/6805806/Portalhypertensive?itemId=7087665
http://www.medscape.com/viewarticle/708863
http://www.ajronline.org/content/175/6/1609.full