Have you been suffering from fever, abdominal pain and symptoms of bloody diarrhea? Watch out, for it could be a case of Schistosomiasis that you may be suffering from. Read and find out all about the disease, including its possible symptoms, causes, treatment options, complications and more.
Schistosomiasis Definition
Page Contents
- 1 Schistosomiasis Definition
- 2 Schistosomiasis ICD9 Code
- 3 Schistosomiasis Prevalence
- 4 Schistosomiasis History
- 5 Schistosomiasis Symptoms
- 6 Chronic Schistosomiasis
- 7 Schistosomiasis Causes
- 8 Schistosomiasis Risk Factors
- 9 Schistosomiasis Diagnosis
- 10 Schistosomiasis Differential Diagnosis
- 11 Schistosomiasis Treatment
- 12 Schistosomiasis Prognosis
- 13 Schistosomiasis Complications
- 14 Schistosomiasis Prevention
- 15 Schistosomiasis Pictures
It refers to an infectious condition caused by a form of parasite known as Schistosoma. The disorder is also referred to by various other names like:
- Bilharzia
- Bilharziosis
- Swimmer’s itch
- Snail fever
- Blood fluke
- Katayama fever
Schistosomiasis ICD9 Code
The ICD9 Code for this disorder is 120.
Schistosomiasis Prevalence
The disorder is not generally seen in the U.S. It is commonly reported in many subtropical and tropical regions around the world, especially of South America, Asia and Africa. Schistosomiasis is one of the most common parasitic infections in numerous regions of the world, second only to Malaria in prevalence. More than 200 million people across the world are reported to be annually affected by this disorder. It is categorized as one of the Neglected Tropical Diseases (NTDs).
Schistosomiasis History
The disorder is also known as Bilharzia, named after the doctor who described it for the first time in the mid-1800s.
Schistosomiasis Symptoms
The symptoms of this disorder tend to vary on the basis of the species of the parasite causing the condition as well as the duration of infection. In the initial stages of infection, patients tend to experience the following symptoms:
- Nausea
- Fatigue
- Abdominal pain
- Sores
- Fever
- Skin irritation
Initially, invasion of the skin may result in rashes (referred to as “Swimmer’s itch”) and itching. The Schistosome suffers destruction inside the skin in this disorder. Patients may also experience diarrhea, which may be bloody in case of some individuals. There may also be urinary problems like:
- Painful urination (Dysuria)
- Frequent urination
- Bloody urine (Hematuria)
Unless treated in time, the condition may cause patients to suffer from chronic ailments. There can be enlargement of spleen and liver. The eggs may enter the nervous system and give rise to various problems, such as seizures. The internal organs may also suffer damages.
Chronic Schistosomiasis
It refers to long-standing cases of Schistosomiasis that can arise months or even years after original exposure to the Schistosoma parasite. This happens due to the fact that adult Schistosoma worms, which are 1-2 cm in length, live in the veins surrounding the bowel and bladder for an average of duration of 3-5 years.
It can cause damage to a number of vital organs of the body, such as the kidneys, liver, bowel, bladder and genital tract.
Most people who develop chronic Schistosomiasis tend to experience its signs and symptoms several months or even years after being initially exposed to the parasite responsible for its occurrence. Chronic cases often give rise to complications in various organ systems like urinary system, liver, heart and gastrointestinal system. Those with chronic forms of the disorder may show improvement in their health condition when carefully treated with antiparasitic drugs and when their complications (associated with Schistosomiasis) are treated symptomatically.
Schistosomiasis Causes
This infectious condition may arise due to contact with water that has been contaminated by the Schistosoma parasite. Drinking from or swimming or washing in water sources contaminated by this parasite are frequently the causes of this disorder.
In its infective stages, the parasite is referred to as “Cercaria.” It freely swims in open water bodies. Upon being exposed to human skin, it burrows into the skin and matures into Schistosomula – another stage of infection. Then, it migrates to the liver and lungs where it gradually matures into adult forms.
Then, the adult worm migrates to any area of the body. This choice of body part depends on the type of parasite that it is. These regions involve:
- Bladder
- Liver
- Spleen
- Rectum
- Intestines
- Lungs
- Portal venous system (the veins responsible for transporting blood to liver from the intestines)
The symptoms of Schistosomiasis result from the natural response of the immune system to the parasitic eggs, rather than responses to the parasite itself.
Schistosomiasis Risk Factors
The risk factors of this disorder include the following:
Living in risk-prone areas
People born or living in regions, where the condition is prevalent, are naturally more susceptible to Schistosomiasis. Such individuals are naturally exposed to the Schistosoma parasite that is causative of this condition and develop the disease as a result.
Bathing or washing in the open
People washing or bathing out in the open from exposed water bodies, either due to habit or due to lack of resources, are also highly susceptible to the disease.
Being of a certain age
School-going children are at greater risk of being infected by the Schistosoma parasite as they often play or swim in water bodies that are contaminated by the microbe.
Poor hygiene
Living in or visiting areas with poor sanitation can also make an individual prone to developing this type of infection.
Schistosomiasis Diagnosis
The diagnosis of the disorder is performed by a physician or nurse. In the initial stages, this is performed by a physical examination of patients as well as a discussion about their medical history. Doctors also try to know whether or not sufferers have recently visited any tropical or subtropical region that is known for prevalence of Schistosomiasis. In regions where the infection is common, people who exhibit signs like bloody diarrhea may be assumed to be suffering from Schistosomiasis. In many cases, stools may be tested (stool examination) to check for the presence of parasitic eggs as some of these eggs are expelled by the body.
Additional diagnostic exams may include one or more of the following:
- Antibody test, to check for signs of infection
- Biopsy of tissue
- Liver function tests
- Kidney function tests
- Complete blood count (CBC) to determine any signs of anemia
- Urinalysis to look for parasite eggs
- Eosinophil count, to determine the number of some white blood cells
Schistosomiasis Differential Diagnosis
The differential diagnosis of this disorder involves isolating its symptoms from those of the following conditions that have similar signs. These include:
- Appendicitis
- Gastroenteritis
- Salmonella infection
- Urinary obstruction
- Inflammatory bowel disease
- Serum sickness
- Spinal cord infections
- Male urinary tract infection
- Female urinary tract infection
- Acute viral syndrome (including HIV)
- Pancreatitis
- Drug reactions
- Helminthic parasitic diseases
- Tropical splenomegaly
- Co-infection with malaria
- Co-infection with HIV
- Cirrhosis
- Pulmonary hypertension
- Co-infection with hepatitis B or hepatitis C
- Viral Hepatitis
- Leishmaniasis
- Gastroenteritis in Emergency Medicine
- Congestive Heart Failure and Pulmonary Edema
- Inflammatory Bowel Disease
- Myeloproliferative Disease
- Peptic Ulcer Disease
- Typhoid Fever
- Urethral Cancer
- Salmonella Infection in Emergency Medicine
Physicians should make sure that the signs exhibited by patients are not the result of any of the above-mentioned disorders.
Schistosomiasis Treatment
The treatment of this infection involves administering medicines to destroy the parasite responsible for the development of this disease. The infection is generally cured with the aid of the drug Praziquantel. However, the medicine can be difficult to obtain as well as expensive in regions where Schistosomiasis is endemic. Fortunately, many charitable organizations are working to make the drug more readily available in such areas as well as promoting adequate steps for prevention of the disorder.
In case of a severe infection or an infection that involves the brain, corticosteroids may be administered.
Cases of this disorder are usually curable with a single course of drug.
The groups that are typically targeted for the treatment of this disease include:
- Children of school-going age in endemic regions
- Risk-prone adults in endemic areas, including people engaged in occupations involving contact with contaminated water (farmers, fishermen and irrigation workers) and women engaged in domestic duties such as washing
- Whole communities living in areas considered to be highly endemic to Schistosomiasis
Schistosomiasis Prognosis
The outcome is generally good in cases where treatment is sought before acute damage or severe complications have occurred.
In the last 20 years, the disorder has been successfully controlled in a number of countries such as:
- China
- Brazil
- Egypt
- Cambodia
- Saudi Arabia
There is also evidence to suggest that the transmission of the disorder was interrupted in Morocco. In various nations, the assessment of the status of the transmission is being assessed. In the last 10 years, treatment campaigns have been upped in several Sub-Saharan nations with national coverage having been achieved in Uganda, Niger and Burkina Faso.
Schistosomiasis Complications
The possible complications of this disorder include the following:
- Seizures
- Bladder cancer
- Chronic kidney failure
- Right-sided heart failure
- Pulmonary hypertension
- Kidney and bladder obstruction
- Chronic liver damage and an enlarged spleen
- Inflammation of the colon (large intestine), along with bloody diarrhea
- Possibility of repeated blood infections, as bacteria can gain entry into the bloodstream through an irritated colon
Schistosomiasis leads to death only in rare cases. However, it can lead to illness and give rise to a variety of symptoms that are debilitating in nature.
When suffering from this disorder, affected individuals are at an elevated risk of developing bladder cancer.
Schistosomiasis Prevention
Snails are known to be an intermediate host for the Schistosoma parasite. Removing snails in water bodies used by humans can help avoid the occurrence of the infection. Other preventive measures for this disease include:
- Avoiding drinking from water bodies that are not known whether safe or not
- Avoid bathing or swimming in water bodies that are contaminated or potentially contaminated
People travelling to areas with a prevalence of Schistosomiasis should boil water before using or drinking it. They should also avoid swimming in freshwater as much as possible. Long-term steps can involve developing clean water reservoirs for use by members of communities.
Schistosomiasis Recommendations for Travelers
People travelling to endemic regions are advised to go through these preventive measures to avoid being affected by Schistosomiasis.
Things to do
Travelers should adopt the following steps to prevent the disease:
- Check whether they are going to regions with a prevalence of Schistosomiasis before traveling there.
- Ensuring that they use accommodations and water resources that are safe from potential parasite contamination. It is important to check whether a hotel, lodge or place of accommodation uses untreated water from a nearby lake as its resource.
- Swimming only in sea water or chlorinated swimming pools in areas with a prevalence of the disorder.
- Avoiding activities in endemic regions that may involve direct contact with water, such as swimming, paddling, snorkeling, diving or rafting
- Using boiled or packaged water and avoiding drinking from water sources that are open and exposed to parasitic contamination
- Visiting a general practitioner (GP) for screening tests if there is suspicion of being exposed to the Schistosoma parasite. Treatment on an early basis can stop the risk of long-term damage to the various organ systems of the body.
Things not to do
Travelers should avoid the following to prevent the occurrence of Schistosomiasis:
- Buying medications from overseas locations for curing the condition. These are often counterfeit and may produce adverse effects when taken too early or in wrong doses. The medication only works when used 8 weeks after original time of exposure to the parasite.
- Using insect repellents to avoid occurrence of infection. As yet, there is no evidence that use of repellents is effective. Also, the majority of repellents are water-soluble and likely to be washed off when in water.
- Depending on harsh towel drying of skin after contact with water. There is no reliable evidence that this is an effective way of removing the Schistosoma parasites.
- Relying on hotel staff or other travelers to know whether or not a source of water is affected. Rather, one should take steps to personally check and ensure whether or not the water resource is safe.
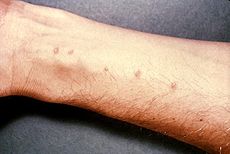
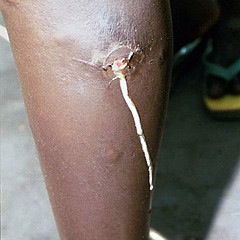
Schistosomiasis Pictures
Check out these images to know how sufferers of this disorder physically look like.
Picture 1 – Schistosomiasis
Picture 2 – Schistosomiasis
If you suspect yourself to be suffering from Schistosomiasis, seek medical attention as fast as possible. This would help you avoid complications of the disorder and check the condition in its very early stages, ensuring a faster recovery for yourself.
References:
http://www.nlm.nih.gov/medlineplus/ency/article/001321.htm
http://emedicine.medscape.com/article/228392-overview
http://www.wisegeekhealth.com/what-is-schistosomiasis.htm
http://en.wikipedia.org/wiki/Schistosomiasis
http://www.patient.co.uk/doctor/schistosomiasis