Silicosis is a hazardous disease affecting individuals of all developing or developed nations involved in stonecutting, metal mining, quartzmining, sandblasting or tunnel construction. Read and know all about the disease, including its possible causes, symptoms, treatment options and prognosis.
Silicosis Definition
Page Contents
- 1 Silicosis Definition
- 2 Silicosis ICD9 Code
- 3 Silicosis Incidence
- 4 Silicosis Types
- 5 Silicosis Causes
- 6 Silicosis Symptoms
- 7 Silicosis Risk Factors
- 8 Silicosis Diagnosis
- 9 Silicosis Differential Diagnosis
- 10 Silicosis Treatment
- 11 Silicosis Management
- 12 Silicosis Prognosis
- 13 Silicosis Complications
- 14 Silicosis Prevention
- 15 Desert Lung Disease
- 16 Silicosis Support Groups
- 17 Silicosis Pictures
It is a respiratory disease that occurs due to inhalation of crystalline silica dust. It is a type of Occupational Lung Disease.
The disorder is also referred to by the following names:
- Miner’s Phthisis
- Potter’s Rot
- Grinder’s Asthma
Silicosis ICD9 Code
The ICD9 Code for this disorder is 502.
Silicosis Incidence
According to a report published by the Center for Disease Control and Prevention (CDC) in 1996, as many as 1 million workers are exposed every year to crystalline silica. Of this population, over 250 people die from Silicosis.
As a result of greater awareness about the disease, enforcement of laws regarding maximum permitted dust levels in industry and use of protective wear, the incidence of new cases of the disorder is reducing in the U.S every year. Since regulations about the use of protective equipment have been implemented by the Occupational Safety and Health Administration (OSHA), the amount of silica dust inhaled by workers has been limited.
Silicosis Types
The disorder is classified into the following three types:
Simple Chronic Silicosis
It occurs as a result of prolonged exposure to low amounts of silica dust, generally for about 20 years. The dust of silica leads to an inflammation in the lymph nodes of the chest and in the lungs. This is the most common type of Silicosis. It is usually restricted to round, small spots in the lungs that can be seen in X-ray images.
Patients of this form of the disease may experience problems in breathing. Generally, sufferers are asymptomatic. The condition is found to be non-progressive once the exposure ends.
Accelerated Silicosis
It arises after exposure to high amounts of silica over a shorter duration, generally 5 to 15 years of time. In this form, the symptoms such as lung inflammation occur at a faster pace than in the simple form of the disorder.
Acute Silicosis
It arises as a result of short-term exposure to extremely high quantities of silica. The lungs get highly swollen and can be filled with fluid, resulting in low levels of oxygen in bloodstream and acute shortness of breath.
As per another classification, the disorder can be categorized into four types:
Chronic Simple Silicosis
It generally arises after 10-12 years of exposure to silica dust and is non-progressive after patients are not exposed to the irritant.
Chronic Complicated Silicosis
It occurs after 20 years or more of exposure to Silica dust. There is a progressive worsening of symptoms and damaged lung regions continue to grow in size even after there is an end to exposure.
Subacute Silicosis
It tends to arise after 3-6 years of acute exposure to silica and resembles the signs of Chronic Complicated Silicosis.
Acute Silicosis
It may arise after less than 2 years of heavy exposure to silica dust and is clinically different from the other forms.
Silicosis Causes
The condition, as already mentioned, arises as a result of exposure to silica – a crystalline substance that can be commonly found in natural surroundings. It is found in most rock beds. It forms dust which can come in contact with people who work in mines, tunnels and quarries or those who work with numerous metal ores. As Silica is the major constituent of sand, sand-blasters and glass workers are also exposed to the substance.
Silicosis Symptoms
The disorder generally gives rise to the following signs and symptoms in sufferers:
- Cough
- Weight loss
- Shortness of breath
Intense exposure to silica dust can result in disorders within a year. However, it generally takes a minimum period of 10-15 years of exposure prior to the development of the symptoms.
Silicosis and Progressive Massive Fibrosis
Progressive Massive Fibrosis is a pathological disorder of the lungs. The condition is characterized by acute scarring of lungs and destruction of normal lung structures. This condition may arise in either simple or accelerated forms of Silicosis, although it is more common in the accelerated type.
Progressive Massive Fibrosis is often compounded by chronic infection, especially Tuberculosis.
Silicosis Risk Factors
The risk factors for this disease involve the following:
Being in certain occupations
Some people are a higher risk of developing Silicosis due to constant exposure to silca dust, as a result of being involved in certain professions like:
- Blasting
- Road construction
- Building construction
- Tunnel construction
- Quartz mining
- Pottery
- Sandblasting
- Metal mining
- Foundries
- Stonecutting
- Abrasive manufacturing
Being of certain age
The disorder is generally identified in workers who are aged between 40 and 75 years of age.
Being male
Men have a tendency to develop the condition more than women as they are more involved in high-risk professions.
Silicosis Diagnosis
The diagnosis of this disorder involves a consideration of the medical history of sufferers. Doctors ask many questions to sufferers about their professions, hobbies and other activities that may have exposed them to silica dust. Physicians may also carry out a physical examination. It involves listening to sounds of breath with the aid of a stethoscope which may indicate blockage in the upper lobes of the lungs.
Additional tests to confirm the presence of the disorder and ruling out similar conditions include:
- Chest CT scan
- Chest X-ray
- Pulmonary function tests
- Serologic tests for connective tissue disorders
- Purified protein derivative (PPD) skin test (for Tuberculosis)
Some other tests for the condition, conducted in less common cases, may include:
- Pulmonary function tests, including lung volume measurement and Spirometry
- Arterial blood gases, to determine the efficiency of gaseous exchange in the lungs by the determination of levels of carbon dioxide (CO2) and oxygen in arterial blood
- Sputum culture, to detect the possible presence of any causative organisms and also for ruling out Tuberculosis
Silicosis Differential Diagnosis
The differential diagnosis of Silicosis includes isolating its symptoms from those of other similar disorders like:
- Sarcoidosis
- Tuberculosis
- Alveolar proteinosis
- Asbestosis
- Siderosis
- Stannosis
- Fungal pneumonia
- Lung cancer
- Lymphoma
- Metastatic carcinoma
- Lung diseases such as Pneumoconiosis
- Coal worker’s Pneumoconiosis
- Talcosis, caused by exposure to irritants
Silicosis Treatment
The disorder does not have any particular treatment. It is important to remove the source of Silica to prevent the worsening of the disorder. Cure mainly involves supportive treatment, which includes:
- Bronchodilators
- Cough medications
- Oxygen, if required
Antibiotic medications are prescribed for respiratory infections, as required. Other kinds of drugs used for the treatment of this disease involve anti-inflammatory medications (to decrease inflammation) and medications to widen the lung airways (Bronchodilators).
Treatment also involves reducing exposure to irritants, cessation of smoking and undergoing routine Tuberculosis (TB) skin tests.
Those with Silicosis are greatly susceptible to TB. Silica is supposed to interfere with the immune response of the body to the bacteria that is the causative agent of TB. Silicosis sufferers should undergo skin tests to help physicians determine the exposure to TB. Patients with a positive skin test should be cured with anti-TB medicines. Any alteration in the appearance of Chest x-ray may be an indication of TB.
People affected with severe cases of Silicosis may require a lung transplant.
Silicosis Management
The condition can be managed by the following measures:
Sleeping in a semi-upright position
It helps decrease the shortness of breath experienced by sufferers.
Stopping smoking
Smoking can worsen the symptoms of Silicosis and elevate the risk of lung cancer. Due to this reason, people suffering from Silicosis are urged to quit smoking.
Silicosis Prognosis
The outcome of this disease tends to vary on the basis of the amount of damage suffered by the lungs. Outcome is also dependent on other factors, such as:
- Duration of dust exposure
- Concentration of dust
- Size of silica dust particles that patients have been exposed to
If lung damage that is already present is permanent, the condition can cause permanent disability. The outcome tends to be less positive if complications occur or if Silicosis arises at any early age.
Although drugs cannot cure the underlying disorders, they can help give relief from the symptoms and let patients attain a complete recovery from Silicosis.
Drug therapy may help in recovery in cases where complications do occur. The amount of recovery, however, depends on the severity and the nature of the complications. Specific work restrictions, if any, are associated to the symptoms of affected individuals, particular work requirements and the presence of complications.
Silicosis Complications
The complications of the disorder may involve:
- Emphysema
- Lung cancer
- Stomach cancer
- Pneumothorax
- Other lung infections
- Respiratory failure
- Right-side heart failure (cor pulmonale)
- Increased risk for Tuberculosis (Silicotuberculosis)
- Progressive massive fibrosis (a variant of Silicosis)
- Connective tissue disease, including Systemic lupus erythematosus, scleroderma (also referred to as Progressive systemic sclerosis) and Rheumatoid arthritis
In some cases, the disorder can even result in the death of sufferers.
Silicosis Prevention
People who are involved in high-risk occupations should wear dust-masks and stop smoking. They should also use respirators and other protective devices recommended by OSHA. In well-developed nations, individuals engaged in professions that cause them to be exposed to silica dust use special respirators that prevent the entry of dust into their lungs. If possible, individuals who are already affected should make some changes in workplace to reduce or even obliterate exposure to silica dust. If that is not possible, they should wear protective equipment and clothing to prevent further exposure. In extreme cases, a complete change of profession may be required.
Today dry mining has been made infrequent. Special filters have been developed for drilling equipment. Any substance that can lower the amount of silica dust in the air, especially the use of water, is employed to introduce more safety in the working conditions.
Desert Lung Disease
It is a non-occupational type of Silicosis that results from prolonged exposure to sand dust in desert regions. Cases of this disease have been reported from the Libyan desert, Negev and Sahara. The condition occurs as a result of accumulation of sand dust in the lungs. The disorder may be associated to Al Eskan disease, a lung disorder that is supposed to arise due to exposure to sand dust which contains organic antigens. Al Eskan disease was diagnosed for the first time after the Gulf War of 1990.
Silicosis Support Groups
Those suffering from Silicosis and their family members should get in touch with one of the many support groups available for providing guidance, information and assistance regarding the disorder.
Silicosis Pictures
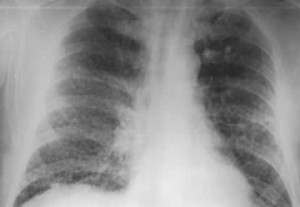
The images underneath would help you understand the appearance of lungs exposed to silica dust.
Picture 1 – Silicosis
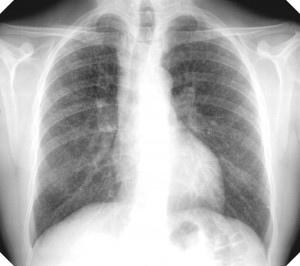
Picture 2 – Silicosis Image
If you have been exposed to Silica dust regularly at work, or already have symptoms of the disorder, contact a health care provider. The earlier you recover from this disorder, the better it is for you.
References:
http://www.nlm.nih.gov/medlineplus/ency/article/000134.htm
http://www.mdguidelines.com/silicosis
http://www.wisegeek.com/what-is-silicosis.htm
http://en.wikipedia.org/wiki/Silicosis