Strabismus is a unique ocular disease that makes sufferers appear cross-eyed and gives rise to vision problems in them. Read and learn all about the condition, including its possible causes, symptoms, diagnosis and treatment options.
What is Strabismus?
Page Contents
- 1 What is Strabismus?
- 2 Strabismus ICD9 Code
- 3 Strabismus Incidence
- 4 Strabismus Types
- 5 Strabismus Causes
- 6 Strabismus Risk Factors
- 7 Strabismus Symptoms
- 8 Strabismus Diagnosis
- 9 Strabismus Differential Diagnosis
- 10 Strabismus Treatment
- 11 Strabismus Complications
- 12 Strabismus Prognosis
- 13 Strabismus Prevention
- 14 Strabismus Pictures
It is an ocular condition characterized by a misalignment of the eyes. It is a visual problem in which the eyes are not properly aligned and point in different directions.
The disorder is known by various other names, such as:
- Squint
- Misalignment of the eyes
Strabismus ICD9 Code
The ICD9 Code for this disorder is 378.
Strabismus Incidence
The condition has been estimated to affect 4% of the U.S population.
Strabismus Types
The disorder can be categorized into a number of types. The most common types of Strabismus include:
Esotropia
Also known as cross-eye or Convergent strabismus, it is a form of the visual disorder in which one or both eyes turn inward in the direction of the nose.
Exotropia
In this form, one or both eyes are pointed in an outward direction. It is also referred to as Wall-eye or Divergent strabismus. It is a common type of Strabismus and develops most often when a child focuses on distant objects. The condition may arise from time to time, specifically when a child is ill, tired or daydreaming.
Parents often notice that their children squint one of the eyes in bright sunlight.
Hypertropia
In this form, there is permanent upward deviation of the visual axis of one of the eyes of sufferers.
Hypotropia
In this type, there is permanent downward deviation of the visual axis of one of the eyes of sufferers.
Strabismus Causes
For both eyes to concentrate on the same object, six different muscles surround each of the eyes and work together to let a person focus. In people affected with Strabismus, these muscles fail to work in unison. Due to this reason, one of the eyes looks at one object and the other one turns in another direction to focus on another object.
When this takes place, two varying images are sent to the brain – one from each eye. This leads to confusion in the brain. In children, the brain may naturally learn to ignore the image sent by the weaker eye. If the Strabismus is left untreated, the eye ignored by the brain in this way may never see properly. This type of loss of vision is referred to as Amblyopia or “Lazy Eye”. In some cases Amblyopia is present first and leads to Strabismus at a later stage.
The cause of Strabismus is unknown in the majority of children affected by the disease. In over half of all cases of the disease, the problem manifests at birth or shortly after a child is born. This is termed as “Congenital Strabismus.”
In the majority of cases, the problem has its cause in muscle control and not muscle strength.
Strabismus and Trauma
The condition can arise from trauma in the following cases:
- Damage to the brain that impairs the control of movement of the eyes
- Damage to the nerves that control the movement of the eyes
- Damage to the eye muscles either in a direct or an indirect way from injury to the eye socket
Strabismus and Associated Disorders
Strabismus can arise due to the presence of many disorders. In adults, the condition may develop as a result of the following diseases:
- Stroke
- Injury to the eye
- Shellfish poisoning
- Guillain-Barre syndrome
- Botulism
- Traumatic brain injury
- Vision loss from any eye disease or injury
- Diabetes (causes a condition known as acquired paralytic strabismus)
Conditions related with in children include the following:
- Cerebral palsy
- Congenital rubella
- Apert syndrome
- Noonan syndrome
- Prader-Willi syndrome
- Incontinentia pigmenti syndrome
- Hemangioma near the eye during infancy
- Trisomy 18
- Traumatic brain injury
- Retinoblastoma
- Retinopathy of prematurity
Strabismus Risk Factors
The disorder is particularly common among children affected with conditions that may affect the brain, such as:
- Prematurity
- Brain tumors
- Hydrocephalus
- Cerebral palsy
- Down syndrome
The disease may have a hereditary association and run in members of the same families. However, many people with the condition have been found to have no relatives with Strabismus. Farsightedness can be a contributory factor, particularly in children. Any other condition that results in loss of vision may also lead to the development of this disorder.
Strabismus Symptoms
The symptoms of this disease may come and go, or be present at all times. The problems usually include:
- Double vision
- Crossed eyes
- Loss of vision or depth perception
- Eyes that do not align in the similar direction
- Uncoordinated eye movements (eyes do not move together)
Children can develop Amblyopia very quickly. Due to this reason, they may not suffer from double vision.
Strabismus Diagnosis
The diagnosis of this disorder involves a detailed physical examination of the eyes of suffering individuals. Follow-up tests might be needed to assess the degree of misalignment of the eyes. Such eye tests may include one or more of the following:
- Visual acuity
- Retinal exam
- Cover/uncover test
- Corneal light reflex
- Standard ophthalmic exam
In some cases, a brain and neurological examination may also be needed for a more accurate diagnosis of the disorder.
During ocular exams, optometrists typically make use of a cover test to diagnose Strabismus. If the eye that is under test is the Strabismic eye, it would fixate on the object after the “normal” eye is covered – provided the vision in the unaffected eye is quite good. Based on the direction of deflection of the Strabismic eye, physicians may determine the direction of deviation.
Strabismus Differential Diagnosis
The symptoms of Strabismus resemble those of another disease known as Pseudostrabismus. The condition usually develops in toddlers and infants who have flat and wide nose bridge and results in an appearance that is similar to that of Strabismus sufferers. With increasing age, the nose bridge become narrower and the folds in the corners of the eyes tend to go away. Physicians should make sure that an individual is not suffering from Pseudostrabismus at the time of diagnosing this disorder.
A Hirschberg test may be used to differentiate between this disease and Strabismus. It is a simple screening exam for Strabismus and involves shining a flashlight on the eye of a patient. When the suffering individual is looking at the light, physicians can see a reflection on the front surface of the patient’s pupil. If the eyes are aligned properly with one another, the reflection will be seen in the same spot of each eye. Due to this reason, the eyes cannot be said to be rightly aligned if the reflection is not observed to be in the same spot in each eye.
Strabismus Treatment
The first step in the treatment of the disease is handing over corrective glasses to affected children, if required. “Lazy eye” or Amblyopia may be addressed first. A patch is likely to be placed over the eye that is in better condition to make the weaker eye function more effectively.
An eye muscle surgery may be required if the eyes fail to move properly even after treatment. Post-operation, various muscles in the eye would be made weaker or stronger. Although operation is an invasive measure, it is considered to be effective and safe. Generally, patients do not need an overnight stay in hospitals.
A surgery for eye muscle repair does not fix the impaired vision of a “Lazy eye.” Following surgery, a child may have to wear corrective glasses. The outcome is usually better if the child is younger at the time the surgery is conducted.
In some cases, children refuse to wear an eye patch despite the efforts of parents. Physicians might use atropine drops in such children. The drops would blur the vision in the straight eye on a temporary basis, and force the misaligned eye to work harder.
Adults affected with mild cases of Strabismus that tends to come and go may have a better condition with eye muscle exercises and glasses that help keep the eyes straightened. If Strabismus arises due to a loss of vision, it needs correction before operation can yield successful outcomes.
Strabismus Complications
The potential complications of this disorder include impaired vision or loss of vision in the eye that is affected. As the condition worsens, patients tend to squint more often. Inability to cope up with the disorder in its initial stages may cause sufferers to develop permanent loss of depth perception apart from a lack of visual ability.
Strabismus Prognosis
The outcome is mixed in case of sufferers of this disorder. Following operation, the visual problems may persist although the eyes may look straight in a single direction. An affected child may continue to have problems in reading at school while adults may find driving more difficult. In athletes and sportsmen, the visual capability may be affected enough to impair their ability to continue their sports activities.
The problem can be generally corrected with early diagnosis and cure. Delay in treatment can result in permanent loss of vision in one eye. Around 1/3rd of all kids affected with this disease tend to develop Ambylopia at a later stage. As the majority of affected children tend to develop Ambylopia or Strabismus again at a later stage, they need to be closely monitored.
Strabismus Prevention
The condition cannot be prevented as its exact causes are not known. However, the possible complications of the condition can be avoided by seeking medical attention on an early basis. If timely treated, the disorder can be checked at its initial stage and ensure better vision for patients.
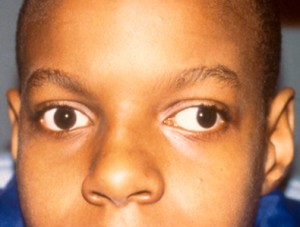
Strabismus Pictures
Get an idea about the physical appearance of individuals affected with this disorder.
Picture 1 – Strabismus
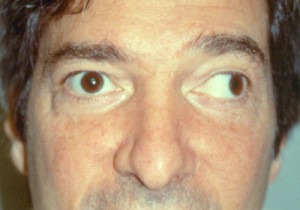
Picture 2 – Strabismus Image
Strabismus patients need early medical evaluation and treatment. If your child has lately been appearing to be cross-eyed, having difficulties in seeing or complaining of double vision, consult a professional healthcare provider on an immediate basis and seek treatment. Difficulties in seeing and reading can adversely affect the educational life and performance of your child. Naturally, it is important to seek medical attention as early as possible.
References:
http://www.nlm.nih.gov/medlineplus/ency/article/001004.htm
http://www.aapos.org/terms/conditions/100
http://kidshealth.org/parent/general/eyes/strabismus.html
http://www.geteyesmart.org/eyesmart/diseases/strabismus-cause.cfm