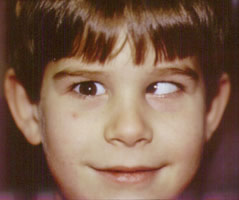
Esotropia Definition
Page Contents
Esotropia is a form of ocular motility disorder that can begin as early as infancy, or even in later adulthood. Individuals with this condition normally have a squint, in which one or both eyes turn inward.
Esotropia Synonyms
This misaligned condition of the eye is also referred to as:
Picture 1 – Esotropia
- Convergent strabismus
- Cross-eye
Esotropia Types
The condition varies according to the age of onset, frequency of occurrence, and the underlying ailments. For simplicity it has been classified into the following types:
Monocular esotropia
The condition can affect only one eye and is subdivided as follows:
Right esotropia
In this type, the right eye normally squints.
Left esotropia
In some patients, the left eye may turn inward.
Alternating esotropia
The disorder is marked by alternate fixation between the right and left eye. Here, at one moment the right eye is straight and the left one turns inward, and at the next the left eye is straight and the right squints. However, patients will never squint with both eyes simultaneously. Medical experts often use the term “bilateral esotropia” to denote this form.
Acquired esotropia
The condition can develop after infancy and typically occurs in patients aged 2-5 years.
Concomitant esotropia
The size of deviation is independent of the line of sight. Majority of cases are concomitant and normally occurs in older children. This particular form can be sub-classified into the following tyes:
Constant esotropia
The affected eye always turns inwards when attempting to focus at all distances.
Intermittent esotropia
In this type, the eye squints occasionally and is more pronounced when viewing close objects. Such short-sighted patients do not squint when looking at distant objects and are known to have near esotropia. The inward movement of the eye may sometimes occur when looking at far objects but not at near ones. In such cases, the condition is called distance esotropia. On the other hand, in cyclic esotropia the convergent deviation of the eyes occurs in repeated cycles.
Primary esotropia
The abnormal condition of the eye could be present as an elementary problem in many individuals. Infantile/congenital esotropia is a sub-type of the disorder that occurs during the first 6 months of life in an otherwise healthy child.
Secondary esotropia
The crossed eyed appearance could be an outcome of an underlying ophthalmologic disorder.
Consecutive esotropia
Many individuals are affected with exotropia, a condition, in which one or both eyes turn outward. However, an overcorrection of the eye defect could often result in inward ocular deviation.
Incomitant esotropia
Unlike the previous form, here the size of inward deviation varies with the direction of gaze. It commonly occurs in children and adults.
Accommodative esotropia
Patients who are having difficulty focusing on near objects could develop the accommodative type of the disorder. The correction of the affected eye/eyes can however, be done using far-sighted glasses. This form could be classically divided into the following categories:
- Refractive accommodative esotropia
- Nonrefractive accommodative esotropia
- Partially accommodative esotropia
- Convergence excess esotropia
Non-accommodative esotropia
This type of eye crossing is not responsive to glasses as opposed to the accommodative form.
A-pattern esotropia
In this type, there is more convergence in midline up gaze than down gaze.
V-pattern esotropia
The inward turning of the eye is more prominent in down gaze.
Esotropia Symptoms
Patients with misaligned eyes normally exhibit symptoms like:
- Headache
- Eye strain
- Pain in the eye
- Double vision
- Reduction in vision
- Loss of depth perception
- Suppression of image from one eye
- Slight head tilt
Esotropia Causes
The condition is a form of strabismus, in which the eyes are improperly aligned with each other. This could be attributed to the lack of coordination between the muscles of the orbit, which are a group of seven muscles that control the movement of the eye. Four of the muscles regulate the movement of eye in the upward, downward, left and right direction under normal circumstances. The other two extraocular muscles control the adjustments involved in counteracting head movement. In someone with convergent strabismus, these muscles fail to function and prevent one or both eyes to focus on the same point in space. The binocular vision, in which both eyes are used together, can get affected, causing problems in depth perception- the eye’s ability to focus on an object and calculate its distance.
The Incomitant form of the disorder has been associated with neurological, mechanical or muscular conditions of the eye such as abducens nerve palsy or Duane’s syndrome. Visual loss or impairment of vision results in the secondary concomitant condition. As mentioned earlier, individuals with long-sightedness/hyperopia are more vulnerable to develop the accommodative disorder. This happens when a hyperopic patient in an attempt to focus or accommodate the eyes ends up converging them. The congenital defect is more often linked to ocular disorders like:
- Manifest Latent Nystagmus
- Defective abduction
- Dissociated Vertical Deviation
Esotropia Diagnosis
A detailed examination of the eyes could point to convergent strabismus. However, the degree of alignment of the eye has to be evaluated by using some of the following diagnostic tests and exams:
Picture 2 – Esotropia Image
Retinal exam
The retina is the light-sensitive membrane lining the inner eyeball. Indirect opthalmoscopy can be used to observe the vitreous, retina and other internal structures of the eye. Any underlying disorder or injury of the retina can help explain the cause of visual loss.
Corneal light reflex
The external screening test is performed by shining a pen light in the eye of a patient in order to determine whether it gets reflected in a similar way. Based on where the light falls on the cornea, an examiner can find out the exact type of ocular misalignment.
Visual acuity test
This is an exclusive method of assessing the acuteness of vision, which is dependent on the sharpness of the retina. The test requires the patient to identify characters in the form of letters and numbers on a standardized chart from a set distance. Visual acuity is normally expressed as a fraction. Individuals with normal eyesight have a visual acuity of 20/20. However, deviation from the reference standard is an early warning sign of an underlying ocular problem.
Cover/uncover test
A cover is placed over an eye for a short duration of time and then removed while observing both eyes for movement. The affected eye will probably turn inward.
Esotropia Treatment
In most cases, physicians recommend patients to wear glasses for correcting the eye. Occlusion or patching therapy yields favorable results in patients with monocular visual dysfunction. An eye patch is placed on the normal eye for compelling the other one to function properly. Problems with binocular vision can be treated with the aid of orthoptic exercises. The aim is to strengthen the eye muscles to correct the binocular deficiency. Exercises like barrel cards, brock string and pencil pushup can help restore the normal functioning of the eyes. Eye care professionals can use a lens with prism correction to treat muscular imbalance that causes errors in visual orientation. The method is highly beneficial to patients with double vision. Botulinum toxin can be given to adult patients for providing permanent symptomatic relief. When none of the non-operative methods work, an extra-ocular surgery would be needed to correct the condition. The underlying eye disorders that cause a squint should be seriously looked into.
Esotropia Prognosis
Unnecessary delay in treatment can lead to permanent vision loss. Non-invasive methods of eye correction have shown good results. Post operative care is a must as many patients complain of having vision problems.
While eye exercises can help patients suffering with Esotropia, glasses can also be equally effective in alleviating the symptoms. The disorder needs prompt medical evaluation; so an early appointment with a healthcare provider is extremely important for patients with suspected squint.
References:
http://en.wikipedia.org/wiki/Esotropia
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001999/
http://www.aapos.org/terms/conditions/48
http://emedicine.medscape.com/article/1198784-overview