Familial Mediterranean fever is an auto-inflammatory condition with a cyclic pattern of symptoms. Read and learn all about the causes, symptoms, diagnosis and treatment of this ailment.
Familial Mediterranean fever Definition
Page Contents
- 1 Familial Mediterranean fever Definition
- 2 Familial Mediterranean fever History
- 3 Familial Mediterranean fever Synonyms
- 4 Familial Mediterranean fever Incidence
- 5 Familial Mediterranean fever Symptoms
- 6 Familial Mediterranean fever Causes
- 7 Familial Mediterranean fever Pathophysiology
- 8 Familial Mediterranean fever Diagnosis
- 9 Familial Mediterranean fever Treatment
- 10 Familial Mediterranean fever Complications
It is an inherited disorder having prominent features such as recurrent episodes of fever and severe abdominal pain. The condition is usually abbreviated as FMF.
Familial Mediterranean fever History
In 1945, the abdominal attacks of FMF were first described by a New York allergist named Dr Sheppard Siegal. The disorder was then medically termed as “Benign paroxysmal peritonitis”. The severity of the disorder was understood by Dr Hobart Reimann, working in the American University in Beirut. The discovery of colchicine as a treatment tool for the attacks was made in 1972. In 1997, the genetic cause of the disorder was illustrated by the following two groups:
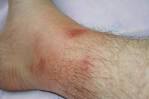
Picture 1 – Familial Mediterranean fever
- The French FMF Consortium
- The International FMF Consortium
Familial Mediterranean fever Synonyms
The disorder is known by various other names, the common ones of which include:
- Recurrent polyserositis
- Familial paroxysmal polyserositis
- Periodic peritonitis
- Benign paroxysmal peritonitis
- Periodic disease
- Periodic fever
- Reimann periodic disease
- Reimann’s syndrome
- Siegal-Cattan-Mamou disease
- Wolff periodic disease
Familial Mediterranean fever Incidence
As the name suggests, FMF is mainly found in families of Mediterranean ancestry. These include the Armenians, Sephardic Jews, Cypriots, Turks and Arabs.
Familial Mediterranean fever Symptoms
The signs and symptoms of FMF usually occur in the form of a series of attacks that may last for 48-96 hours, and attain peak intensity within the first 12 hours. Majority of the patients are subjected to the first attacks before the age of 18. Such patients seem healthy between the attacks with no signs of the disease. Apart from intense fever and abdominal discomfort, the affected individuals usually have bouts of the following:
- Inflammation of the abdominal lining
- Abdominal tenderness
- Constipation followed by diarrhea
- Arthritis
- Swelling of pleural cavity of the lungs
- Chest pain
- Skin rashes
- Pericarditis
- Pelvic inflammatory disease in females
- Bacterial infection of the skin
- Muscle ache
- Inflammation of the tunica vaginalis, covering the testis
Familial Mediterranean fever Causes
Mutation in the MEFV gene on chromosome 16 has been linked to the disorder. FMF is an autosomal recessive trait that affects individuals who have received the mutant gene from both of their carrier parents. Generally, in this type of inheritance if both parents are carriers, there is a 25% chance of a child inheriting both abnormal genes and, consequently, developing the disorder. There could even be a 50% chance of a child acquiring only one defective gene, and of being a carrier like the parents as well as a 25 % chance of receiving both normal genes. If one parent is a carrier and the other being affected with FMF, then there could be a 50% chance of the child to possess the defective gene. On the other hand, if both parents are suffering from FMF then the child has a 100% chance of getting affected. As suggested by a few reports, the disorder could occur in an individual with only one carrier parent.
Familial Mediterranean fever Pathophysiology
The MEFV gene is specifically located on the short arm of chromosome 16 (16p13) and codes for a protein called pyrin or marenostrin. FMF is a consequence of several mutations in the gene. The various types of genetic transformations determine the severity of the condition. Mutations occur chiefly in exons 2, 3, 5 and 10. The precise role of pyrin has not been properly established by genetic researchers. However, it is presumed that the protein suppresses the activation of caspase 1 – the enzyme that stimulates production of interleukin 1β, a cytokine acting as an important mediator of various immune reactions. Simply put, an impaired pyrin becomes incapable of controlling inflammation and evokes autoinflammatory responses in various body tissues. Medical experts have not been able to find out the causative factors responsible for triggering the attacks. The production of specific symptoms as a repercussion of excessive release of IL-1 is yet to be ascertained.
Familial Mediterranean fever Diagnosis
Health specialists must be highly suspicious for FMF when dealing with individuals having cyclic episodes of fever, abdominal problems and joint pain. Conducting the following tests may aid in the correct diagnosis of the underlying illness:
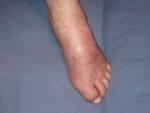
Picture 2 – Familial Mediterranean fever Image
Blood test
Elevated levels of C-reactive protein, an acute-phase protein, which is an essential hallmark of inflammation, suggest FMF. In addition to this, an increased white blood cell count signifies an inflammatory reaction in the body. Erythrocyte sedimentation rate is another component of the hematology test that detects inflammation by simply measuring the rate at which red blood cells settle in a test tube. In patients with FMF, the sedimentation rate increases with more inflammation.
Molecular testing
The exons 2, 3, 5, and 10 of the MEFV gene can be sequenced to detect the anomaly.
Joint aspiration
Arthritis causes the lining tissues of the joint to become inflamed and produce excessive amount of synovial fluid. In this procedure, a sterile needle and syringe are used to drain fluid from the joint. Analysis of the fluid in the laboratory can help to exclude the other causes of arthritis, such as infection and gout.
Chest radiography
A chest X-ray taken in the upright position and while lying on the side is an accurate tool in discovering small amounts of fluid in the pleural space. The quantity of the fluid can be estimated to determine the intensity of the chest attacks.
Imaging studies
Use of a CT or MRI scan may reveal abdominal inflammation, swollen pleural cavity and pericarditis.
Electrocardiogram
The associated abnormalities of pericarditis can disrupt the normal electrical activity of the heart. The test may help in evaluating the deficits in the cardiac system.
Metaraminol Provocative Test
This is a highly sensitive procedure that can positively indicate the existence of FMF. Here, a single 10 mg infusion of Metaraminol (a potent medicine used to treat hypotension) is administered to affected people in order to trigger an inflammatory response. Individuals who have mild to severe FMF experience the symptoms within 48 hours after the intake of the drug.
Familial Mediterranean fever Treatment
The number of attacks can be greatly reduced with colchicine, a medication known for treating gout. Although the drug includes side effects like gastrointestinal conditions and netropenia, the drastic improvement normally observed in the FMF-affected patients makes it reliable. The prescribed dose of this medicine is normally 1-2 mg that must be taken on a daily basis. In some patients, the drug is administered at the onset of an attack. Colchicine in adjunct with anakinra can enhance the treatment of FMF. Etanercept can help in the alleviation of joint pain. The use of interferon alfa as an alternative to colchicines is beneficial to many patients. Analgesics can reduce the intensity of body pain. Non-steroidal anti-inflammatory drugs can treat the frequent bouts of joint pain. Prednisolone can effectively soothe muscle pain.
Familial Mediterranean fever Complications
The most feared complication of FMF is amyloidosis in which a particular protein, called amyloidin, gets deposited in various body tissues without any evident attacks. The condition is more debilitating when the protein begins to accumulate in the kidney, heart, spleen, thyroid and gastrointestinal tract. Hypertension and renal vein thrombosis may accompany the condition. Recurrent joint attacks may manifest into chronic arthritis causing joint destruction. In FMF-affected females, risks of infertility and miscarriages are high. The condition also puts patients at a high risk of developing Henoch-Schönlein purpura and Spondylarthropathy.
With the advent of colchicine therapy, the periodic symptoms of Familial mediterranean fever has been reduced to a great extent. Early detection of the condition, followed by a long-term treatment, can help patients from developing the near-fatal complications.
References:
http://en.wikipedia.org/wiki/Familial_Mediterranean_fever
http://www.mayoclinic.com/health/familial-mediterranean-fever/DS00766
http://www.genome.gov/12510679
http://emedicine.medscape.com/article/330284-overview

Woow its a relief to hear that its cause isnt known cz i would either blam it on my health provider or husband but it gives me hope that he will one day be fine.