Fibrodysplasia Ossificans Progressiva, or FOP, is a rare condition that is extremely painful and restrictive. Read on to know what Fibrodysplasia Ossificans Progressiva is as well as its causes, symptoms, diagnosis and treatment.
Fibrodysplasia Ossificans Progressiva Definition
Page Contents
- 1 Fibrodysplasia Ossificans Progressiva Definition
- 2 Fibrodysplasia Ossificans Progressiva History
- 3 Fibrodysplasia Ossificans Progressiva Symptoms
- 4 Fibrodysplasia Ossificans Progressiva Causes
- 5 Fibrodysplasia Ossificans Progressiva Diagnosis
- 6 Fibrodysplasia Ossificans Progressiva Differential Diagnosis
- 7 Fibrodysplasia Ossificans Progressiva Treatment
- 8 Fibrodysplasia Ossificans Progressiva Prognosis
- 9 Fibrodysplasia Ossificans Progressiva Life Expectancy
- 10 Fibrodysplasia Ossificans Progressiva Pictures
- 11 International Fibrodysplasia Ossificans Progressiva Association
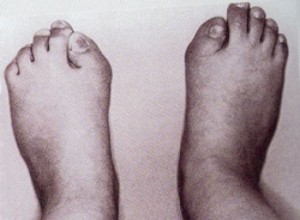
Picture 1 – Fibrodysplasia Ossificans Progressiva
This is a rare genetic disease that affects the connective tissues of the human body. It affects only one out of 2 million individuals across the world.
The disorder is known by many other names, such as:
- Activin A receptor
- Activin receptor type I protein
- ACVR1 gene
- Skin sores
- Type I gene
- Valgus deviation
- ACVR1 protein
- Bone morphogenetic protein (BMP)
- Myositis
- Ossification
- Pressure sores
- Fibrous nodules
- Heterotopic ossification
- Isotretinoin
The condition is also known as Stone Man Syndrome. The peculiar name is attributed to the fact that the progressive symptoms of the disease harden the body tissues like stone and leads to complete paralysis.
Fibrodysplasia Ossificans Progressiva History
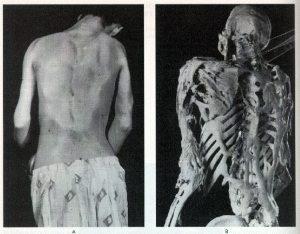
The condition was first documented in 1692 by a French physician known as Guy Patin. The disease was more famously recognized in the case of Harry Eastlack. The syndrome was diagnosed in Eastlack at the age of ten. It immobilized the entire body of the individual excluding his lips.
Fibrodysplasia Ossificans Progressiva Symptoms
The initial symptoms of Fibrodysplasia Ossificans Progressiva generally arise in childhood. The disease makes a progression all through the life of a sufferer.
Children who are born with this disease seem to be normal from all aspects. In most cases, the only defect is an abnormality of the big toes. The toes appear to be shorter than usual and consist of a bony lump close to their base. This congenital abnormality of the toe is regarded as a defining feature of the condition that helps in its diagnosis.
The progressive symptoms usually begin to arise as the child nears his or her adolescent years. Initially, painful inflammation of the soft tissues is the only symptom. These are aggravated by viral disorders or injuries. Over time, inflammations increase in number. The existent swellings turn harder due to slow transformation of the soft tissues into bone. The joints become stiffer and mobility becomes painful and difficult. Gradually, individuals with this syndrome begin losing mobility with the progression of the disease. Most sufferers require a wheelchair or other support to move about by the time they enter their thirties.
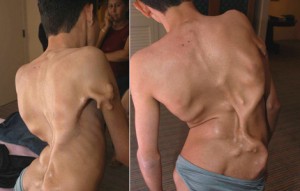
The loss of mobility usually starts with the neck and shoulder region of the body and progresses downwards. Body regions commonly impacted by this condition involve
- Jaw
- Neck
- Shoulders
- Chest
- Elbows
- Wrists
- Spine
- Hips
- Knees
- Ankles
Even though a person is born with this condition, formation of extra bone may not occur during birth. An individual may pass several months or years without suffering from a sudden occurrence, which may indicate the growth of new bone.
Fibrodysplasia Ossificans Progressiva Causes
A genetic mutation is the inherent cause of Fibrodysplasia Ossificans Progressiva. The mutation occurs in the gene ACVR1 (= ALK2) that codes for a protein called Activin Receptor Type-1. This mutation alters the shape of the receptor by substituting the amino acid Arginine with the amino acid Histidine. It results in the malfunction of the receptor. This leads to the transformation of the endothelial cells into mesenchymal stem cells and ultimately into bone.
Due to this defect, an injury to soft tissue results in the deposition of bones during the bodily repair process. Because of this reason, injuries can not only lead to the formation of new inflammation but also worsen swellings that already exist.
The condition an also arise due to a viral illness. Viral disorders play a role in the growth of unusual bone tissue by stimulating inflammatory reactions from the immune system. Tissue damage can occur due to such inflammatory reactions.
Fibrodysplasia Ossificans Progressiva Diagnosis
In most cases, a proper diagnosis of Fibrodysplasia Ossificans Progressiva (FOP) is possible on the basis of the big toe malformation (a characteristic of this condition) in patients as well as the physical observation of the rapidly altering inflammation on the neck, head or back of sufferers.
There is a high lack of awareness of FOP among doctors. This explains why the disease is misdiagnosed in an estimated at 80 percent cases or more. The errors in FOP diagnosis have resulted in suffering and pain for patients as well as their families across the world. Misdiagnosis leads to unnecessary invasive methods, such as biopsies. There have also been permanent complications arising from medical interventions, which include loss of movement.
Fibrodysplasia Ossificans Progressiva Differential Diagnosis
FOP is frequently misdiagnosed as
- Cancer
- Aggressive juvenile fibromatosis (also known as Desmoid tumors)
- Progressive osseous heteroplasia (a rare ailment characterized by unusual growth of bone)
Differential diagnosis for FOP should aim at differentiating the disease from the abovementioned conditions.
Fibrodysplasia Ossificans Progressiva Treatment
Unfortunately, there is still an absence of an effective treatment for Fibrodysplasia Ossificans Progressiva. Surgical removal of excess bones is not considered as an option. This is due to the fact that surgery is often found to result in greater bone formation. Bones thus formed fail to go away on their own.
Medications used for FOP treatment usually aim at providing relief from its symptoms, such as inflammation and pain. A short course of high-dose corticosteroids, if commenced within a day of a flare-up episode of symptoms, might help in reducing inflammation and acute tissue edema that FOP sufferers experience during the initial stages of the condition. However, corticosteroid usage should be limited to the very early stages of cure of symptoms rapidly flaring up in the major joints, submandibular area or jaw. Corticosteroids should not be used in curing flare-ups that involve regions such as the trunk, back or neck of a person. This is mainly due to the recurring nature and long duration of the flare-ups along with the problems in assessing the real cause of their onset.
Fibrodysplasia Ossificans Progressiva Prognosis
FOP is a progressive disorder and typically tends to worsen with time and advancing age of a patient. However, the rate of formation of new bone varies from person to person. The progression of this disorder is usually unpredictable.
Fibrodysplasia Ossificans Progressiva Life Expectancy
Generally, the life expectancy is poor for individuals affected with FOP. This is mainly due to the fact that there is an absence of effective cure for the disorder. FOP eventually results in complete paralysis of the body and has fatal consequences. Most people suffering from FOP die before they are 40 years old.
Fibrodysplasia Ossificans Progressiva Pictures
Here are some useful Fibrodysplasia Ossificans Progressiva photos that will provide you with a visual idea about the disease. Take a look at these Fibrodysplasia Ossificans Progressiva images to know about the physical symptoms arising due to this condition.
Picture 2 – Fibrodysplasia Ossificans Progressiva Picture
Picture 3 – Fibrodysplasia Ossificans Progressiva Image
International Fibrodysplasia Ossificans Progressiva Association
Also known as IFOPA, this is a non-profit organization that provides support to education, communication and medical research for individuals affected by FOP. The establishment is based in Florida, USA and raises funds for supporting research on FOP. It was founded in 1988 by Jeannie L. Peeper, a FOP patient herself.
Presently, medical researchers are busy researching FOP and new ways of curing the condition. A medicine is being developed to control the growth of the bone.
References:
http://www.ucsfbenioffchildrens.org/conditions/fibrodysplasia_ossificans_progressiva/
http://www.wellness.com/reference/conditions/fibrodysplasia-ossificans-progressiva-fop/
http://www.disabled-world.com/disability/types/fop.php