Postpartum thyroiditis (PPT) is a condition observed after childbirth and is manifested by mood swings and intense palpitation after delivery. If you or a family member has lately been suffering from such symptoms, read and know all about the causes, symptoms, diagnosis and treatment of this condition.
Postpartum thyroiditis Definition
Page Contents
It is a temporary inflammation of the thyroid gland that develops in many women post pregnancy. The term “postpartum” refers to the period after delivery. The condition is usually painless and belongs to a group of thyroiditis known as Resolving Thyroiditis. It may involve either Hyperthyroidism or Hypothyroidism or both, consecutively. Hypothyroid symptoms extending beyond one year after delivery is generally not regarded as Postpartum thyroiditis.
This is a common disorder that affects many new mothers.
Postpartum thyroiditis Phases
It usually occurs in two phases that are generally transient.
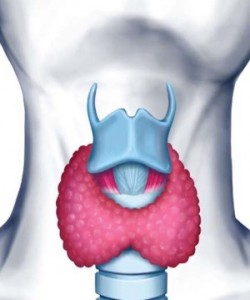
Picture 1 – Postpartum thyroiditis
Hyperthyroid Phase
The initial phase of this disorder is characterized by hyperthyroidism, a condition marked by excessive production of thyroid hormones due to overactive thyroid glands. During this phase, symptoms generally appear two to six months post-delivery. Hormonal disturbances are normally very subtle and may often remain undetected. The thyroid gland loses control over the release of thyroid hormone that it normally stores, causing elevated levels of the hormone in the blood.
Hypothyroid Phase
Hypothyroidism may occur in the second phase where the thyroid gland does not produce sufficient amount of thyroid hormone. This phase is also temporary and can occur within three to twelve months after delivery. During hyperthyroid phase, sufficient damage to the thyroid gland may cause decreased production of thyroid hormone, resulting in this condition. In most cases, however, patients do not go through the initial phase and directly develop Hypothyroidism.
Postpartum thyroiditis Incidence
It affects about 5% of all women within a year after delivery. One in five women with this disorder develops permanent hypothyroidism that may require life-long treatment.
Postpartum thyroiditis Symptoms
This condition usually occurs within the first year after delivery. Symptoms are generally very mild and may vary from one patient to another. The two phases of this disorder are manifested by different sets of symptoms.
Hyperthyroid Phase
Some of the main signs and symptoms in this phase involve:
Nervousness
Patients may undergo extreme anxiety and easiness. They often experience an unpleasant feeling of fear and concern.
Goiter
In this condition, the thyroid suffers enlargement, which leads to an acute swelling of the neck or larynx.
Palpitation
In some patients, irregular or rapid beating of the heart may occur without any specific cause.
Heat intolerance
Sufferers show hypersensitivity to heat. Even a slight rise in temperature becomes unbearable for them. It is often accompanied by profuse sweating.
Fatigue
Some patients get physically exhausted very easily. They may even feel lethargic to perform routine activities.
Irritability
Mood swings and fussiness are other common symptoms of postpartum women.
Weight loss
New mothers may have a decreased appetite that causes extreme reduction in body weight.
Trembling hands
During this phase, the hands shake uncontrollably. This may even affect other parts of the body.
Muscular weakness
One or more muscles of the body may lose strength. Spasms may also develop in these regions.
Hypothyroid Phase
The main difficulties experienced in this phase are:
Inability to concentrate
Patients may lose focus and have difficulty in concentrating.
Carelessness
Affected individuals may develop lack of concern and casual approach. They can become quite negligent and behave in an improper manner.
Dry skin
Scaly and dry skin on the lower legs, arms, abdominal regions and thighs is a typical symptom of the hyperthyroid phase.
Cold intolerance
In the later phase, patients undergo abnormal sensitivity towards cold conditions or temperatures.
Muscle aches
This condition is quite common and may involve a single muscle or a group of muscles in the body.
Poor memory
Frequent episodes of momentary memory lapse may occur.
Postpartum thyroiditis Causes
Medical experts are yet in the dark regarding the cause of sudden inflammation of the thyroid gland occurring in some women after delivery. Nonetheless, there are some factors that are suspected to cause this condition.
Autoimmunity
It case of an autoimmune disorder, the immune system of the body turns against its own cells and tissues mistaking them as pathogen. It starts producing autoantibodies as a response. During pregnancy, the immune system gets suppressed to prevent the formation of antibodies against the fetus. This protects the fetus from getting rejected by the body, thus preventing a miscarriage. Post delivery, the immune system gets activated once again and produces antibodies like thyroglobulin (TgAb) that may attack the thyroid gland. This can cause Postpartum thyroiditis. Increased production of autoantibodies against thyroid peroxidase denoted as “TPOAb” causes cellular damage and alters the function of the thyroid gland.
Changes in T-cells
T-cells belong to a group of white blood cells (WBCs), known as lymphocytes, which play a major role in the immune system and guard the body against infection. There are a number of different types of T-cells like helper cells, cytotoxic cells that identify and destroy infectious agents. In this condition, however, the number of T- helper cells (such as CD4) increases in comparison to CD8 and directly attacks the thyroid gland.
Hashimoto’s thyroiditis
In this autoimmune condition, the thyroid gland is attacked by a variety of cell and antibody-mediated immune processes. Lymphocyte (T-cells) infiltration and follicle formation within the thyroid gland occurs, causing both Hypothyroidism and Hyperthyroidism.
Graves’ disease
In this disorder, an abnormal response of the immune system causes the thyroid gland to produce excessive amount of thyroid hormones. Thyroid autoantibodies are believed to stimulate thyroid hormone secretion while thyroid growth causes Hyperthyroidism and Goiter.
Type 1 diabetes
In this form of diabetes, autoimmune destruction of insulin-producing beta cells of the pancreas leads to elevation of glucose in the blood and urine of the patients. This may cause a greater risk for thyroid dysfunction in post partum women.
Postpartum thyroiditis Diagnosis
This condition usually remains undetected by physicians, owing to the subtleness of the symptoms of this disorder. In most cases, the level of thyroid hormone is checked to determine this condition. Some other diagnostic tests for the disorder include:
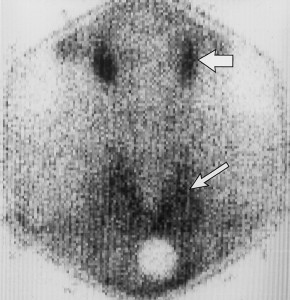
Picture 2 – Postpartum thyroiditis Image
Blood test
Thyroid stimulating hormone (TSH) and thyroid hormone thyroxine (T4) levels in the blood are normally measured by a routine blood test. Thyroxine (T4) is the key hormone produced in the thyroid gland. Higher levels of T4 level suppress the levels of TSH in blood, causing Hyperthyroidism. On the other hand, lower levels of T4 and higher levels of TSH in the blood normally indicate Hypothyroidism.
Thyroid scan
This diagnostic technique is used for the evaluation of Hyperthyroidism. Radioactive dye is orally administered to patients in the form of capsule or fluid. Thyroid gland absorbs the dye, which is later scanned by placing a scintillator counter over the neck. Images obtained after the completion of scan show those regions of the thyroid gland that have absorbed the dye. The absorption is generally very less and uneven.
Postpartum thyroiditis Treatment
Treatment depends on the phase of the condition that one is suffering from and the degree of symptoms that the patients exhibit.
Beta blockers
These are usually administered to the patients during Hyperthyroid phase to block the effects of thyroid hormones on the body, such as palpitations and tremors.
Thyroid hormone replacement
These are synthetic medicines that are given to the patients during Hypothyroid phase. Levothyroxine is a commonly used synthetic thyroid hormone that can restore the normal thyroid hormone levels in the body. It is generally prescribed to the patients for approximately six months, following which it should be discontinued for almost four to six weeks. In case patients develop permanent hypothyroidism after Postpartum thyroiditis, Levothyroxine must be taken on a daily basis.
Natural thyroid hormones, such as desiccated (dried and powdered) animal thyroid (Armour) that is obtained from pigs, can also be used for thyroid therapy. These are generally administered to the patients in form of supplements.
Radioactive iodine therapy
Iodine is an essential mineral for the human body. It is used by the thyroid gland to function properly. In this method, a radioactive form of iodine is used to destroy some of the gland cells. This is usually performed to reduce the production of thyroid hormone by the thyroid gland. However, this technique is generally not recommended for breast feeding mothers.
Postpartum thyroiditis is a common disorder with mild, temporary symptoms. 80% of the patients regain normal thyroid function without any therapy. It is not a life-threatening disorder and effective treatments are now available to relieve discomfort. Early detection must be done in order to shorten the extent of suffering in patients.
References:
http://en.wikipedia.org/wiki/Postpartum_thyroiditis#Diagnosis
http://www.mayoclinic.com/health/postpartum-thyroiditis/AN00153
http://www.thyroid.org.au/ThySoc/ThySocPPTD.html
http://www.drugs.com/cg/postpartum-thyroiditis.html