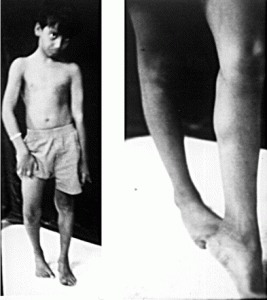
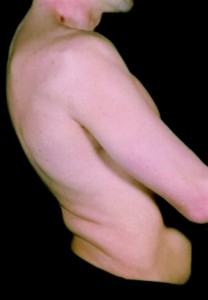
What is Stiff-Person Syndrome
Page Contents
- 1 What is Stiff-Person Syndrome
- 2 Stiff Person Syndrome Signs and Symptoms
- 3 What Causes Stiff‑Person Syndrome
- 4 Risk Factors
- 5 Complications
- 6 Diagnosis and Tests
- 7 Treatment and Management of Stiff‑Person Syndrome
- 8 Prognosis and Life Expectancy
- 9 Incidence and Prevalence
- 10 ICD-9-CM Codes and ICD-10-CM Codes
Stiff-Person syndrome (SPS), is a rare progressive autoimmune disease of the nervous system, characterized by stiffness and painful episodic spasms in the muscles of the body, especially the spine.
Coined first by doctors Frederick P. Moersch and Henry W. Woltman in 1956, it was originally known as “stiff man syndrome”, but the name underwent a change on the premise that individuals of both gender and all ages are affected by it.
It can be classified into the following types, depending on its symptoms, and severity:
- Focal stiff person syndrome
- Progressive encephalomyelitis with rigidity and myoclonus
- Jerking stiff person syndrome
- Stiff limb syndrome
Stiff Person Syndrome Signs and Symptoms
Beginning between ages 30 and 50, symptoms may either take years to develop or emerge within weeks.
Early Symptoms
- Stiffness is the earliest symptom, felt in lower back, neck, and leg muscles.
- With the progression of the disorder, severe and painful spasms may develop that may stay for few minutes to hours, and may impact a particular region or the entire body, commonly occurring in the abdominal muscles (causing the person to feel fuller), respiratory and chest muscles
The triggering factors of spasms involve, stress, cold weather, infections and sudden noise or touch.
Other symptoms
- Sleep disturbance
- Shortness of breath
- Anxiety
- Tremors
- Unintended weight loss
What Causes Stiff‑Person Syndrome
The exact cause of this disorder is not known, and among the varied theories that are proposed, one points out that it may result from an abnormal autoimmune reaction in the brain and spinal cord. GABAergic neurons control muscle movements using gamma-aminobutyric acid (GABA) as a neurotransmitter, and are produced by an enzyme, GAD (glutamic acid decarboxylase). According to several studies, in approximately 60% of people with SPS, these enzymes are blocked by antibodies, thereby lowering the levels of GABA in the CNS, ultimately causing a loss of neural inhibition.
Risk Factors
It is more likely to affect women than men. Some of the risk factors associated with certain underlying medical conditions include:
- Diabetes
- Vitiligo
- Thyroiditis
- Pernicious anemia
- Epilepsy
- Breast cancer
- Cerebellar ataxia
- Gluten sensitivity
Complications
- Walking disability involving a rigid gait
- A hunched posture
- Depression
- Skeletal fractures and muscle ruptures
Diagnosis and Tests
The diagnosis generally involves:
- Physical examination
- Antibody testing to detect the presence of high levels of GAD antibodies
- Electromyography (EMG) to record electrical activities occurring in skeletal muscles
- Lumbar puncture test to confirm the disorder
Additional laboratory tests to support the diagnosis and detect certain underlying conditions may involve:
- Hemoglobin AIC test for detecting diabetes mellitus
- Complete blood count for identifying pernicious anemia
- Test for thyroid-stimulating hormone for detecting thyroiditis
Differential Diagnosis
- Fibromyalgia
- Hyperexplexia
- Multiple sclerosis
- Dystonia
- Transverse myelitis
- Occult vascular malformations
- Neuromyotonia (Isaac’s syndrome)
- Schwartz-Jampel syndrome
- Muscular dystrophies
- Metabolic myopathies
- Lyme disease
Treatment and Management of Stiff‑Person Syndrome
Treatment, mainly directed at lowering the pain and managing the symptoms involves:
Medication
- Administration of benzodiazepines along with baclofen to reduce muscle stiffness and spasms.
- Corticosteroids such as gabapentin and tiagabine to reduce seizures; however, prolonged usage may induce various side effects such as headache and dizziness.
Immune-Modulating Therapies
Intravenous Injection of Immune Globulin
Giving immune globulin intravenously may help in reducing the stiffness and sensitivity to noise, stress and touch.
In this procedure, unwanted substances such as toxins, and polluted plasma parts are removed from blood plasma and then the treated plasma is returned to the body. However, more research needs to be done in this area.
Autologous Hematopoietic Stem Cell Transplantation or Auto-HSCT
This method, usually executed in case medicines are all ineffective, involves infusion of bone marrow stem cells that are collected from peripheral cord blood, bone marrow or umbilical cord blood so that hematopoietic functions are revived.
Physical Therapy
An affected individual is also made to undergo physical therapy, comprising of stretching, relaxation exercises and massages so as to overcome problems of voluntary movement and fine motor skills.
Prognosis and Life Expectancy
Living with SPS can be tough since treatment cannot cure the condition completely. Owing to the destruction of his normal defensive reflexes, a person suffering from SPS becomes susceptible to injuries and even death may occur due to a sudden fall. Life expectancy thus depends on how severe one’s condition is and several means are undertaken to ensure that symptoms remain within control.
The condition, rarely occurring in pregnancy can be adequately managed with proper treatment, but babies with SPS, generally do not survive beyond a few months.
Incidence and Prevalence
Though the exact incidence of the condition is not known, it is estimated that 1 in 1,000,000 people may have SPS.
ICD-9-CM Codes and ICD-10-CM Codes
The ICD-9-CM code of SPS is 333.91, and the ICD-10-CM code is G25.8.