Truncus arteriosus (TA) is a rare condition of the fetal heart that usually occurs during the first 8 weeks of pregnancy. Read and know all about the types, symptoms, causes, treatment and prognosis of this cardiac abnormality.
Truncus arteriosus Definition
Page Contents
It is a congenital defect of the heart in which a single blood capillary, known as the Truncus arteriosus, becomes incapable of undergoing division into the pulmonary artery and aorta. This blood vessel is the first section of the embryonic arterial vascular system that initially opens from both the ventricles of the heart before going through segmentation. The major function of the aorta is to carry oxygenated blood to different parts of the body. On the other hand, the pulmonary artery transports deoxygenated blood to the lungs for oxygenation. In this condition, however, infants have only a single blood vessel or truncus that enters the lungs directly. This causes severe cardiac failure.
Truncus arteriosus other names
The condition is known by various names like:
- Persistent truncus arteriosus
- Common arterial trunk
Truncus arteriosus Embryology
Bulbus cordis is a transitory dilation in the embryonic heart formed at the conjunction of arterial trunk and aortic arches. Both truncus arteriosus and bulbus cordis are divided by the aorticopulmonary septum, a membrane wall. Subendocardial tissue is a loose connective tissue that connects the endocardium (innermost layer) and myocardium (middle layer) of the heart. During the fifth week of embryologic/fetal development, opposing ridges of this tissue appear in the bulbus cordis and Truncus arteriosus. These smaller projections further undergo fusion to form the aorticopulmonary septum. TA occurs when this membrane wall fails to develop and divide the main arterial trunk into the aorta and the pulmonary trunk.
Truncus arteriosus Types
In 1949, Collett and Edwards developed the most well-renowned classification for this condition, known as the “Fourfold System”. The categorization for this condition is based on the branching pattern of the pulmonary arteries. As per this classification, TA is categorized into:
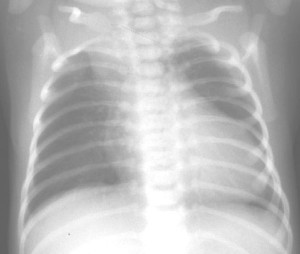
Picture 1 – Truncus arteriosus
TA Type 1
It is manifested by a short pulmonary trunk that arises from the truncus arteriosus, giving rise to left and right pulmonary arteries.
TA Type 2
In this form, two pulmonary arteries branch out from the posterior or posterolateral (on the side and toward the posterior aspect) side of the truncus arteriosus.
TA Type 3
Each pulmonary artery arises from the left and right lateral aspect of the truncus arteriosus.
Earlier, there existed a Type 4 form of this disorder. It is currently considered as a form of pulmonary atresia, a congenital malformation of the pulmonary valve with a defective valve orifice. It is no longer a part of the above classification.
Truncus arteriosus Incidence
The condition occurs in one out of every 10,000 live births. It accounts for approximately 1% of all cases of congenital heart disorders.
Truncus arteriosus Symptoms
In this condition, an array of symptoms develops in the first few weeks of the life of affected infants. However, each individual may experience different symptoms that often tally with other medical conditions of the heart.
Cyanosis
Abnormal blue or purple coloration of the skin and mucous membranes, due to lower levels of oxygen in blood, is a common characteristic of this condition. It generally appears first on the lips, tongue and fingernails of the newborns.
Hypocalcemia
Low concentration of calcium in blood may affect the nervous system, causing muscle cramps, abdominal cramps and rickets.
Heart failure
Inefficiency of the heart to pump sufficient blood to the body tissues may lead to a number of fatal consequences, including death.
Cardiomegaly
In this condition, the heart often gets abnormally enlarged. It appears quite bigger in size and is different from a normal heart.
Tachypnea
It is a respiratory condition where newborns undergo rapid breathing shortly after delivery. Whereas the respiratory rate is 40-60 times per minute in normal people, it is comparatively higher in individuals with this condition.
Biventricular hypertrophy
In this disorder, the right and left ventricles of the heart increase excessively in size. In most cases, however, left ventricular hypertrophy is more common.
Bounding arterial pulses
The disorder is most often characterized by a leaping and forceful pulse in the arteries located close to the skin.
Loud second heart sound
Normal heart sounds, referred to as “lub” and “dub”, generally occur in a sequential cycle with each heartbeat. These are called the “First Heart Sound” and “Second Heart Sound”, owing to the closing of the aortic and semilunar valves during pumping. In this congenital malformation, however, the intensity of the second heart sound is unusually higher and sharper.
Diaphoresis
Affected individuals may sweat profusely even under normal conditions.
Dyspnea
Deficiency of oxygen in the blood causes acute shortness of breath.
Fatigue
Chronic tiredness occurs when the muscles and tissues of the body receive less amount of oxygenated blood, causing extreme exhaustion and lethargy.
Mid-systolic ejection murmur
It is a noise caused by the turbulence of blood flowing through the semilunar valves that have undergone structural changes.
Poor feeding
Infants with this form of cardiac defect may experience difficulties in being fed or receiving the proper quantity of nutrition that leads to poor weight gain.
Truncus arteriosus Causes
In most cases, the cause of this congenital condition is generally unknown. But there are certain factors that may increase the chances of this rare condition such as:
Viral sickness during pregnancy
Rubella is a viral infection of the skin, causing rashes, especially in pregnant women. Affected women pass this infection to their babies while still in the womb. There are also other forms of viral infection that may develop in the early pregnancy period and affect the fetus.
Genetic disorders
DiGeorge syndrome is caused by the deletion of chromosome 22 that may lead to a host of congenital heart disorders.
Neural crest cells are a group of transient, multipotent, and migratory cells that usually give rise to a diverse cell lineage such as smooth muscles, melanocytes and peripheral neurons. Aorticpulmonary septum develops from cardiac neural crest that separates the aorta and pulmonary arteries. This in turn fuses with the interventricular septum during development of the heart. Genetic abnormalities in this group of cells may give rise to TA.
Teratogens
Development of the fetal heart may get affected if pregnant women are directly exposed to various forms of pharmacological and industrial agents.
Alcohol intake
Excessive consumption of alcohol can cause a wide range of physical birth defects including heart malformations of this type.
Gestational diabetes
It is a temporary condition that generally goes away post-delivery. However, newborns are at a greater risk of developing cardiac abnormalities due to this disease.
Wrong medications
Certain non-prescribed medications, administered at the time of pregnancy, have potential risks that may cause malformations of various parts of the developing fetus including the heart, limbs and, facial features.
Truncus arteriosus Diagnosis
Midsystolic murmur in the heart can be easily detected by physicians using a stethoscope during a thorough physical examination. Diagnostic techniques generally vary according to the age and clinical condition of the patients. Some of the tests usually recommended for confirming the condition include:
X-ray
A radiograph of the chest can demonstrate the size and structure of the heart as well as any form of lung abnormalities arising during this condition.
Echocardiogram
In this ultrasound test, high-pitched sound waves are used to view the entire anatomy of the heart for any kind of malformation in the valves and chambers.
Electrocardiogram (ECG or EKG)
Electrical activity of the heart is measured using this method. Abnormal rhythms could indicate some sort of malfunctioning of the heart due to decreased flow of blood.
Cardiac catheterization
It is an invasive procedure in which a small, thin, flexible tube (Catheter) is inserted into a chamber or vessel of the heart. A special contrast dye is injected to visualize the internal structures of the heart and to check the blood flow and pressure in the chambers.
Cardiac Magnetic resonance imaging (MRI)
It is another non-invasive technique that gives detailed images of the heart and the major blood vessels that aid physicians to detect any congenital abnormality in infants.
Truncus arteriosus Treatment
Surgical correction of the cardiac defect is the only recommended treatment for this disorder. In some cases, multiple surgical interventions are essential to completely cure the condition. The medical history, age, extent of the condition, and level of tolerance of an affected infant should be known before initiating the appropriate treatment.
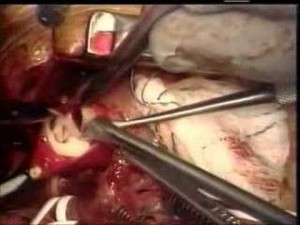
Picture 2 – Truncus arteriosus Image
Pre-operative medication management
Medications are generally prescribed before proceeding with the cardiac surgery. Some of the commonly administered antidotes include:
Digoxin
It strengthens the cardiac muscles for efficient pumping of the blood.
Diuretic
It removes excess fluids from the body in the form of urine, to maintain the balance of water in the body.
ACE (angiotensin-converting enzyme) inhibitors
These drugs decrease high blood pressure by dilating the vessels that enable better pumping of the heart.
Surgical repair
Cardiac experts usually opt for surgery when affected infants are 2 weeks old. The surgical procedure comprises of the following steps:
- The pulmonary arteries are detached from the Truncus arteriosus, which is the common artery.
- Next, these are connected to the right ventricle using a homograft – which is a part of the pulmonary artery with intact valves. A conduit or tunnel could also be used instead of a homograft.
- Finally, the Ventricular septal defect is closed with a patch.
Truncus arteriosus Prognosis
Nearly 65% of untreated patients of TA die within the first year of life. Surgical repair of the congenital defect, performed within the first 6 months of life, may improve the outcome.
Proper medical management of TA can prevent possible serious complications in future, including pulmonary hypertension and leaky heart valves. If any child in your family exhibits any of the symptoms of this condition, it is essential for you to immediately consult a good health care professional for timely diagnosis and treatment.
References:
http://emedicine.medscape.com/article/351490-overview
http://en.wikipedia.org/wiki/Persistent_Truncus_Arteriosus
http://www.cincinnatichildrens.org/health/t/truncus/
http://www.definition-of.net/truncus+arteriosus