Mullerian Agenesis Definition
Page Contents
Mullerian Agenesis (MA) is defined as a hereditary malformation in the genital tract of the female reproductive system, characterized by the absence of uterus and deformity of the vagina. Females affected with the disorder lack normal menstrual periods and are generally unable to carry pregnancy. The disease often leads to primary amenorrhea.
This female reproductive disorder is known by various names including:
- Mullerian Duct Anomalies
- Mayer-Rokitansky-Küster-Hauser(MRKH)
- Mullerian Aplasia
- Vaginal Agenesis
Mullerian Agenesis ICD9 Code
The ICD9 code for this medical condition is 626.
Mullerian Agenesis Incidence
MA is said to occur in 1 in every 5000 women in the US. It is considered to be the second most significant reason for irregular periods among young females. Around 12% of such patients suffer from spine abnormalities. Around 15% of the women suffering from MRKH have urinary system defects. Such patients have normal hormones and ovaries and can attain pregnancy with the help of a gestational carrier. MA is typically sporadic in nature. Female relatives of the affected individual are not susceptible to the disease.
Mullerian Agenesis Causes
The exact cause of the MRKH syndrome is still not known. However, medical practitioners suggest that such diseases occur due to the amalgamation of a number of environmental and genetic factors. The reproductive anomalies occur due to the shortened growth of the Mullerian duct. In most cases, MEKH occurs due to the heterozygous transformation of the WNT4 gene on chromosome 1p36. WNT4 gene on chromosome 1p36 is responsible for the growth of the paramesonephric duct of the female reproductive system. In the absence of this gene, the Mullerian duct is generally absent or deformed and never grows in the female reproductive system.
Mullerian Agenesis Symptoms
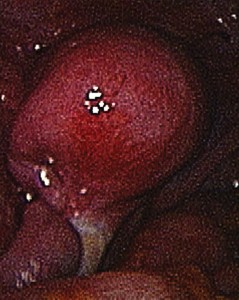
Females affected with MA are hormonally normal in nature. Such patients enter puberty with the growth of the body and experience painful intercourse due to shortened vagina. According to medical researchers, vagina, cervix and the uterus is partially or completed absent among patients affected with MRKH syndrome. The classical signs and symptoms of the disorder include:
Picture 1 – Mullerian Agenesis
- Lack of menstrual cycle during puberty
- Kidney problems
- Bone malformations
- Renal anomalies
- Hearing loss
Mullerian Agenesis Diagnosis
Among individuals whose karyotypic and hormonal examinations for amenorrhea are found to be normal, tests to confirm the diagnosis of MRKH syndrome are conducted through Laparoscopy or radiology. Birth disorders of the uterus can be easily detected by:
- MRI
- Ultrasound
- Sonohysterography
- X-ray
Mullerian Agenesis Differential Diagnosis
The differential diagnosis of MA includes distinguishing the signs of the disease from those of other conditions that give rise to similar warning signs. These include:
- 5-Alpha-Reductase Deficiency
- Androgen Insensitivity Syndrome
- Congenital Adrenal Hyperplasia
- Hermaphroditism
- Müllerian-inhibiting substance deficiency
- Turner Syndrome
Mullerian Agenesis Treatment
In women affected with MA, pregnancy cannot be made possible through any treatment. Affected women can give birth through IVF. This involves the transfer of embryo to a gestational carrier. Surgery or Vaginal dilators may allow penetrative sexual intercourse in a functional vagina.
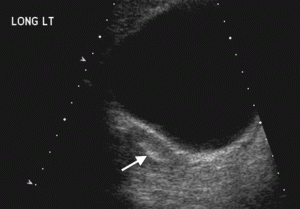
Picture 2 – Mullerian Agenesis Image
In the McIndoe procedure, an artificial vagina is formed with the aid of a skin graft. Following surgery, dilators are kept in order to prevent vaginal stenosis. The Veccihietti technique is a laparoscopic one which improves the vagina of an MA-affected woman so much as to make it comparable to a normal vagina. In this method, the surgery lasts for about 45 minutes.
Mullerian Agenesis Risk factors
The risks of recurrence in one family with this type of inheritance, is between 1-2%. Sisters have been found to be born with the same condition. However, relation of this disease to other factors like diet, work, environment, chemical exposure, drugs, radiation or infections have not yet been completely assessed.
References:
http://en.wikipedia.org/wiki/M%C3%BCllerian_agenesis
http://www.ncbi.nlm.nih.gov/pubmed/11023205